Spring sports and outdoor activities are here…tennis, pickleball, baseball, soccer, running, walking, hiking, golfing, etc. One of the most common injuries associated with physical activity, especially after a sedentary winter or change in temperature is a “pulled hamstring.” This painful injury is not only for the weekend warrior. Well-trained, healthy and fit professional athletes often have their season interrupted for weeks and months due to a hamstring injury. What is the hamstring? How is it injured? What is the best treatment?
A hamstring strain is a tear of the muscle fibers of the muscle group in the back of the thigh called the hamstring. The hamstring muscle is a group of three muscles that run from the back of the hip (lower pelvis), crossing the back of the knee and attaches to the knee bone (tibia). The hamstring muscles work to extend the hip and bend the knee during running and walking activities. They are very active when an athlete changes direction, especially forwards and backwards or decelerating. This injury, like others muscle strains, varies in intensity.
Severe hamstring strain occurs when many muscle fibers are torn. The athlete may experience a sudden onset of severe pain in the back of the thigh and occasionally report a popping sensation. Pain, swelling and black and blue skin from tissue damage and bleeding is often reported. Also, pain is reproduced when attempting to bend the knee. In very severe cases, the boney attachment can be pulled so strongly that a small fracture can occur. Healing time can be as short as a few days or as long as weeks or even months.
Your family physician will examine the back of your leg to determine if you have hamstring strain. Sometimes, pain in the buttocks and back of the leg can be referred from your lower back if the sciatic nerve is inflamed. In more advanced cases, you may be referred to an orthopedic surgeon for further examination and treatment. An X-ray, MRI or bone scan will show the extent of the tear and if the bone is involved. The diagnosis will determine if your problem is minor, moderate or severe.
There are many conservative options. Your family physician or orthopedic surgeon will help you decide which choices are best.
Recent studies have determined that a training program specifically designed to prevent hamstring injuries is effective, especially for the competitive athlete. This program includes:
SOURCES: Journal of Physical Medicine & Rehabilitation and American Academy of Orthopaedic Surgeons
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

A health column about sugar for Easter??? Well, maybe this information will be more appropriate next week! For those trying to lose weight or “get in shape” for the “bathing suit season,” a better understanding of the role sugar plays in your diet and overall health may be valuable. You have probably noticed a lot of attention being paid to sugar lately. Many television stars and other celebrities have shared their experiences using a “sugar cleanse” when they need to lose a few pounds and get healthier.
I have had several patients and friends tell me the same thing. For 4-6 weeks these people decide to avoid all refined sugars with the goal of losing weight and improving their health and wellness. Well, what is all the fuss about? Terms like simple sugars and simple carbs, which are purported to be bad, and complex carbs, suggested to be good, are being used ad nauseam. While medical research does not support the value of a short term “sugar cleanse,” it may have value for another reason. For example, it would be very beneficial if one engages in a “sugar cleanse” for the purpose of changing their palate with the hope of developing long term healthy eating habits, especially for those with diabetes…to be implemented AFTER the Easter candy has been consumed!
So, with this in mind, I decided to find the answers to some simple questions about the fuss over sugar. What is a simple sugar? What is a complex sugar? Which sugars are good for you?
Sugars, along with starches and fibers, are one of three types of carbohydrates (also referred to as a carb). A carb is “simple” or “complex,” based on its chemical composition and how it is processed in the body. It gets a little complicated because some foods have both simple and complex carbs. Typically, simple carbs are chemically more “simple” and basic, and therefore they are broken down more easily and serve as a quick source of energy. Some of these carbs are naturally simple (like fruit and milk) while others are processed or refined sugars such as those used in candy, soda and baked goods.
To determine if a food product has good or bad simple sugar, you must also know how much fiber, vitamins and minerals are in the food. A food with a higher sugar content combined with a low fiber, vitamin or mineral content will be worse than a food with the same sugar content but high fiber and vitamins or minerals. For example: a candy bar, which is high in sugar without fiber or vitamins or minerals, is not as healthy as a fresh orange, which contains fiber, vitamins and minerals along with its simple sugar (fructose).
Complex carbs have a more complicated chemical makeup and take more time for the body to break down for use as energy. Therefore, these are considered “good” carbs because they provide a more even distribution of energy for the body to use during activity. They cause a more consistent and gradual release of sugar into the blood stream (as opposed to peaks and valleys caused by simple carbs) and provide energy to function throughout the day. Additionally, “good” carbs have the added benefit of providing vitamins, fiber, and minerals that are missing from simple carbs.
Remember that carbohydrates fuel the body and are an important source of energy, especially for active and athletic people. However, carefully selecting the type of carb you eat is critical to peak function and performance.
Simple carbs taste great (according to our modern brain raised on simple sugars) and are easy to break down into a quick source of energy. However, the sensation of hunger is quick to return because the sugar is released and used up in the body quickly, giving the sensation of needing more.
Simple carbs are often “refined” and therefore stripped of their fiber, vitamins and minerals, which is why they are often referred to as “empty” calories.
Simple carbs lead to rapid spikes in blood sugar and insulin levels after meals. When these levels are not controlled over time, it can lead to obesity, which is ultimately related to adult-onset diabetes and high blood pressure.
Sources: www.everydayhealth.com; www.yourdictionary.com; Mayo Clinic
Visit your doctor regularly and listen to your body

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!


Guest Author: Gretchen Welby, PharmD, MHA
Gretchen graduated from Philadelphia College of Pharmacy and Science, The University of Scranton, and received a Doctor of Pharmacy degree from Temple University.
Gretchen has been teaching for over 25 years at Rutgers University, Keystone College, Lackawanna College, The University of Scranton, and Marywood University. She has earned certifications in Pilates, yoga, barre and teaches all three locally. She has a Wellness and Lifestyle coaching certification from Harvard University.
Gretchen resides in Scranton with her husband, Timothy Welby, MD, and has three daughters – Casey, Kate, and Caroline.
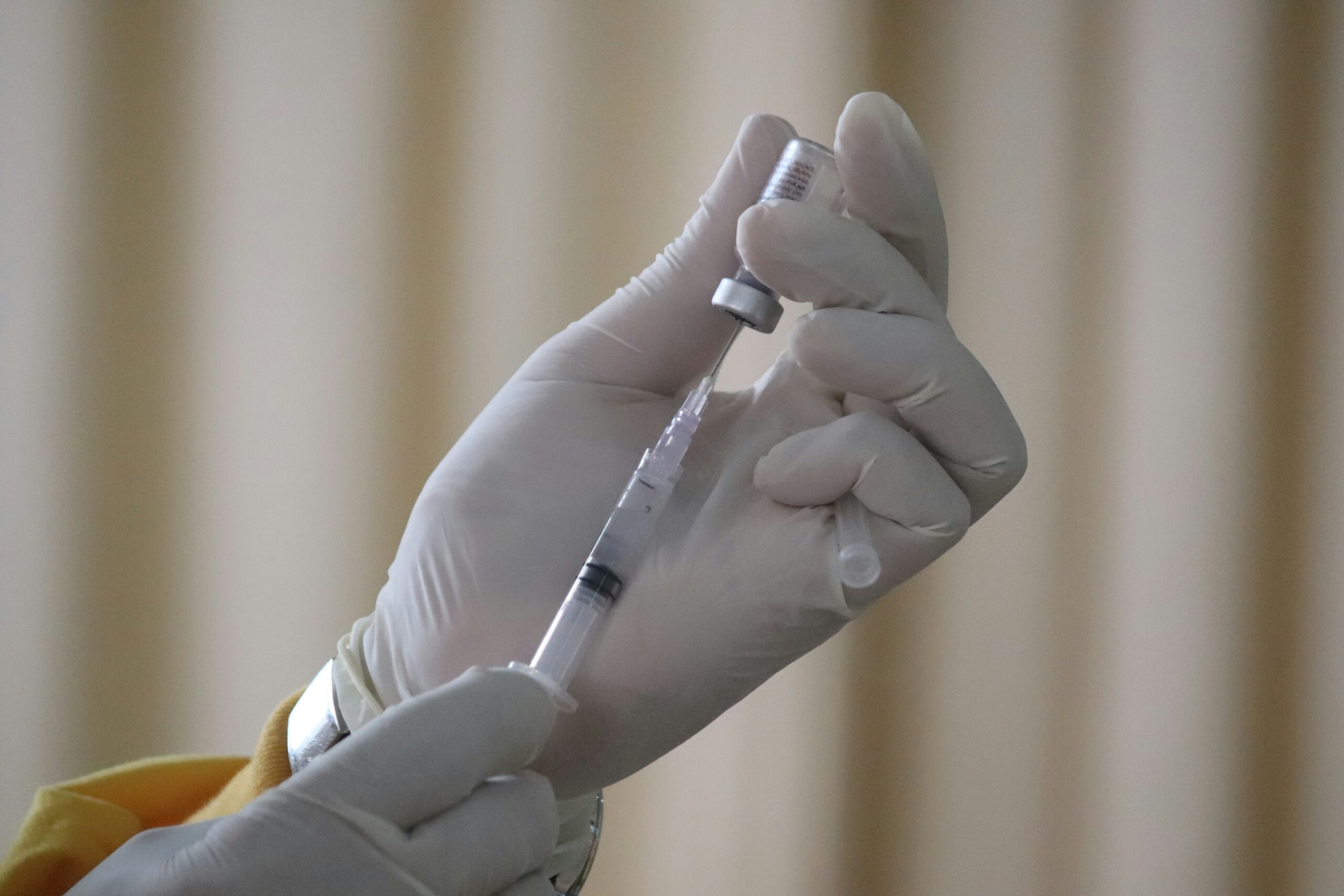
I have invited Gretchen Welby, PharmD, MHA to present the current wisdom on the very controversial topic of vaccination/immunization to raise awareness and dispel any myths and misunderstandings.
Scientific progress has rarely advanced by popular vote, and vaccination is no exception. While public sentiment deserves respect and thoughtful engagement, the evidence guiding immunization policy is built on decades of rigorous research, transparent testing and continuous review. These research processes are designed precisely to rise above fear, trend, politics or misinformation. Choosing to prioritize scientific findings over shifting opinion is not an act of dismissal, but of responsibility…it is a commitment to decisions that protect both individual lives and the collective good, even when those decisions challenge what feels comfortable or widely believed.
2024 marked the 50th anniversary of the World Health Organization’s Expanded Programme on Immunization (EPI). An initiative to make life-saving vaccines available to all worldwide. A modeling study done to mark the 50 years of EPI estimated that vaccination averted 154 million deaths, including 146 million deaths among children. Several additional studies on vaccine effectiveness show that vaccines improve infant safety, contribute to a healthy society, and even reduce cancer risk. Vaccines work for an individual and society. The data show that many vaccines can reduce mortality by 99% or more. Unfortunately, global immunization has been a victim of its own success because people have forgotten how deadly and dangerous the diseases vaccines protect against can be.
Vaccine effectiveness is overshadowed today by misinformation about vaccine safety, changing vaccine administration timelines, and mixed public health messaging. What are the outcomes of the recent relaxed vaccine message? The number of measles cases has jumped. Fifty-nine cases were reported in 2023. In 2025, 2242 cases were reported. For additional perspective, an article published in the 2007 edition of JAMA listed the number of deaths pre-vaccine release and the number of deaths post-vaccine release. The findings are remarkable.
The recent Centers for Disease Control and Prevention (CDC) change to the childhood vaccine schedule reduces routine protection against 13 childhood diseases to 7, with shared decision-making now required for the remaining 6. Diphtheria, tetanus, acellular pertussis (DTaP; Tdap), Haemophilus influenzae type b (Hib), Pneumococcal (PCV), Inactivated poliovirus (IPV), Measles, mumps, rubella (MMR), Varicella (VAR), and Human papillomavirus (HPV – changing from 2 doses to 1 dose) are now part of the routine vaccine schedule.
Rotavirus, COVID-19, Influenza, Hepatitis A, Hepatitis B, Meningococcal ACWY, and Meningococcal B are now grouped in a shared-decision-making model. Traditionally, when changes are made to the vaccine schedule, they are made with much deliberation, study, and expert input from multiple agencies and governing bodies. However, this recent change, however, did not follow the normal study path. This is concerning because changes are proposed without proper study of the immediate and long-term consequences.
Vaccines have been shown to be safe, with most patients experiencing very minor side effects. Normal reactions from vaccinations include low-grade fever for 24-48 hours. A low-grade fever and minor muscle aches signal the body's immune response. Tenderness and redness at the injection site are other normal reactions from immunization and should last from 24-48 hours. There is no proof that thimerosal (a preservative historically used in vaccines) causes adverse reactions. Additionally, thimerosal has been removed from most vaccine preparations used today. Vaccines do not overwhelm a child’s immune system. Children are exposed to hundreds of antigens daily. A WHOLE pediatric vaccination schedule exposes them to around 50 antigens. There is NO evidence to support altering or delaying the American Academy of Pediatrics vaccination schedule. This does NOT increase safety; it DECREASES protection at a time when infants and children are most vulnerable.
How can consumers of healthcare information, in particular, vaccine information, find reliable, trustworthy, educated guidance? Since the June 2025 changes in CDC personnel have resulted in less qualified members of the Advisory Committee on Immunization Practices (ACIP), it is generally best to rely on non-governmental sources such as the American Academy of Pediatrics, American College of Gynecologists, the Infectious Disease Society of America, and the Vaccine Integrity Project for vaccine advice. Additionally, discuss vaccine efficacy and safety with your doctor.
For More Information:
Vaccination greatly reduces disease, disability, death and inequity worldwide - PMC
The New Federal Vaccine Schedule for Children: What Changed and What Are the Implications? | KFF
JAMA 2007; 298:2155-2162
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
It’s that time of year…after a long winter of nights that come early and last too long there is LIGHT at the end of the tunnel! In the fall and winter, especially this far north, many people start to feel the gloom of their surroundings creep into their psyche and spring cannot arrive too soon...Is this normal, or a sign of something more serious?
Seasonal affective disorder, or SAD, is at the far end of a spectrum of seasonal mood changes. The mildest of these, “seasonality”, is a normal response to cyclical changes in weather and light exposure. However, when symptoms like depressed mood, lack of motivation, or a shift to more vegetative daily habits become severe and debilitating, SAD may be the cause. In fact, one study found that SAD affects up to 10% of primary-care patients, and that those with a previous diagnosis of depression are even more at risk. Fortunately, though, there are well established therapies that can help those afflicted with SAD to get through the dark winter months.
The American Psychiatric Association defines SAD as a subtype of either Major Depressive Disorder or Bipolar Disorder, depending on the symptoms. It can consist of episodes that onset during either fall/winter or spring/summer, or have symptoms characteristic of either “major depressive” or “manic” episodes. The vast majority of those with SAD, however, experience a persistent overall depressed mood during the shorter days of fall and winter.
In more serious cases:
If enough of these symptoms are present for a long enough time and onset in a seasonal pattern, that can mean Seasonal Affective Disorder. Most people with the disorder find themselves sleeping more and eating more (especially carbs), and report that their symptoms can even resolve with relocation to a sunnier environment. Along the spectrum of disease is a less severe form called “subsyndromal” SAD, which can still be effectively treated. Periods of SAD tend to resolve with the coming of spring, but they can be immensely distressing and always deserve medical intervention.
No one knows exactly why Seasonal Affective Disorder happens, but it appears to be associated with decreased exposure to natural light during the fall and winter months. One possible explanation is the “phase-shift” hypothesis. It states that your body’s circadian rhythms, which are regulated by hormones and the brain, become out-of-step with environmental sleep/wake cues as the days shorten. In other words, the light levels around you and your body’s internal clock are telling you two different things about when to sleep. This disruption of circadian rhythms, or “phase-delay”, likely contributes to the symptoms of SAD, although precisely how it induces changes in mood remains unclear.
Another hypothesis for the mechanism underlying SAD involves abnormalities in the activity of serotonin, a neurotransmitter in the brain. Normally, serotonin regulates mood and attention. However, studies have found that people with SAD clear serotonin out of their brains faster, giving the hormone less of a chance to provide a boost in mood.
Current medical treatment of SAD targets the changes in both circadian rhythms and serotonin metabolism. This can be accomplished with light therapy, antidepressant medications or a combination of both.
Medical Contributor:
Brendan Bormes, MD, GCSM 2019: This column was previously featured in “Health & Exercise Forum” in association with the students and faculty of Geisinger Commonwealth School of Medicine.
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

According to the Centers for Disease Control and Prevention (CDC), the 2025/26 flu season has been exceptional. Normally, elderly adults have the largest number of flu related hospitalizations while young children are second. This year, however, baby boomers between 50 and 64 years of age are the second most vulnerable. And, as of January 2026, the US flu season has resulted in an estimated 19 million illnesses, 250,000 hospitalizations, and 10,000 deaths. At the risk of creating an overreaction and promoting “germaphobic” behavior, if there is one time of year that diligent hygiene has merit, it is now…during flu season.
Contracting the cold or flu can make you feel run-down and under the weather for weeks. Unfortunately, your daily activities and responsibilities cannot take a sick day. The common cold and flu is most prevalent during late fall, winter and early spring. According to flufacts.com, “The influenza virus, more commonly known as the flu, is defined as a contagious respiratory infection that infects the nose, throat, and lungs. Thankfully, there are several easy and effective preventive measures that can reduce the probability of contracting the cold and flu. These preventive measures are designed to help keep your immune system strong and healthy. A healthy immune system fights against pathogens, such as the cold and flu virus. This article will focus on the ten best ways to prevent the flu and cold this season.
Sources: www.flufacts.com; www.webmd.com; www.lifescript.com; www.cdc.gov
Guest Contributor: Paul Mackarey, Jr. DPT, is a Doctor of Physical Therapy and partner at Mackarey & Mackarey Physical Therapy Consultants, LLC in Scranton and Clarks Summit.


EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

NEPA has had its share or snow this winter…and the recent storm added plenty of the pretty white stuff for work and play. Much has been written about the dangers of snow shoveling for your heart. However, while not fatal, low back pain is the most common injury sustained while shoveling snow. Heart attacks are also more common following wet and heavy snow.
Snow shoveling can place excessive stress on the structures of the spine. When overloaded and overstressed, these structures fail to support the spine properly. The lower back is at great risk of injury when bending forward, twisting, lifting a load, and lifting a load with a long lever. When all these factors are combined simultaneously, as in snow shoveling, the lower back is destined to fail. Low back pain from muscle strain or a herniated disc is very common following excessive snow shoveling.
Sources: The Colorado Comprehensive Spine Institute; American Academy of Orthopaedic Surgeons
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Patients often tell me that they would like to exercise but hesitate due to their knee or hip pain. They want to know what they should avoid, how to prevent and what is recommended to prevent or limit the progression of arthritis. Osteoarthritis (OA) is also known as degenerative arthritis. It is the most common form of arthritis in the knee. OA is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the joint which eventually wears down to the bony joint surface.
It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. It causes gradual onset of pain, swelling and stiffness in the joint involved, especially after increased activity. While diet and exercise help, some people are more likely to develop OA based on previous trauma or injury, labor intensive occupations and genetics. Either way, we all get OA to some degree but there are a few things you can do to limit wear and tear to your joints.
However, OA is not an excuse to avoid exercise, but it is important to be smart about it. Regular exercise is essential to maintain a normal lifestyle for those with OA. However, if you make poor lifestyle choices, do the wrong exercise, use poor technique, or are too aggressive, you could flare-up your joints and do more harm than good.
SOURCES: WebMD, University of Pennsylvania
Visit your family doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
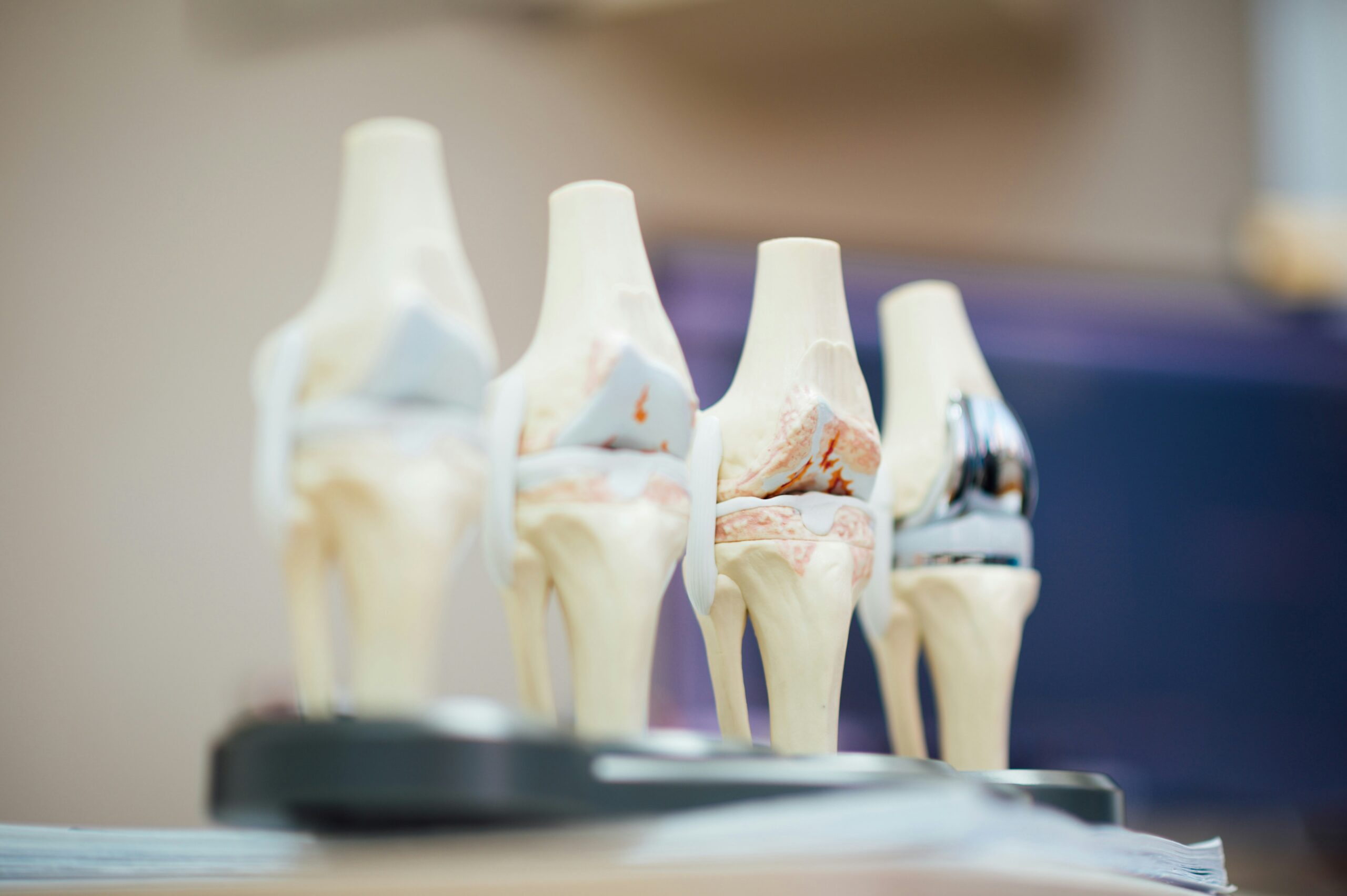
Patients often tell me that they would like to exercise but hesitate due to their knee or hip pain. They want to know what they should avoid, how to prevent and what is recommended to prevent or limit the progression of arthritis. Osteoarthritis (OA) is also known as degenerative arthritis. It is the most common form of arthritis in the knee. OA is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the joint which eventually wears down to the bony joint surface.
It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. It causes gradual onset of pain, swelling and stiffness in the involved joint, especially after increased activity. While diet and exercise help, some people are more likely to develop OA based on previous trauma or injury, labor intensive occupations and genetics. Either way, we all get OA to some degree but there are a few things you can do to limit wear and tear to your joints.
SOURCES: WebMD, University of Pennsylvania,
Visit your family doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
Next Week: Part II of II “Save Your Joints”
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

It is no surprise that the most common New Year Resolution is to be healthier…eat less, exercise more, etc. However, health is multidimensional! To be truly healthy, one must have a healthy mind, body and spirit! It is well documented and established that exercise and diet contribute to your physical health, and mentally, the brain is healthier by avoiding toxins such as tobacco, drugs and alcohol, while the spirit is healthier by being mindful, spiritual and meditative. Unfortunately, less attention is paid to other critically important aspects of health: the unhealthy impact of negative visceral emotions such as hate, jealousy, and anger.
Considering our present divisive social and political climate in the United States and globally, I find myself in constant search to understand the pervasive hate and division which seems to be, not only prevalent, but acceptable. I have attempted to read books such as “The Science of Hate,” by Matthew Williams, about the science of hate and survival, “Demon Copperhead,” by Barbara Kingsolver, about those marginalized and left behind, ”The Demon of Unrest,” by Erik Larson, about the history of our national political division preceding the Civil War and its relevance in the present, and watch TED Talks podcasts and television specials such as those presented by WVIA Public Media in a special series “We Stand Against Hate.”
All of this, to no avail! I failed in my effort to understand the unthinkable: We hate individuals whom we have NEVER even met. We hate groups of people through unfounded generalizations. We hate because of color, creed, stature, rank?!?! At the end of the day, I just don’t get it! Fortunately, I was not born with the “hate gene” and may never fully understand. But what I do understand is that HATE IS UNHEALTHY! So, if you want to be truly and completely healthy this new year, work on your hate!
The word “hate” is thrown around more often than the actual emotion is felt. The statement “I hate broccoli” is rarely accompanied by the strong negative emotion of true hatred. Even strong feelings of anger or disgust are not the same as hate. According to Laura Williams, clinical psychologist “Hate is a profoundly intense and enduring dislike for someone or something. Hate can be tenacious, and often has roots in mistrust, fear, or (lack of) individual power, and vulnerability.”
It can be hard to distinguish hate from other powerful negative emotions that you may be feeling at the same time. Some psychologists say what makes hate different is that it’s directed toward who or what someone or something is, rather than what they’ve done.
The negative physiological, physical health, mental and emotional effects of hate are well documented by many sources including the National Institutes of Health.
Ultimately, hate creates an internal state of emergency which demands significant physical and mental resources and leads to wear-and-tear on your entire system. Letting go of hate is a form of self-care that promotes relaxation and long-term well-being.
2026 is a great opportunity to be truly healthy…eat well, exercise more and rid yourself of hate!
Visit your family doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Happy Holidays Seniors! My gift to readers this holiday season is to offer some health tips for seniors. However, before I get accused of being a “Scrooge” about enjoying the food and drink associated with the season, please know that I was raised in an Italian kitchen. As such, it is fair to say that I have and will eat my fair share of the Italian Christmas Eve food celebration consisting of, but not limited to: Chianti wine, seafood antipasti, calamari, baccala, smelts, pasta with anchovies, seafood ravioli, cannoli, Italian cheesecake and Baci Perugina Dark Chocolate Hazelnut candy, cappuccino, espresso, sambuca and limoncello.
Overindulgence during the holidays causes many, including seniors, to make New Year's resolutions related to diet and exercise. But, this year, I propose that you incorporate healthy habits during the holiday season, and you may find that your resolutions are not as hard to keep. According to American Association of Retired Persons (AARP), seniors are considered those 50 years old and older. I will never forget how humbled I felt when I received my application to join AARP a few years ago. With this in mind, this year I offer healthy holiday tips for seniors, who are especially vulnerable to unhealthy holiday habits.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
