Preventing a fall can not only save your independence but also your life! Preventing injuries from falls reduces the need for nursing home placement. Injuries from falls are the seventh leading cause of death in people over the age of sixty-five.
The following suggestions will assist you in minimizing your risk of a fall:
Following these helpful hints will keep you safe by preventing a loss of balance and a potential fall!
Contributor: Janet M. Caputo, PT, DPT, OCS
Medical Reviewer: Mark Frattali, MD, ENT: Otolaryngology /Head Neck Surgery at Lehigh Valley Health Network

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at GCSOM.
For all of Dr. Mackarey's articles, visit our exercise forum!
Northeastern Pennsylvania is home to a large elderly population and many of the medical problems we expect to see are age related. Dedicated medical practitioners are in constant search for new knowledge and information to prevent or delay many age-related problems. One of the most devastating problems associated with aging is the risk of falling and falling.
Loss of balance causes falls. Falls are a leading cause of injury and death. Thirty percent of women and thirteen percent of men over the age of sixty-five will fall. Twenty to thirty percent of these individuals suffer moderate to severe injuries. Preventing falls is not an easy task. A good understanding of the causes of loss of balance and knowledge of a few fall prevention suggestions can enhance your balance and reduce your risk of a fall.
The Falls Risk Self-Assessment below allows and individual to determine their risk of falling to take the appropriate steps for prevention and treatment. The next three weeks will be dedicated to this topic to educate and inform readers and their families to make good decisions.
The Falls Risk Assessment is from the Centers for Disease Control (CDC).
1. YES (2) NO (0)
2. YES (2) NO (0)
3. YES (1) NO (0)
4. YES (1) NO (0)
5. YES (1) NO (0)
6. YES (1) NO (0)
7. YES (1) NO (0)
8. YES (1) NO (0)
9. YES (1) NO (0)
10. YES (1) NO (0)
11. YES (1) NO (0)
12. YES (1) NO (0)
Add up the number of points for each YES answer. If you have scored 4 or more points you may be at risk for falling.
Accordingly, 0-1 = Low Risk; 1-2 = Moderate Risk; 3-4 = At Risk; 4-5 = High Risk; 5-6 = Urgent; > 6 = Severe
Low Moderate At Risk High Risk Urgent Severe
0 1 2 3 4 5 6 7 8
Listen to your body and talk to your doctor.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
Next Monday Part II of III on Balance Disorders and Falls Prevention
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate clinical professor of medicine at GCSOM.
For all of Dr. Paul's articles, check out our exercise forum!
When an older loved one sustains a serious injury it is traumatic for the entire family and mine is no exception. My grandmother and father enjoyed 90 wonderfully active years; however, their independence was lost the same way more than one-third of a million people lose their independence each year… hip fractures! As a doctor of orthopedic physical therapy, I feel remise that I could not prevent this from happening. What most of us fail to realize is that his fracture, like many, was more than just an orthopedic problem …it involves age, gender, diet, exercise, vision, leg strength, medications, environmental risks, and vestibular problems (inner ear problems effecting balance).
Injuries due to falling are a very common problem in the elderly. Hip fractures are the most common injury due to falling in the seniors. According to the American Academy of Orthopaedic Surgeons, each year more than 300,000 people are hospitalized for hip fractures in the United States. These fractures represent 72% of all fracture costs, totaling more than 12 billion dollars in 2005 and, not surprisingly, 90% occurred in those 65 and older. Most hip fracture patients who previously lived independently will require family assistance, home or long term care and 50% will require a cane or walker.
Several risk factors for hip fractures have been identified. While some factors are somewhat controllable and may improve bone quality, (diet, exercise, smoking, alcohol) others are not.
Vestibular or inner ear problems
Preventing a fall can not only save your independence but also your life! Preventing injuries from falls reduces the need for nursing home placement.
NEXT MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” Hip Fractures - Part II of II

This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at GCSOM.
For all of Dr. Mackarey's Articles visit: www.mackareyphysicaltherapy.com/forum
Northeastern Pennsylvania is home to a large elderly population and many of the medical problems we expect to see are age related. Dedicated medical practitioners are in constant search for new knowledge and information to prevent or delay many age-related problems. One of the most devastating problems associated with aging is falling.
Loss of balance causes falls. Falls are a leading cause of injury and death. Thirty percent of women and thirteen percent of men over the age of sixty-five will fall. Twenty to thirty percent of these individuals suffer moderate to severe injuries. Preventing falls is not an easy task. A good understanding of the causes of loss of balance and knowledge of a few fall prevention suggestions can enhance your balance and reduce your risk of a fall.
The Falls Risk Self-Assessment below allows an individual to determine their risk of falling AND take the appropriate steps for prevention and treatment. The next three weeks will be dedicated to this topic to educate and inform readers and their families to make good decisions.
The Falls Risk Assessment is from the Centers for Disease Control (CDC).
WHAT IS YOUR RISK OF FALLING?
Add up the number of points for each YES answer. If you have scored 4 or more points you may be at risk for falling. Accordingly, 0-1 = Low Risk; 1-2 = Moderate Risk; 3-4 = At Risk; 4-5 = High Risk; 5-6 = Urgent; > 6 = Severe
Low Moderate At Risk High Risk Urgent Severe
0 1 2 3 4 5 6 7 8

NEXT MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” Next Monday Part I of III on Balance Disorders and Falls Prevention
Read all of Dr. Mackarey's articles at https://mackareyphysicaltherapy.com/forum/
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate clinical professor of medicine at GCSOM.
Preventing a fall can not only save your independence but also your life! Preventing injuries from falls reduces the need for nursing home placement. Injuries from falls are the seventh leading cause of death in people over the age of sixty-five.
The following suggestions will assist you in minimizing your risk of a fall:
Following these helpful hints will keep you safe by preventing a loss of balance and a potential fall!
Medical Reviewers: Mark Frattali, MD, ENT at Delta Medix, Division Chairman Otolaryngology – Head Neck Surgery at Commonwealth Health Regional Hospital

NEXT MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!”
Read all of Dr. Mackarey's articles at https://mackareyphysicaltherapy.com/forum/
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at GCSOM.
2nd of 3 Columns on Balance Disorders and Falls Prevention
Last week we discussed the causes of balance loss. Today, we will discuss treatment for this problem. Two primary treatments are medication and vestibular rehabilitation.
Medication for dizziness and loss of balance requires a visit to your family doctor. In a more involved case, your family physician may refer you to a specialist such as an ear, nose and throat physician or neurologist. There are many medications available for loss of balance. While this can be complicated, the specialist will determine the most appropriate one for your balance disorder.
Vestibular rehabilitation for dizziness and loss of balance is a great adjunct to medication to manage your balance disorder. It is a comprehensive program that addresses a wide range of problems that may cause imbalance such as: addressing the inability to tolerate motion, visual changes, providing balance rehabilitation, instruction in repositioning techniques for BPPV (benign paroxysmal positional vertigo), correcting postural dysfunctions, muscle weakness, joint stiffness, offering education for prevention, maintenance and self care after discharge. Through experience and motion, vestibular rehabilitation allows: formation of internal models (one learns what to expect from ones actions), learning of limits (learning what is safe and what is not) and sensory weighting (one sense, either vision, vestibular or somatosensory is selected in favor of another in maintaining balance).
In some minor cases, vestibular rehabilitation may be performed at home. However, more serious cases may require an evaluation by a physician specializing in the dizzy patient such as an ear, nose and throat physician or neurologist. These specialists will determine the nature of your problem and may enroll you in a more structured program under the direction of a physical therapist. Vestibular rehabilitation addresses not only vertigo (i.e. dizziness) but also balance problems.
Benign paroxysmal positional vertigo (BPPV) and vestibular hypofunction (e.g. unilateral and bilateral vestibular loss) are two causes of vertigo that can be addressed by a vestibular rehabilitation. Your physical therapist will tailor a program designed to address your specific vestibular disorder (i.e. BPPV or hypofunction).
If you have been diagnosed with BPPV, your therapist may take you through an Epley maneuver. In BPPV, particles in the inner ear become displaced and get lodged in an area that produces vertigo. Vertigo is experienced with tilting head, looking up/down and rolling over in bed. The causes include: infection, head trauma and degeneration. During the Epley maneuver the patient is guided through positional changes which clear these particles from the symptomatic part of the ear.
If you have been diagnosed with either unilateral or bilateral vestibular hypofunction, your therapist will most likely design a program to “retrain” your vestibular system with special exercises, including:
If you have a vestibular problem that primarily manifests as loss of balance, exercises to stimulate your balance responses, strengthen your legs, and enhance your joint position sense may be helpful. These exercises encourage reliance on vestibular and/or visual input. The exercises are performed on unstable surfaces (i.e. tilt boards, balance beams, and foam) and include a variety of tasks from simple standing to more complex arm and leg movements requiring coordination.
In addition to the above mentioned treatments, Posturography and Virtual Reality Training are computerized programs that may be used by your therapist to address your vestibular and/or balance problem. Also, Recreational Activities that involve using your eyes while head and body is in motion (i.e. dancing, golfing, tennis, walking while looking from side to side) are shown to be helpful in stimulating balance and vestibular responses. Furthermore, you may consider Alternative Balance Activities (i.e. Yoga, Tai Chi, Pilates) which incorporate slow gentle movements to improve strength, balance and posture as well as relaxation techniques for the anxiety that accompanies dizziness/off-balance.
Whatever you do, just DO NOT give into your dizziness. People that just “give up” become sedentary. A sedentary lifestyle further denies your body the necessary stimuli to challenge your vestibular system and make it stronger. Eventually, these people end up in a vicious cycle because the more they sit the dizzier and more off balance they get which only makes them sit more!
Remember, one fall increases your risk of another fall. It is imperative to determine what caused your fall and take action! Ask your physician or physical therapist to assess your fall risk.
Medical Reviewer: Mark Frattali, MD, ENT at Delta Medix, Division Chairman Otolaryngology – Head Neck Surgery at Commonwealth Health Regional Hospital

NEXT MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” Next Monday Part III on Balance Disorders and Falls Prevention
Read all of Dr. Mackarey's articles at: https://mackareyphysicaltherapy.com/forum/
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate clinical professor of medicine at GCSOM.
1st of 3 Columns on Balance Disorders and Falls Prevention
Northeastern Pennsylvania is home to a large elderly population and many of the medical problems we expect to see are age related. Dedicated medical practitioners are in constant search for new knowledge and information to prevent or delay many age related problems. One of the most devastating problems associated with aging is falling. It will be the purpose of this series of three columns to educate readers about the risks and causes of falling and the prevention and treatment of balance disorders.
Loss of balance causes falls. Falls are a leading cause of injury and death. Thirty percent of women and thirteen percent of men over the age of sixty-five will fall. Twenty to thirty percent of these individuals suffer moderate to severe injuries. Preventing falls is not an easy task. A good understanding of the causes of loss of balance and knowledge of a few fall prevention suggestions can enhance your balance and reduce your risk of a fall.
The causes of loss of balance which may lead to a fall are divided into three categories: age related changes, medical conditions and medications.
Age Related Changes affecting the sensory system, the musculoskeletal system as well as psychological behavior can negatively impact balance causing a fall:
Medical Conditions can also cause loss of balance increasing the risk of a fall:
Medications can also negatively effect balance and increase the risk of falls. Interactions between medications as well as the side effects of certain medications can cause dizziness or drowsiness resulting in loss of balance. Theses medications include: tranquilizers, sedatives, anti-depressants, alcohol, diuretics, blood pressure medications, cardiac medications, laxatives and pain killers.
In conclusion, determining who is at risk for a fall is a complex task since many factors including age, disease and medication can affect the outcome. Early intervention to prevent a fall can avoid many costly consequences.
Medical Reviewer: Mark Frattali, MD, ENT at Delta Medix, Division Chairman Otolaryngology – Head Neck Surgery at Commonwealth Health Regional Hospital

NEXT MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” Next Monday Part II on Balance Disorders and Falls Prevention
Read all of Dr. Mackarey's Articles at: https://mackareyphysicaltherapy.com/forum/
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate clinical professor of medicine at GCSOM.
This column is written at the request of Kathryn Sarrides, an exceptionally spry senior who lives happily in Green Ridge with her sage husband, Harry. They, like many their age, work hard to maintain their independence by engaging in physical activity and exercise as well as intellectual stimulation by playing bridge, reading books and staying socially active. Last week, Kathryn came to me with a very common problem among octogenarians and nonagenarians… she was concerned about her safety getting out of a chair, especially a chair that did NOT HAVE ARMS!
Falls are a leading cause of injury and death in seniors. Thirty percent of women and thirteen percent of men over the age of sixty-five will fall. Twenty to thirty percent of these individuals suffer moderate to severe injuries. While preventing falls is not an easy task, there are a few things to consider that may go a long way!
The National Institute of Health (NIH) recommends four areas of concentration for elderly persons to concentrate on in order to maintain safety and independence: strength, flexibility, balance and endurance. It will be the purpose of this column to recommend safe and practical tips to get out of a chair and exercises to keep you strong and limber enough to do it safely.
1. Scoot Your Butt to the edge of the chair
2. Tip Your Trunk Forward – over your bent knees
3. Push Off the Arms of the Chair – while leaning forward
4. IF THE CHAIR HAS NO ARMS – Place one hand on the chair seat and the other hand on your knee. Then push up with your arms (SEE PHOTO A)
5. Push From your Legs – at the same time you push with your arms
6. Stay Still Standing – for a few seconds after You get up …before you walk

Strength Exercises involve using the muscles to move the arms and legs against resistance such as a weighted object, dumbbells, resistance bands, and body weight against gravity. Strength is necessary to perform daily activities such as: getting out of a chair, walking, lifting a half-gallon of milk, transferring to/from a shower safely.
These exercises are performed while sitting in a chair with backrest, slowly, 5 -10 repetitions, and 3-5 times per week. No weight is used in the beginning, only the weight of the arm against gravity. In 1-2 weeks a light 1-2 pound weight and light resistance band may be added.
Do these exercises while sitting in a chair with a backrest:
Chair Push-Ups – While sitting in a chair with arm rests, perform a push-up by pushing off the arms while pushing with your legs (PHOTO B)
Shoulder Shrug – shrug top of shoulders up toward the ears
Row the Boat – pull both arms back at a 45 degree angle with bent elbows as if “rowing a boat”
Elbow Bend/Extend – bend and straighten elbows

Do these exercises while sitting in a chair with a backrest:
Hip Hike – lift hip up 2-4 inches as if “marching” (PHOTO C)
Hip Spread – with heels on the floor, spread knees apart
Hip Squeeze – with heels on the floor, squeeze knees together
Leg Kicks – extend knee as if kicking the foot forward and up
Heel Raise – raise heel up with toe on floor
Toe Raise – raise toes up with heel on floor
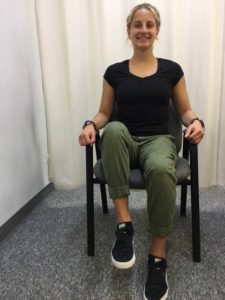
Do these exercises while Standing. Always hold onto a counter top or the back of a stable chair:
Standing Leg Curl – facing and holding onto the countertop (chair), bend the knee by bringing the foot back (PHOTO D)
Standing Hip Hike - facing and holding onto the countertop (chair), hike hip up as if marching (PHOTO E)
Standing Squat – facing and holding onto the countertop (chair), bend both knees to a 20-30 degree angle. Hold this position for 5-10 seconds.
Once you have mastered these exercises against gravity, then advance to using light weights or light resistance bands. Ankle weights are very inexpensive and can be purchased in 1 pound increments. Light resistance bands are available in yellow and red in colors.
Visit your doctor regularly and listen to your body.
Keep moving, eat healthy foods, exercise regularly, and live long and well!


Read Dr. Mackarey’s "Health & Exercise Forum" every Monday in the Scranton Times-Tribune.
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine.