Germaphobes, cleaning zealots, neat freaks, and those with diagnosed or undiagnosed obsessive-compulsive disorder (OCD), this column is for you! If you would rather clean your bathroom floor than go for a walk on a beautiful sunny day, please read on. If you use a toothbrush on tile grout on a regular basis and take pride in the sparkle of your toilet bowl than beware… studies show that performing these tasks with too much vigor and passion might lead to back, neck, and shoulder and wrist pain.
For some, and you know who you are, (I am related to a few) spring cleaning can be a particularly exciting sporting event. It is almost an exorcism to rid a home of all its evil spirits, smudges, dust, dirt, germs, and odors. Every April curtains come off the windows to be washed and carpets rolled up, removed and cleaned. The surfaces under the curtains and carpets are sterilized with cleaning detergents, disinfectants and chemicals that would make sterile techniques in most hospital operating rooms seem inadequate. And that doesn’t include the heavy work: moving furniture, bedding, including mattresses and box springs.
As a physical therapist and survivor of childhood exposure to copious amounts of cleaning chemicals, I have come to learn that there are healthy and safe options for spring cleaning your home. Of course, the most obvious solution is to hire professional help if you can afford it. The other practical solutions are below:
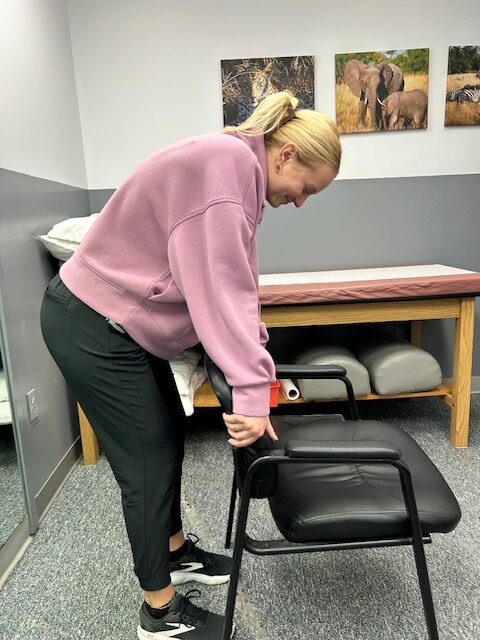 Incorrect
Incorrect 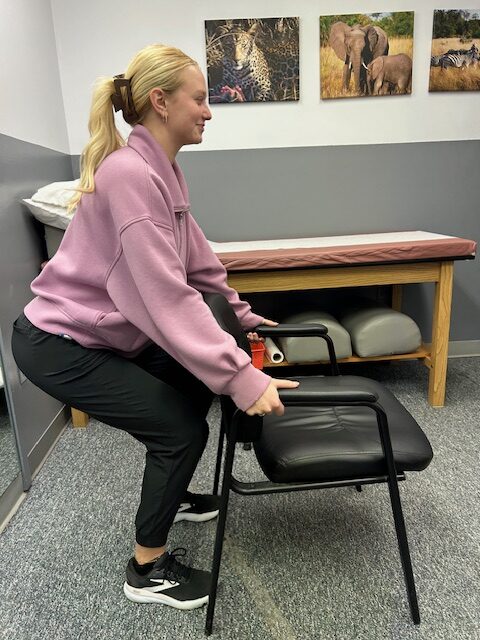 Correct
Correct Incorrect
Incorrect  Correct
Correct
Model: Hannah Keane, Physical Therapy Aide, Mackarey PT
Sources: National Center for Injury Prevention and Control at the CDC, www.medicinenet.comwww.household-management-101

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

What medical problems do a carpenter, typist, truck driver, jackhammer operator, violinist, pianist and court stenographer have in common? Carpal tunnel syndrome! Over the past 10-15 years, carpal tunnel syndrome has moved to the forefront in medicine and has become water cooler conversation. So, what is carpal tunnel syndrome and how is it treated?
Carpal tunnel syndrome (CTS) is a nerve disorder caused by compression of the median nerve at the wrist. The median nerve is one of three main nerves that provide sensation to the hand. This nerve specifically supplies sensation to the thumb, index, middle, and half of the ring finger. In CTS, compression on the median nerve occurs as it travels through a narrow passage in the wrist called the carpal tunnel. The carpal tunnel is formed by eight bones in the wrist (the floor of the tunnel) and the transverse carpal ligament, a strong ligament traveling across the roof of the tunnel. Within the tunnel there are nine tendons, which are a bit smaller than a pencil. These tendons share this space with the median nerve. In the case where there is swelling on the structures in the carpal tunnel, a person can experience pins and needles, numbness, and aching in the hand.
To be properly diagnosed, a physician will discuss your symptoms and medical history and examine strength and sensation. A nerve conduction study, electromyography (EMG), and x-ray may be ordered to provide information regarding sensation in the median nerve distribution and confirm compression at the carpal tunnel.
Treatment focuses on the causes. Therefore, treatment suggestions may include activity modification and postural changes during activities. Other suggestions may include frequent rest periods, elevation, and exercises or stretching. Wrist splints are effective in relieving compression at the carpal tunnel and are typically recommended for night wear. Appropriate fit of the splint is vital. Occupational and physical therapists or certified hand therapists can check the fit of prefabricated splints or can fabricate a custom splint. The above-mentioned treatments all focus on decreasing inflammation and compression on the median nerve.
Your physician may order pain relievers or anti-inflammatory medication. A cortisone injection into the carpal tunnel may also be recommended to assist with decreasing inflammation near the carpal tunnel.
A referral to an occupational or physical therapist or certified hand therapist may be made. A therapist can provide information regarding the diagnosis, appropriate treatment, and symptom reduction. They can make recommendations to introduce into daily activities to allow appropriate positioning of the upper extremities. A therapist will also instruct individuals on helpful stretching exercises or fabricate a wrist splint. Other treatments include ultrasound, iontophoresis, and massage. The focus of therapy is to introduce changes and interventions that reduce inflammation at the carpal tunnel to assist with symptom relief.
Surgery, referred to as a carpal tunnel release, may be indicated if symptoms are significant and impair functional activity performance.
To reduce your chances of getting CTS:
Guest Contributor: Nancy Naughton, OTD, CHT, is a Doctor of Occupational Therapy and certified hand therapist, specializing in the rehabilitation of the hand and upper extremity at Hand Surgery Associates, Olyphant, PA.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Farmers and gardeners in NEPA always say that Memorial Day, the “kick off” day for planting without the fear of frost, however, this year we have had an unusually cold and wet spring… but it is not too late to start…not only for the beds but your body! While gardeners are anxious to work in their gardens and enjoy the fruits of their labor, a relaxing and enjoyable activity can turn dangerous quickly. Precautions are necessary as repetitive stress injuries such as shoulder and elbow tendonitis and carpal tunnel syndrome can stem from raking, weeding, digging and pruning. Additionally, simple scrapes, blisters, and bites can turn into serious problems if not treated appropriately. Since prevention is the best approach, the American Society of Hand Therapists (ASHT) promotes warm-up exercises and injury prevention tips to help all levels of gardeners avoid serious and long-term injuries while enjoying this popular outdoor activity.
ASHT recommends following these upper extremity warm-up exercises prior to gardening:
Note: These exercises should never be painful when completing them. You should only feel a gentle stretch. Hold 10 seconds and repeat 5 times. Should you experience pain, please consult a physician or hand therapist.
ASHT recommends the following guidelines to prevent injury and foster healthy gardening practices:
Professional Contributor: Nancy Naughton, OTD, CHT, is an occupational therapist and certified hand therapist practicing in NEPA.

Next Week: “Prevention of Gardening Injuries” Part II of II.
EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Tennis elbow, also called lateral epicondylitis, is an inflammation of the lateral (outside) bony protuberance at the elbow. It is at this protuberance that the tendon of the long muscles of the hand, wrist and forearm attach to the bone. As the muscles repeatedly and forcefully contract, they pull on the bone, causing inflammation. The trauma is irritating when working the muscles in an awkward position with poor leverage like hitting a backhand in tennis.
It is not unusual for a patient to come to my office with severe pain on the outside of their elbow. Especially, after intensifying their tennis workouts or changing the racquet string tension. Others come to me with pain on the inside of the elbow (“golfer’s elbow”) from wrist action that advanced golfer’s use at impact. However, this problem is not only for tennis players and golfers. Laborers working with wrenches or screwdrivers with an awkward or extended arm can also develop tennis elbow. Others who are vulnerable are: those working for hours at a computer using a mouse as well as those working hard maintaining their lawns and gardens.
In a more chronic problem, lateral elbow pain may arise by a degenerative condition of the tendon fibers on the bony prominence at the lateral elbow. Sporadic scar tissue forms from a poor attempt by the body to overcompensate and heal without eliminating the cause.
While symptoms may vary, pain on the outside of the elbow is almost universal. Patients also report severe burning pain that begins slowly and worsens over time when lifting, gripping or using fingers repetitively. In more severe cases, pain can radiate down the forearm.
Conservative treatment is almost always the first option and is successful in 85-90 percent of patients with tennis elbow. Your physician may prescribe anti-inflammatory medication (over the counter or prescribed). Physical/Occupational therapy, rest, ice, and a tennis elbow brace to protect and rest may be advised. Ergonomic changes in equipment, tools, technique and work-station may be necessary. Improvement should occur in 4-6 weeks. If not, a corticosteroid injection may be needed to apply the medication directly to the inflamed area. Physical therapy, range of motion, and stretching exercises may be necessary prior to a gradual return to activity. Deep friction massage can assist healing.

Exercises performed in a particular manner to isometrically hold and eccentrically lengthen the muscle with contraction.

New Conservative Treatment: Platelet-Rich-Plasma (PRP) is a new treatment for the conservative management of degenerated soft tissues that has recently received great media attention. In great part, due to its success in several high profile athletes. According to the Journal of the American Academy of Orthopaedic Surgeons,(JAAOS), platelet-rich plasma (PRP) is autologous (self-donated) blood with an above normal concentration of platelets. Normal blood contains both red and white blood cells, platelets and plasma. Platelets promote the production and revitalization of connective tissue by way of various growth factors on both a chemical and cellular level.
The actual PRP injection requires the patient to donate a small amount of their own blood. The blood is placed into a centrifuge (a machine that spins the blood at a high velocity to separate the different components of blood such as plasma, white and red blood cells), for approximately 15 minutes. Once separated, the physician draws the platelet-rich plasma to be injected directly into the damaged tissue. In theory, the high concentration of platelets, with its inherent ability to stimulate growth and regeneration of connective tissue, will promote and expedite healing.
Surgery for tennis elbow is only considered in patients with severe pain for longer than 6 months without improvement from conservative treatment. One surgical technique involves removing the degenerated portion of the tendon and reattaching the healthy tendon to bone. Recently, arthroscopic surgery developed to perform this technique. However, research does not support the value of one over the other at this point. Physical/occupational therapy is used after surgery. Return to work or athletics may require 4-6 months. More recently, a surgical technique using ultrasound to guide a needle to debride (clean) the area of scar tissue has been developed. If eligible for this procedure, the time required for healing, rehabilitation and return to activity is much shorter.
If you feel you suffer from tennis elbow, ask your family physician which of these treatment options are best for you.
Visit your doctor regularly and listen to your body.
EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy

This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!