November is National Alzheimer’s Disease Awareness Month. It is appropriate that it is also National Family Caregivers Month, since many people afflicted with Alzheimer’s are physically well and often rely on caregivers. It would be very unusual to find a person whose life has not been affected by someone with Alzheimer’s disease (AD). AD is a form of dementia. It is sometimes referred to as Senile dementia/Alzheimer’s type (SDAT). Currently, more than 4 million people in the USA have AD. Approximately 10% of all people over 70 have significant memory deficits. The number doubles each decade after 70. The risk increases with age and family history for the disease.
AD is a progressive degenerative disease of the brain that affects memory and thought process. Memory impairment is the hallmark of this disease. Also, those suffering from AD present changes with the following: language, decision-making, judgment, attention, and other personality or aspects of mental function. AD progresses differently in each case.
Two types of AD have been identified, early onset and late onset. In early onset, symptoms appear before the age of 60 and progress very rapidly. It accounts for 5-10% of all cases. Autosomal dominant inherited mutations have been found in early onset AD.
The cause of AD is not completely understood; however, most experts agree that both genetic and environmental factors are involved. It is important to rule out other medical causes before a final diagnosis of AD can be made. Only a post-mortem microscopic examination of brain tissue can confirm the diagnosis. Structural and chemical parts of the brain disconnect as the brain tissue shows twisted fragments of protein that clogs up the nerve. Clusters of dead and dying nerve cells block the transmission of information and communication from one nerve cell to the next. AD causes a disconnection of areas of the brain that normally work together.
The Greater Boston Physicians for Social Responsibility and the Science and Environmental Health Network offer the following guidelines to reduce the Risk of Developing AD:
Source: The HealthCentralNetwork, Inc

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

October is National Breast Cancer Awareness Month and there is good news to report!
A recent study in the Journal of the American Medical Association from Harvard has found that regular exercise can improve the survival of patients with breast cancer. I have discussed these findings with local physician, Dr. Christopher Peters of Northeast Radiation Oncology Center and he says that he regularly councils his patients about the value of exercise in the recovery from breast cancer. As found in the study, he recommends aerobic exercise such as walking and/or biking and mild resistance exercise. He also encourages patients to enroll in a formal rehabilitation program, especially to prevent a frozen shoulder if invasive surgery was performed.
Previous studies have shown many benefits of exercise for breast cancer patients including improving immune functioning and controlling depression. However, new research recently presented at the American Association for Cancer Research annual meeting was the first report to conclude that physical exercise may improve survival in breast cancer patients. Additional studies have shown other benefits of exercise. For example, a study conducted at Vanderbilt University found that women who had high activity levels throughout life were less likely to develop endometrial cancer. At the Hutchinson Cancer Research Center in Seattle, researchers found that exercise with moderate intensity can reduce serum markers of inflammation (C-reactive protein), which, when elevated, are associated with chronic disease and poor cancer survival.
In the current study, conducted at Harvard University, researchers compared survival rates in women with breast cancer with exercise levels in terms of metabolic equivalent (MET) hours per week. While women with high activity levels of exercise had the best outcomes, even women with moderate exercise benefited.
Benefits of exercise in women with breast cancer:
In conclusion, current research supports the fact that exercise may improve breast cancer survival. The following guidelines are proposed:
Flexibility Exercises involve moving the arms, legs and trunk through comfortable range of motion to give you more mobility in order to improve your ability to perform daily activities such as tucking in a shirt, tying shoes or fastening a bra. Best if performed after strength exercises because the muscles and joints will be warm and limber. Always perform slowly with slight stretch sensation and no pain. No bouncing or overstretching!
These exercises are to be performed while sitting in a chair with a backrest, slowly, 5 repetitions, 3-5 times per week.
Balance Exercises involve strengthening muscles that keep the body upright and stable in standing in order to improve your ability to perform daily activities without falling. According to the NIH, 300,000 US hospital admissions for broken hips occur each year due to falls. Check with your physician if you have a history of dizziness before performing these exercises on your own. Best if performed with someone at home or some assistance. Always use a countertop or back of chair to hold onto for support.
Endurance Exercises involve any activity such as walking, swimming, biking or raking leaves that elevates your heart rate and breathing for an extended period of time. Check with your physician if you have a history of heart problems or dizziness before performing these exercises on your own. Best if performed with someone at home or some assistance. Start off slowly for only 5 minutes and add 1-2 minutes each week or 2. Wear good and comfortable shoes – no heels!
While not all of these endurance exercises may be appropriate for you, one or two of these may offer a good starting point.
Visit your doctor regularly and listen to your body. Keep moving, eat healthy foods, exercise regularly, and live long and well!

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

October is National Physical Therapy Month! The American Physical Therapy Association (APTA) would like to recognize the thousands of physical therapists as dedicated health care providers. Moreover, physical therapists would like to thank the public for allowing us to participate in your health and wellness. While PT’s may not save lives…we do save LIFESYLES!
This column will address a question that is frequently asked by people of all ages and activity levels…stretching. First, it is important to keep in mind that stretching should NEVER be performed without warming up your body and muscles first. This can be done by running slowly in place or around the block for 5-10 minutes. Second, stretching should NEVER be painful. Third, a good stretch should be performed slowly and feel like slight tension in the muscle. NEVER bounce or jerk. First, perform the stretches by actively moving your muscles slowly and deliberately 5-10 times. Then, hold the stretch for 5-10 seconds, repeat 5-10 times, 2-4 times per week.
Remember, flexibility is only one aspect of complete health and wellness. Strength training, cardiovascular fitness, meditation and stress management and proper nutrition are also necessary for a healthy lifestyle. Also, be careful not to overstretch before competition as it may weaken the muscle.

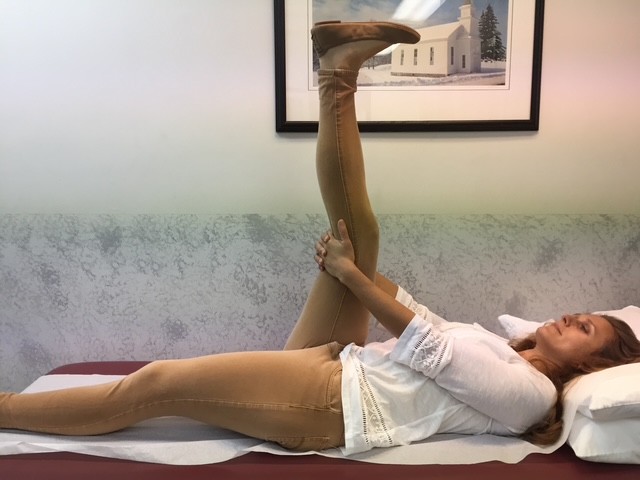

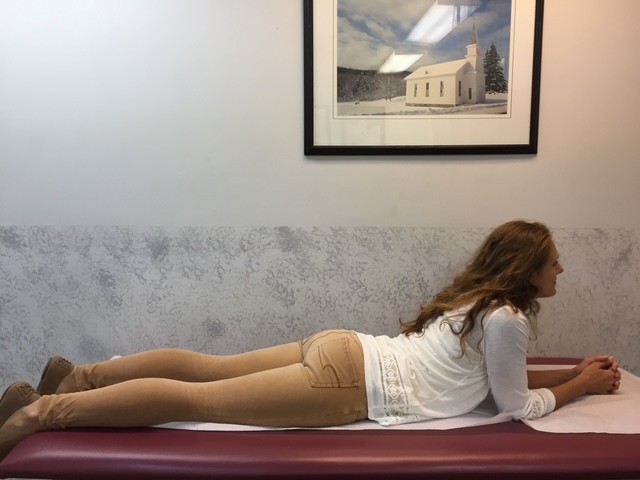

MODEL: Sarah Singer, PTA, Mackarey Physical Therapy

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

It is two weeks away from the 28th Steamtown Marathon. After training all spring and summer for the first seven Steamtown Marathons, not a Columbus Day Weekend goes by without my thoughts of this great event.
I would like to introduce this topic with some marathon history. In 490 B.C. Athens was under attack by the Persians and was outnumbered more than two to one. The Athenians fought bravely and defeated the enemy in the town of Marathon. The victory kept the intruders 26 miles away from Athens. To keep the anxious citizens of Athens calm, leaders immediately ordered a foot soldier, Phedippides, to run to the capital city to share the news. Phedippides ran, in full armor, for 26 miles from Marathon to Athens, delivered the message and died immediately. Now, people do the same thing of their own free will!
Each year at this time, dozens of runners preparing for the Steamtown Marathon come to my office with severe shin pain known as shin splints. Unfortunately, in many of these athletes, this problem can lead to a much more severe and advanced problem with shin splints called a stress fracture.
A stress fracture is fatigue damage to bone with partial or complete disruption of the cortex of the bone from repetitive loading. While standard x-rays may not reveal the problem, a bone scan, and MRI will. It usually occurs in the long bones of the leg, mostly the tibia but also the femur (thigh) and foot. Occasionally, it occurs in the arm.
10-21% of all competitive athletes are at risk for stress fractures. Track, cross country and military recruits are at greatest risk. Females are twice as likely as males to have a stress fracture. Other athletes at risk are: sprinters, soccer and basketball players, jumpers, ballet dancers are at risk in the leg and foot. Gymnasts are also vulnerable in the spine while rowers, baseball pitchers, golfers and tennis players can experience the fracture with much less frequency in the ribs & arm.
The problem is much more prevalent in weight bearing repetitive, loading sports in which leanness is emphasized (ballet, cheerleading) or provides an advantage (distance running, gymnastics).
Stress fractures usually begin with a manageable, poorly localized pain with or immediately after activity such as a shin splint. Over time, pain becomes more localized and tender during activity and then progresses to pain with daily activity and at rest.
Visit your doctor regularly and listen to your body.

Read Health & Fitness Forum Next Monday/Sunday: Preparing Your First Aid Kit For the Steamtown Marathon
EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Here are 10 most common exercise myths!

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

September is National Yoga Month! It is hard to believe that yoga, which is now a cultural mainstay, was once considered a foreign practice. An ancient discipline that totes numerous health benefits, it is meant to cultivate inner peace, enlightenment, and a strong relaxed body. In the past, only major cities housed yoga studios but over time it has spread into small towns across the country. Studios offer a variety of classes and each promotes their own unique philosophy. Whether you are looking for a new workout regime, compliment to your current program or simply to quiet your mind in a hectic world, yoga may be an option for you.
Yoga is a discipline that developed over 5,000 years ago and is generally recognized as an ancient system for wellbeing. The word yoga, from the Sanskrit word “yuj”, literally means to yoke or to bind together. The primary focus is to harmonize or unite the mind, body, and spirit through a combination of poses, breathing techniques, and meditation.
The specific origin of it is a topic of debate. However, it is said to have originated in India and was brought to the Western world by gurus in the late 19th and early 20th centuries. The basis for most current practices is The Yoga Sutras of Patanjali. In The Yoga Sutras, eight limbs of yoga are specified. The three most common limbs are meditation, pranayama or breathing exercises, and asana which are the physical poses. Classes can vary greatly, however, most classes include a combination of meditation, breathing exercises, and physical postures.
There are numerous styles of yoga. If you are a newcomer, deciding on a class may be difficult. It is always a smart idea to call a studio before attending a class to gain information and have any questions answered. Furthermore, if you have any health concerns you may want to consult your doctor prior to trying a new form of exercise. Some common forms include but are not limited to:
Below you can find a few common poses or asanas that can be found in beginner classes. These poses promote flexibility and strength and can be incorporated into your everyday workout routine. Remember, before you attempt the poses, begin by walking, biking or running to warm up. Don’t overstretch, perform slowly, and hold the position. You should feel mild discomfort NOT pain.





There are a lot of options when it comes to where to start to practice. It is important that the studio you choose employs certified yoga instructors who have completed comprehensive training. A good instructor can make all the difference in your experience. The studio should provide a clean environment and offer a variety of classes including beginner level if you are a newcomer. The best way to get a feel for a studio is to stop in for more information. You may want to ask about pricing as there are often discount introductory rates. Ask about rentals if you do not own a yoga mat and request to see the space. Some yoga studios have a strong sense of community while others are more like a gym. Try out a few different places until you find a fit for you.
Guest Columnist: Catherine Udomsak, PT, DPT | Model: Sarah Singer, PTA

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

September is National Yoga Month! It is hard to believe that yoga, which is now a cultural mainstay, was once considered a foreign practice. An ancient discipline that totes numerous health benefits, yoga is meant to cultivate inner peace, enlightenment, and a strong relaxed body. In the past, only major cities housed yoga studios but over time yoga has spread into small towns across the country. Studios offer a variety of classes and each promotes their own unique philosophy. Whether you are looking for a new workout regime, compliment to your current program or simply to quiet your mind in a hectic world, yoga may be an option for you.
Yoga is a discipline that developed over 5,000 years ago and is generally recognized as an ancient system for well-being. The word yoga, from the Sanskrit word “yuj”, literally means to yoke or to bind together. The primary focus of yoga is to harmonize or unite the mind, body, and spirit through a combination of poses, breathing techniques, and meditation.
The specific origin of yoga is a topic of debate. However, it is said to have originated in India and was brought to the Western world by yoga gurus in the late 19th and early 20th centuries. The basis for most current yoga practices is The Yoga Sutras of Patanjali. In The Yoga Sutras, eight limbs of yoga are specified. The three most common limbs are meditation, pranayama or breathing exercises, and asana which are the physical poses. Yoga classes can vary greatly, however, most classes include a combination of meditation, breathing exercises, and physical postures.
So what is with all the hype? Why has yoga become so popular? Many would say it is due to its numerous mental and physical health benefits. Research has shown that yoga, when practiced regularly, can reduces stress levels and even boost one’s immune system. Regular stretching releases tension in the body and the controlled breathing and mediation decrease anxiety. Studies show that those who practice yoga habitually can have decreased blood pressure and cholesterol making them less prone to heart disease. Other ailments which are shown to be positively impacted by yoga include insomnia, depression, and chronic pain including low back pain and headaches. Yoga is an excellent way to combat the negative effects of stress on the body and cope with anxiety and angst.
In addition to stress reduction, yoga has many physical benefits. These include increased flexibility, strength, and balance. Those who practice yoga regularly are often less prone to injury, such as a muscle strain or tear, due to their increased flexibility. Furthermore, yoga can be an effective way to strengthen one’s core which is crucial to maintaining ideal posture and protecting the back. For athletes, yoga can be a great way to challenge one’s balance and improve stability. In the elderly, it is a safe way to improve overall body awareness and decrease the risk of falling. Yoga has also been shown to improve respiration and many report an overall increase in energy when incorporating yoga into their lives.
With all of the positive impacts yoga has on the body it is easy to see why it has become such a popular form of exercise. There are classes to meet almost all needs and most poses can be modified based on ability. Yoga can be practiced by those of all ages and all fitness levels. Whether you’re looking for a way to loosen up tight muscles or you simply wish to quiet your mind for an hour, yoga is a tool to improve and maintain health. The only thing you need is a mat and an open mind.
Yoga can be practiced by anyone. From children to adults to the elderly, there are classes for all ages and abilities. It can be a form of cross training for athletes, especially runners who tend to have tight musculature. It also promotes balance and core stability which may be beneficial to sportspersons including football players, soccer players, boxers, etc. Furthermore, there are classes for the elderly which focus on balance and maintaining mobility. There are even prenatal yoga classes for pregnant women to promote deep breathing, flexibility and muscle tone.
Next Week: Types of Yoga and Basic Poses
Guest Columnist: Catherine Udomsak, PT, DPT

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
STAY TUNED for Yoga: TYPES OF YOGA AND BASIC POSES: Part II of II!
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Happy Labor Day! There is little doubt that the workplace has been redefined since the pandemic as many employees continue to work from home. Sitting for many hours at a workstation that may not be optimal has also changed the way we define workplace health and safety. It may be more important than ever to pay close attention to designing an ergonomic workstation, changing position, and stretching regularly to prevent injury.
Since 1894 Labor Day has been designated as the national holiday that pays tribute to the contributions and achievements of American workers. Research supports the notion that healthier employees are happier and more productive. When employers encourage healthy behavior and safety at work, they benefit in many ways.
For example, in addition to improving job satisfaction and productivity, healthy employees save money by using less sick time, worker’s compensation benefits and health benefits. For example, according to the Centers for Disease Control and Prevention, approximately 75 percent of employers” health care costs are related to chronic medical problems such as obesity, diabetes, high blood pressure, and high cholesterol. Deconditioned, overweight employees are more likely to suffer from these preventable conditions and are at greater risk for injury. Employers, please consider using this holiday as an opportunity to start a health promotion program at your workplace…have a health fair, offer healthy snacks, encourage walking, smoking cessation, exercising at lunch, and offer fitness club stipends.
Lower back pain, one of the costliest illnesses to employers, is one example of a problem which can be prevented with a good health and safety program. It is widely accepted in the medical community that the best treatment for lower back pain (LBP) is prevention. Keeping fit, (flexible and strong), practicing good posture, and using proper body mechanics are essential in the prevention of LBP. At our clinic, significant time and effort is spent emphasizing the importance of these concepts to our patients, employees, and the businesses we work with through industrial medicine programs. A comprehensive approach can produce significant reductions in LBP injuries through an onsite safety program which promotes education, wellness, body mechanics, lifting techniques, postural and stretching exercises and ergonomics.
As little as 10 extra pounds puts great stress on your lower back. It also makes it more difficult to maintain good posture. Eat well, exercise regularly and don’t smoke. Smokers have a much higher incidence of LBP and failure from lower back surgery.
Good posture is critical for a healthy back. When sitting, standing or walking maintain a slight arch in your lower back, keep shoulders back, and head over your shoulders. In sitting, use a towel roll or small pillow in the small of the back. Also, consider sitting on a physio ball, which promotes proper posture for part of the day.
Perform postural exercises throughout the day. Most of the day we sit, stand, and reaching forward and bend our spine. These exercises are designed to stretch your back in the opposite direction of flexion. Please perform slowly, hold for 3-5 seconds and repeat 6 times each 6 times per day.
Chin Tuck: Tuck your chin back to bring your head over shoulders.
Shoulder Blade Pinch: Pinch your shoulder blades together.
Standing Extension: While standing, put your hands behind back and extend lower back 10-20 degrees.
Good Body Mechanics and ergonomics are also important in the prevention of LBP. When lifting, think twice. Think about the weight, shape and size of the object. Think about where the object is going and the surface resistance of the floor. Does it require two people to lift? Can I safely lift that high or bend that low?
When bending to lift an object think about safety:
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
While I fully expect to be at the “butt end” of many comments for this column, I feel compelled to address this topic at the request of several patients. It seems that many geriatric physical therapists commonly encounter patients that suffer from constipation which limits their participation in rehabilitation. Ironically, research demonstrates that exercise and activity actually help relieve constipation.
The National Digestive Diseases Information Clearinghouse (NDDIC) reports that 3.1 million people in the United States suffer from constipation. The NDDIC further reports that this problem leads to almost 400,000 hospitalizations, 1.4 million visits to emergency rooms, 1 million prescriptions and 121 deaths each year. Constipation is defined by the Ohio University College of Osteopathic Medicine as three or less bowel movements per week. It is also estimated that more than 27 percent of the elderly are affected.
Severe constipation can result in immediate medical attention in some cases due to intestinal obstruction. In addition to infrequent bowel movements, some symptoms include: feeling poorly, weight loss, loss of appetite, abdominal distention and/or pain, and vomiting.
Healthy people must continue to keep active. Get into good exercise habits at a young age and continue through life. Maintaining a consistent schedule of eating and exercise is also helpful. Some simple suggestions for beginning an exercise program for prevention of constipation in the healthy population are:
Depending on your general health and ambulatory status, these endurance exercises may be appropriate for you. Therefore, consider one or two of the following as a good starting point:
IN CONCLUSION: KEEP MOVING YOUR BODY AND YOU WILL KEEP MOVING YOUR BOWELS!
Visit your doctor regularly and listen to your body.
Keep moving, eat healthy foods, exercise regularly, and live long and well!

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

PIAA fall sport teams will begin their official practices a soon – including double sessions for high school football. While a warm August may be a wonderful time of year to swim and kayak, it may not offer the best temperature and humidity for athletes playing football, soccer and other sports. One common problem these athletes suffer from is severe muscle cramping. Every year multiple players limp off the practice field in pain and many concerned players, parents and grandparents repeatedly ask me about the problem. What exactly is a muscle cramp? Why does it happen? How can it be prevented?
A muscle cramp is defined as an involuntary contraction or spasm of a muscle that will not relax. The tight muscle spasm is painful and debilitating. It can involve all or part of the muscle and groups of muscles. The most common muscles affected by muscle cramps are gastrocnemius (back of lower leg/calf), hamstring (back of thigh), and quadriceps (front of thigh). Cramps can also occur in the abdomen, rib cage, feet, hands, and arms. They can last a few seconds or 15+ minutes. They can occur once or multiple times. It can cause very tight spasms or small little twitches.
Although the exact cause may be unknown at this time, there are several theories why muscle cramps occur. According to the American Academy of Orthopaedic Surgeons, when a muscle is flexible and conditioned, the muscle fibers are capable of changing length rapidly and repeatedly without stress on the tissue. Also, overall poor conditioning or overexertion of a specific muscle leads to poor oxygen/carbon dioxide exchange and build up of lactic acid and cause a muscle spasm. Also, this process can alter muscle spindle reflex activity and stimulate the spinal cord to send a message to the muscle to contract. If uncontrolled this leads to cramps and spasm.
Muscle cramps are more common in hot weather due to loss of body fluids, salts, minerals, potassium, magnesium and calcium. This leads to an electrolyte imbalance which can cause a muscle to spasm.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
