NEPA has had its share or snow this winter…and the recent storm added plenty of the pretty white stuff for work and play. Much has been written about the dangers of snow shoveling for your heart. However, while not fatal, low back pain is the most common injury sustained while shoveling snow. Heart attacks are also more common following wet and heavy snow.
Snow shoveling can place excessive stress on the structures of the spine. When overloaded and overstressed, these structures fail to support the spine properly. The lower back is at great risk of injury when bending forward, twisting, lifting a load, and lifting a load with a long lever. When all these factors are combined simultaneously, as in snow shoveling, the lower back is destined to fail. Low back pain from muscle strain or a herniated disc is very common following excessive snow shoveling.
Sources: The Colorado Comprehensive Spine Institute; American Academy of Orthopaedic Surgeons
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

More than 65 million people, almost 30% of the population in the United States, are actively involved in providing 20 or more hours of care for a chronically ill, disabled, or aged family member or friend each week. As our population continues to age, this number is expected to grow rapidly.
The role of a caregiver is multifaceted and often involves tasks and skills beyond the education or comfort level of most providers. Some examples include; managing money, paying bills, shopping, cleaning, maintaining and repairing a home, dispensing and injecting medications, cleaning wounds, changing dressings, catheter management, bed baths, assisting in position changes, transferring from the bed to the chair, ambulation, stair climbing, bathroom assistance for toileting and showering and many other responsibilities. Consequently, a caregiver is often at risk for mental, spiritual and physical fatigue or breakdown. It is no surprise that depression, illness and injury often plague a caregiver and eventually, the caregiver is in need of a caregiver. One of the most common injuries suffered by a caregiver is back pain.
Lower back pain (LBP) is one of the most common problems in our society. Over 90% of all Americans will suffer from it at least once in their lives. It is generally agreed that prevention is the best treatment for LBP.
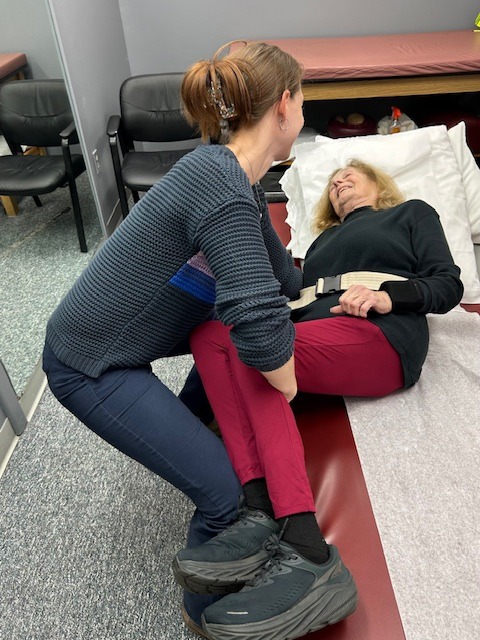
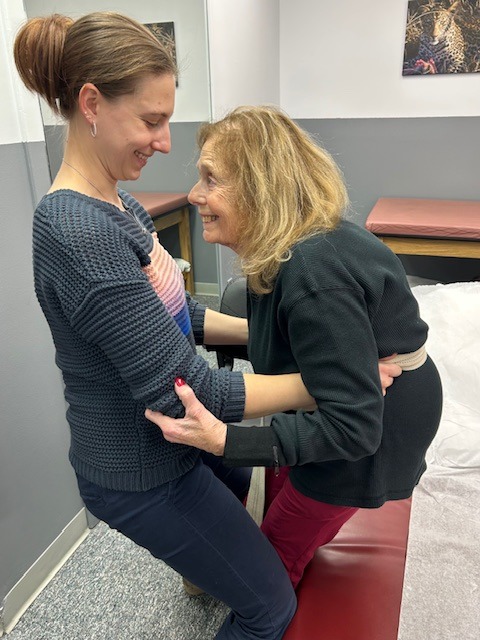
MODELS: Andrea Molitoris Kozlowski, PT, DPT, Associate Mackarey Physical Therapy, Doris Koloski, Scranton

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

I think we would all agree, technology is a wonderful thing. However, like all good things, it comes at a price. Students and workers alike are suffering from the many physical effects of sitting for too many hours. Studies show the impact of prolonged sitting, especially with proper posture, are multifaceted: pain, headaches, vision problems, poor concentration, excess fat storage with weight gain. Studies strongly support the use of good posture, ergonomic workstations, posture stretches, frequent changes of positions, including the use of standing desks to prevent pain and injury. In fact, standing desks are not a new invention; they have been used by many to promote health and stimulate thought…Hemingway, Franklin and Jefferson all stood while they worked.
The average head weighs 10 to 12 pounds and when tilted down at a 45 degree angle the forces of gravity are multiplied by 5. While reading, studying or working on the computer with poor posture, one must support 50 or more pounds of pressure on the neck, middle and lower back for hours on end. It is no wonder why this activity is associated with headaches, neck and back pain, numbness and tingling in arms and legs, muscle spasms etc. Some studies report the lifetime prevalence of neck and shoulder pain in office workers as high as 80%.
Recent research has also correlated the amount of time an individual sits to a decrease in their average life expectancy. Seriously, watching television and sitting is literally killing us. The Heart and Diabetes Institute of Australia conducted extensive research on sedentary behavior, including a review of almost one million people. They used actuary science, adjusted for smoking, waist circumference, and diet and exercise habits to assess the specific effects that the hours of sitting in a day impacts a person’s life span. They found that sitting too long results in a decrease in muscle contraction of the big leg muscles and because these unused muscles need less fuel, more unused glucose (fuel) is stored in the muscle. High glucose levels result in high blood sugar, which leads to adult-onset diabetes and other health issues.
The deleterious effects of sitting in children have also come under scrutiny and it may impact the classroom. Due to technology, today’s classroom is more advanced in many ways. However, the traditional hard chair and desk remain unchanged. Not only are these, “one size fits all,” desks uncomfortable, current research suggests that they may also limit learning.
Recent studies show that standing desks promote not only a physically healthier child by expending more calories and lowering obesity but also improves focus and concentration to improve academic outcomes.
Research from Texas A&M Health Science Center found two landmark things about children who worked at standing desks such as Stand2LearnR, when compared to those seated: One, children burned more calories and obese children burned more than normal-weight peers. Two, children were more attentive in the classroom and engaged more with their teacher and their work when allowed to stand. Teachers in the study not only found the results to be favorable for fidgety, high-energy kids, but those who tend to be overweight and tired benefited greatly.
Researchers were quick to point out that there may be many ways to promote movement and limit sitting in the classroom that may also promote learning in a healthy way such as sitting on exercise balls or inflatable discs.
The average office worker sits for more than 10 hours per day between office work, sitting at lunch, checking email and social media at home. Amazingly, studies suggest that even vigorous exercise before and after work cannot overcome the damage from prolonged sitting. New products such as the “TrekDeskR,” allows a worker to work on a computer, phone, or do paperwork, while walking on a treadmill, has great health value. Also, other products such as VariDeskR, allows for frequent positional changes from sitting to standing while working. Even without using a standing desk, changing positions, such as standing during phone calls or meetings has proven to be valuable. Current Wisdom: Alternate standing (30-45 minutes) and sitting (15-30 minutes)
Spine problems can be prevented with good posture and proper body mechanics. Poor posture and improper body mechanics subject the spine to abnormal stresses that, over time, can lead to degeneration and pain. Good posture and proper body mechanics and frequent changes in positions, can minimize current spine pain and prevent recurrent episodes. Posture is the position in which you hold your body upright against gravity. Good posture involves positions that place the least amount of stress on the spine. Good posture maintains the spine in a “neutral” position. In a neutral spine, the three normal curves are preserved (a small hollow at the base of the neck, a small roundness at the midback and a small hollow in the low back). When viewed from the side, the upper back appears straight with a small hollow in the lower back.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Recently, a young woman came to my office with complaints of severe middle and lower back pain. On her first visit, I noticed her beautiful pink purse (big bag) and asked her permission to weigh the bag and discovered that it weighed 8 pounds. While 8 pounds does not seem excessive, the woman weighed 120 pounds and based on the research, would be advised to carry a 2.5-to-3.5-pound bag, (2-3% of her body weight).
A recent study shows that the average weight of a woman’s purse has increased by 38% and now exceeds 6 pounds. Despite technological advances, women have not found a way to simplify their lives, or at least what they think they need in their lives. High tech gadgets have only added weight to a purse already filled to the brim.
On a whim, I decided to ask permission to examine the contents of some of my patient’s purses. A typical purse includes the following: hairbrush, cosmetic bag, mirror, feminine products, keys, and sunglasses, reading glasses, checkbook, wallet, coupons, water bottle, and medications. Additionally, I discovered heavy high-tech products such as cellular phones, tablets, digital Bluetooth earpieces, and rechargers. Lastly, some women add the weight of a book or Kindle to the bag. Studies also show that the larger the bag and stronger the straps, the more items are stuffed in, resulting in a very heavy purse.
It is a pervasive attitude that a woman should never be stranded without her purse full of essentials. So, where is the problem? The problem is that carrying a heavy bag, usually on one side of the body, forces the body to tilt forward and to the opposite direction to compensate. Over time, this change in posture leads to neck, middle and lower back pain.
Consider the following suggestions to promote healthy use of a purse and prevent injury:

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

While I normally do not address the topic of shoveling snow until January, considering recent weather events, I thought it might be valuable to present it sooner. Much has been written about the dangers of snow shoveling for your heart. However, while not fatal, low back pain is the most common injury sustained while shoveling snow. Heart attacks are also more common following wet and heavy snow.
Snow shoveling can place excessive stress on the structures of the spine. When overloaded and overstressed, these structures fail to support the spine properly. The lower back is at great risk of injury when bending forward, twisting, lifting a load, and lifting a load with a long lever. When all these factors are combined simultaneously, as in snow shoveling, the lower back is destined to fail. Low back pain from muscle strain or a herniated disc is very common following excessive snow shoveling.
Sources: The Colorado Comprehensive Spine Institute; American Academy of Orthopaedic Surgeons
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

While many people celebrate the Labor Day holiday by firing up the grill, others will be shopping to get their students ready for the school year. One item on the shopping list should be a good quality and well-fitted backpack…to prevent lower back pain!
In 2018, the government of India announced a ban on homework and recently in Poland; the government ministers did the same. Can you imagine…a ban on homework? In an effort to promote student health and address recent surges in the incidence of back pain in the young, there will be no homework for students in grades one and two.
It was estimated that the majority of students ages 7 – 13 in India were carrying almost half their body weight. Not surprisingly, medical practitioners noticed a dramatic increase in reported cases of back pain among this group and decided to take action. In addition to the homework ban for grades one and two, Indian authorities have also implemented a limit of 10% of the student’s body weight.
Back pain in students seems to be universal. Each year, as students in the United States prepare to return to school from summer vacation, the subject of backpacks arises. The good news: when compared to purses, messenger bags, or shoulder bags, backpacks are the best option to prevent lower back pain. The bad news is, most of the 40 million students in the USA using backpacks, are doing so incorrectly.
Studies have found more than 33% of children had LBP that caused them to miss school, visit a doctor, or abstain from activity. Also, 55% of children surveyed carried backpacks heavier than the 10-15% of their body weight, which is the maximum weight recommended by experts. Additionally, the study noted that early onset of LBP leads to greater likelihood of recurrent or chronic problems. Backpacks that are too heavy are particularly harmful to the development of the musculoskeletal system of growing youngsters. It can lead to poor posture that may lead to chronic problems.
The following information on backpack safely is based, in part, by guidelines from The American Physical Therapy Association. Parents and teachers would be wise to observe the following warning signs of an overloaded and unsafe backpack:
Consider the following suggestions to promote backpack safely and prevent back injury:

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Several years ago, while hiking to the bottom of the Grand Canyon with my family, my wife Esther developed “canyon knee,” also known as “hiker’s knee” or in medical terms, “patellar tendonitis.” Regardless of the term, the end result was that she had severe pain in the tendon below her knee cap and was unable to walk up the trail to get out of the canyon. In addition to ice, rest, bracing, and non-steroidal anti inflammatory medications, the National Park Ranger insisted that she use two trekking poles on her ascent to the rim.
Prior to that experience, I always thought that “walking, hiking sticks or trekking poles” were for show or those in need of a walking aide. Well, I could not have been more incorrect. Needless to say, Esther made it out of the canyon safely and, with the use of our life saving trekking poles; we have lived “happily ever after!” Now, 15 years later, I rarely walk more than 5 miles without my poles.
As a result of this experience, I have been recommending walking or trekking poles to my patients. These poles are an essential part of hiking or distance walking gear, for the novice and expert alike. Specifically, for those over 50 who have degenerative arthritis and pain in their lower back, hips, knees, ankles or feet, these simple devices have been shown to improve the efficiency of the exercise and lessen the impact on the spine and lower extremities. Additionally, using poles reduces the likelihood of ankle sprains and falls during walking. Trekking poles are also a safe option for those with compromised balance. If you want to walk distances for exercise and need a little stability but don’t want the stigma of a cane, trekking poles are for you.
Early explorers, Europeans and Native Americans have been using walking sticks for centuries. More recently, in the 1968 classic hiker’s bible, “The Complete Walker,” Colin Fletcher praised his “walking staff” for its multipurpose use: for balance and assistance with walking and climbing, protection from rattlesnakes, and for use as a fishing rod. Today, these sticks are now versatile poles made from light-weight materials.
Trekking poles are made of light-weight aluminum and vary in cost and quality. But, like most things, “you get what you pay for!” These hollow tubes can telescope to fit any person and collapse to pack in luggage for travel. Better poles offer multiple removable tips for various uses, conditions and terrains. For example, abasket to prevent sinking too deeply in snow, mud or sand; a blunt rubber tip for hard surfaces like asphalt or concrete, or the pointed metal tip to grip ice or hard dirt/gravel. Better quality poles offer an ergonomic hand grip and strap and a spring system to absorb shock through your hands, wrists and arms upon impact.
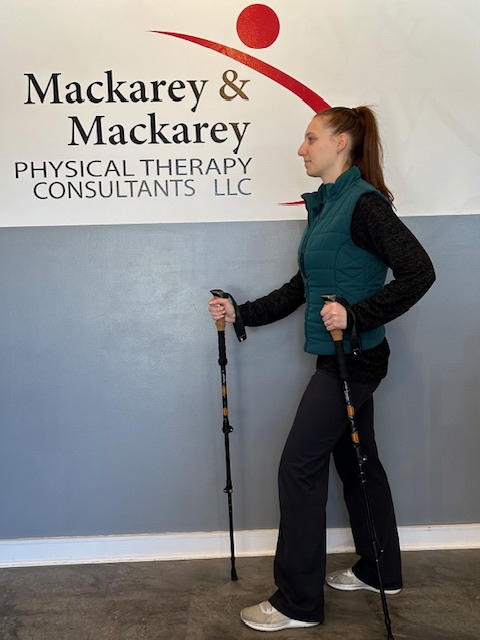
The poles should be properly adjusted to fit each individual. When your hand is griping the handle the elbow should be at a 90 degree angle. Proper use is simple; just walk with a normal gait pattern of opposite arm and leg swing. For example, left leg and right arm/pole swings forward to plant while the left arm/pole remain behind with the right leg .
This pattern is reciprocated with as normal gait advances (opposite arm and leg). I have been very pleased with my moderately priced poles (Cascade Mountain Tech from Dick’s Sporting Goods ($34.99 per pole). Prices range from $19.99 to 79.95 per pole. dickssportinggoods.com; montem.com; leki.com; rei.com. However, if you travel frequently to hike the State and National Parks, you may want to purchase more expensive poles that collapse and retighten more efficiently. (montem.com; leki.com;)
Montem Trekking Poles - with close-up of easy adjustable locking clasp.

There are numerous studies to support the use of trekking poles, especially research that supports their use for health and safety. One study compared hikers in 3 different conditions; no backpack, a pack with 15% body weight and a pack with 30% body weight. Biomechanical analysis was performed blindly on the three groups and a significant reduction in forces on lower extremity joints (hip, knee, and ankle) was noted for all three groups when using poles compared to those not using poles.
Another study confirmed that trekking poles reduced the incidence of ankle fractures through improved balance and stability. Additional studies support the theory that trekking poles reduce exercise induced muscle soreness from hiking or walking steep terrain and another study found that while less energy is expended in the lower body muscles using poles, increase energy is used in the upper body; therefore, the net caloric expenditure is equal as it is simply transferred from the legs to the arms.
In conclusion, it is important to remember that trekking poles for hiking or distance walking are much more than a style statement. They are proven to be an invaluable tool for health, safety and wellness by reducing lower extremity joint stress, improving stability and balance, and enhancing efficiency for muscle recovery.
Sources: Medicine and Science in Sports and Exercise. The Complete Walker, by Colin Fletcher
Model: Andrea Molitoris, PT, DPT at Mackarey Physical Therapy

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
In addition to lowering blood pressure, this gentle form of exercise can help maintain strength, balance, flexibility and mental health and is an ideal activity for all ages!
This research was brought to my attention by my friend and mentor from Dalton, Peter Frieder, Chairman,Gentex Corporation and current Board Chair at WVIA. Peter is celebrating his birthday today with a number of years that clearly does not represent his physiological age, in great part due to his dedication to health and wellness. Happy Birthday and thank you!
According to a new study by the China Academy of Chinese Medical Sciences (CACMS), the ancient martial art practice of Tai Chi is effective in lowering blood pressure as much, if not more, than traditional aerobic exercise. For those with prehypertension or hypertension and are unable to tolerate the repetitive and prolonged weight bearing stresses of running, walking or cycling, these results have tremendous implications. The slow, gentle and controlled movements and positions of Tai Chi coupled with controlled breathing and meditation may be a valuable alternative, especially for those with aging muscles and joints. Improved strength, flexibility balance, posture and mental health are additional bonuses.
Tai Chi is multifaceted in that it combines martial arts, slow gentle and controlled movements, sustained postures, a focused and meditative mind, and controlled breathing. It is considered by many to be “meditation or medication in motion.”
Tai Chi involves slow-motion movements transitioning with control from one position to another. The positions have historically been named for the actions of animals, for example:

Deep and purposeful breathing, mental focus, body awareness and meditation are integral components of the exercise. The beauty of Tai Chi is not only in the physical form, but also in its safety for all levels of fitness. It is helpful for individuals from high level athletes to those with physical disabilities. The movements are natural and gentle without forcing the muscles and joints to extreme or uncomfortable positions. It is often used as an adjunct therapy in the wellness as well as rehabilitation of a variety of athletic (ACL surgery, joint replacements) and neurological conditions (Parkinson’s, MS, head trauma), to name a few. Based on the aforementioned Chinese study, Tia Chi can be applied as a technique to control or lower blood pressure, especially for those who cannot utilize traditional aerobic exercise.
Tai Chi has been found to offer many physical and mental benefits. Some of these include:
Muscle Strength – upper and lower body, trunk and core strength
Flexibility – participants report improved range of motion and flexibility of the spine and extremities
Balance and Proprioception – some studies report a reduction of falls due to a variety of sustained positionsand improved awareness of one’s body in space
Aerobic Conditioning - recent studies have found that participants have lower heart rate and blood pressure
Mental Health – through improved balance, strength, and flexibility, studies show participants have gained confidence and control as well as lower blood pressure and stress reduction.
All Tai Chi classes begin with four basic principles: warm-up, instruction, practice and breathing.
Warm-up- gentle easy motions to warm-up and loosen the joints and muscles to prevent injury.
Tai Chi Forms – “Short Forms” are beginner movements which are gentle, slow, and short in duration while “Long Forms” are more advanced.
Breath Work – gentle breathing combined with movement to relax the mind and focus energy
Don’t be intimidated by the language or history – Yang, Wu, Cheng are only brands of movements with a history of martial arts but this in no way impacts participation.
Get medical clearance – check with your physician to see if Tai Chi is safe for you. Some orthopedic or vestibular problems might require special attention.
Observe or take a beginner class – often available at local fitness clubs or senior centers. Research options in your area and find a friend to join you. Consider an introductory instructional video to get a feel for Tai Chi. (See local Tia Chi classes below)
Meet with an instructor – if it makes you more comfortable, make time to talk to an instructor before enrolling in a class.
Dress for success – wear loose-fitting clothes that allow for range of motion and comfortable shoes for balance and support.
Track your progress – use an app or keep a journal of your progress. Heart rate, blood pressure and endurance (the time you can hold a pose or tolerate a class) are easy to monitor.
Model: Lily Smith, University of Scranton Physical Therapy Student and PT aide at Mackarey Physical Therapy.
Sources: HarvardHealthPublishing; New Atlas; China Academy of Chinese Medical Sciences (CACMS); National Institutes of Health
Local Tai Chi Classes: Steamtown Yoga, Scranton, PA; Mission Yoga, Scranton, PA;Dragon’s Heart Tai Chi & Kung Fu, Clarks Summit, PA; Rothrocks Kung Fu & Tai Chi, Duryea, PA
For more information: HarvardHealth; www.taichihealth.com; www.treeoflifetaichi.com

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
As most sports enthusiasts know, Aaron Rodgers, former Green Bay Packer quarterback and recent New York Jets QB (for just over a minute and half) suffered a season ending injury when he tore his Achilles tendon in the first game of the 2023/24 NFL season. Since then, I have been answering many questions from patients and sports fans about the nature of the Achilles Tendon rupture injury, recovery, and how to prevent it.
As the days continue to get shorter and temperatures begin a slow steady decline, athletes and exercise enthusiasts will work harder to warm-up and exercise during the winter months. A little caution and preparation are in order to avoid muscle/tendon strain, or worse yet, muscle/tendon tears, especially Achilles Tendon rupture. The Achilles tendon is one of the more common tendons torn.
This is the second of two columns on Achilles tendon rupture. Last week, I discussed the definition, sign and symptoms of the problem. This week will present examination, treatment and outcomes.
A thorough history and physical exam is the first and best method to assess the extent of the injury and determine accurate diagnosis. While a complete tear is relatively easy to determine, a partial or incomplete tear is less clear. Ultrasound and MRI are valuable tests in these cases. X-rays are not usually used and will not show tendon damage.
Consultation with an orthopedic or podiatric surgeon will determine the best treatment option for you. When conservative measures fail and for tendons completely torn, surgical intervention is usually considered to be the best option with a lower incidence of re-rupture. Surgery involves reattaching the two torn ends. In some instances, a graft using another tendon is required. A cast or walking boot is used post-operatively for 6-8 weeks followed by physical therapy.
Most people return to close to normal activity with proper management. In the competitive athlete or very active individual, surgery offers the best outcome for those with significant or complete tears, to withstand the rigors of sports. Also, an aggressive rehabilitation program will expedite the process and improve the outcome. Walking with full weight on the leg after surgery usually begins at 6 -8 weeks and often requires a heel lift to protect the tendon. Advanced exercises often begin at 12 weeks and running and jumping 5-6 months. While a small bump remains on the tendon at the site of surgery, the tendon is well healed at 6 months and re-injury does not usually occur.
Prevention of muscle and tendon tears is critical for healthy longevity in sports and activities. In addition to the Achilles tendon, the tendons of the quadriceps (knee) and rotator cuff (shoulder) are also vulnerable. A comprehensive prevention program includes: gradual introduction to new activities, good overall conditioning, sport specific training, pre-stretch warm-up, stretch, strengthening, proper shoes, clothing, and equipment for the sport and conditions. Also, utilizing interval training, eccentric exercise (lowering body weight slowly against gravity – Photo 1) and proprioceptive and agility drills are essential (Photos 2 & 3).
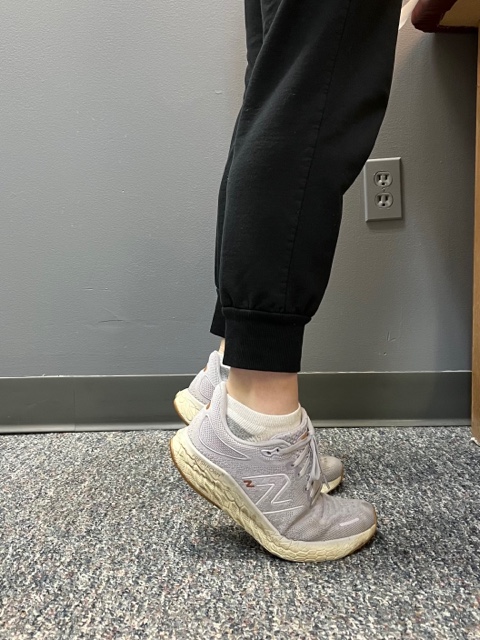

In PHOTO 1a & 1b: Eccentric Lowering and Lengthening: for the Achillies tendon during exercise. Beginning on the ball of both feet (1a), bend the strong knee to shift the weight onto the weak leg (1b). Slowly lowering the ankle/heel to the ground over 5-6 seconds. Repeat.
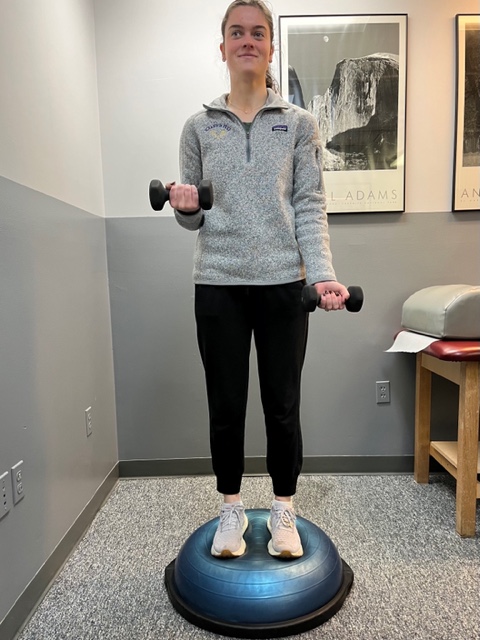
In PHOTO 2: Proprioceptive Training: for the Achillies tendon. Standing on a Bosu Ball while exercising the upper body (for example, biceps curls, shrugs, rows, lats) while maintaining balance on the ball.
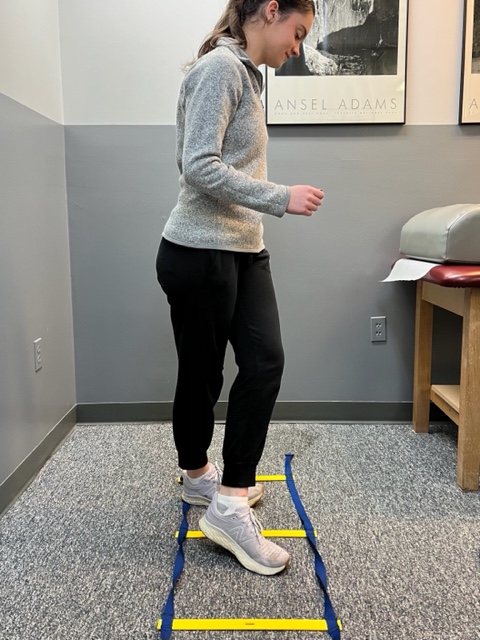
PHOTO 3: Agility Drills: for the Achilles tendon involves stepping through a “gait ladder” in various patterns and at various speeds.
MODEL: Kerry McGrath, student physical therapy aide at Mackarey Physical Therapy
Sources: MayoClinic.com;Christopher C Nannini, MD, Northwest Medical Center;Scott H Plantz, MD, Mount Sinai School of Medicine

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at GCSOM. For all of Dr. Mackarey's articles, visit our exercise forum!
As most sports enthusiasts know, Aaron Rodgers, former Green Bay Packer quarterback and recent New York Jets QB (for just over a minute and half) suffered a season ending injury when he tore his Achilles tendon in the first game of the 2023/24 NFL season. Since then, I have been answering many questions from many about the nature of the injury and how to prevent it.
As the days continue to get shorter and temperatures begin a slow steady decline, athletes and exercise enthusiasts will work harder to “fit in” a warm-up before running or other activities during the winter months. But, no matter how limited time is, skipping the warm-up is risky. This time of year, one can expect to feel a little cold and stiff, especially if you are over 40, and therefore a little caution and preparation are in order to avoid muscle/tendon strain, or worse yet, muscle/tendon tears. The more commonly torn tendon is the Achilles tendon . Prevention of muscle tears, including the Achilles tendon includes; gradual introduction to new activities, good overall conditioning, sport specific training, pre-stretch warm-up, stretch, strengthening, proper shoes, clothing, and equipment for the sport and conditions.
A muscle contracts to move bones and joints in the body. The tendon is the fibrous tissue that attaches muscle to bone. Great force is transmitted across a tendon which, in the lower body, can be more than 5 times your body weight. Often, a tendon can become inflamed, irritated, strained or partially torn from improper mechanics or overuse. Although infrequent, occasionally tendons can also snap or rupture. A tendon is more vulnerable to a rupture for several reasons such as a history of repeated injections of steroids into a tendon and use of medications such as corticosteroids and some antibiotics. Certain diseases such as gout, arthritis, diabetes or hyperparathyroidism can contribute to tendon tears. Also, age, obesity and gender are significant risk factors as middle-aged, overweight males are more susceptible to tendon tears. Poor conditioning, improper warm-up and cold temperatures may also contribute to the problem.
Tendon rupture is very painful and debilitating and must not be left untreated. While conservative management is preferred, surgical management is usually required for complete tears. The purpose of this column is to present the signs, symptoms and management of Achilles tendon ruptures.
The Achilles tendon (also called the calcaneal tendon), is a large, strong cordlike band of fibrous tissue in the back of the ankle. The tendon (also called the heel cord) connects the powerful calf muscle to the heel bone (also called the calcaneus). When the calf muscle contracts, (as when you walk on the ball of your foot), the Achilles tendon is tightened, tension is created at the heel and the foot points down like pushing a gas pedal or walking on tip of your toes. This motion is essential for activities such as walking, running, and jumping. A partial tear of the tendon would make these activities weak and painful, while a full tear through the tendon would render these activities impossible.
With age, the Achilles tendon (and other tendons) gets weak, thin, and dehydrated, thus making it prone to inflammation, degeneration, partial tear or rupture. The middle-aged weekend warrior is at greatest risk. A full or complete tear (Achilles tendon rupture) usually occurs about 2 inches above the heel bone and is associated with a sudden burst of activity followed by a quick stop or a quick start or change in direction, as in tennis, racquet ball, and basketball.
In some instances, the tendon can be injured by a violent contraction of calf when you push off forcefully at the same time the knee is locked straight as in a sudden sprint. Other times, the tendon is injured when a sudden and unexpected force occurs as in a trip off a curb or sudden step into a hole or a quick attempt to break a fall.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog Next Week: Achilles tendon Part II of II.
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at GCSOM. For all of Dr. Mackarey's articles, visit our exercise forum!