Patients often tell me that they would like to exercise but hesitate due to their knee or hip pain. They want to know what they should avoid, how to prevent and what is recommended to prevent or limit the progression of arthritis. Osteoarthritis (OA) is also known as degenerative arthritis. It is the most common form of arthritis in the knee. OA is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the joint which eventually wears down to the bony joint surface.
It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. It causes gradual onset of pain, swelling and stiffness in the joint involved, especially after increased activity. While diet and exercise help, some people are more likely to develop OA based on previous trauma or injury, labor intensive occupations and genetics. Either way, we all get OA to some degree but there are a few things you can do to limit wear and tear to your joints.
However, OA is not an excuse to avoid exercise, but it is important to be smart about it. Regular exercise is essential to maintain a normal lifestyle for those with OA. However, if you make poor lifestyle choices, do the wrong exercise, use poor technique, or are too aggressive, you could flare-up your joints and do more harm than good.
SOURCES: WebMD, University of Pennsylvania
Visit your family doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
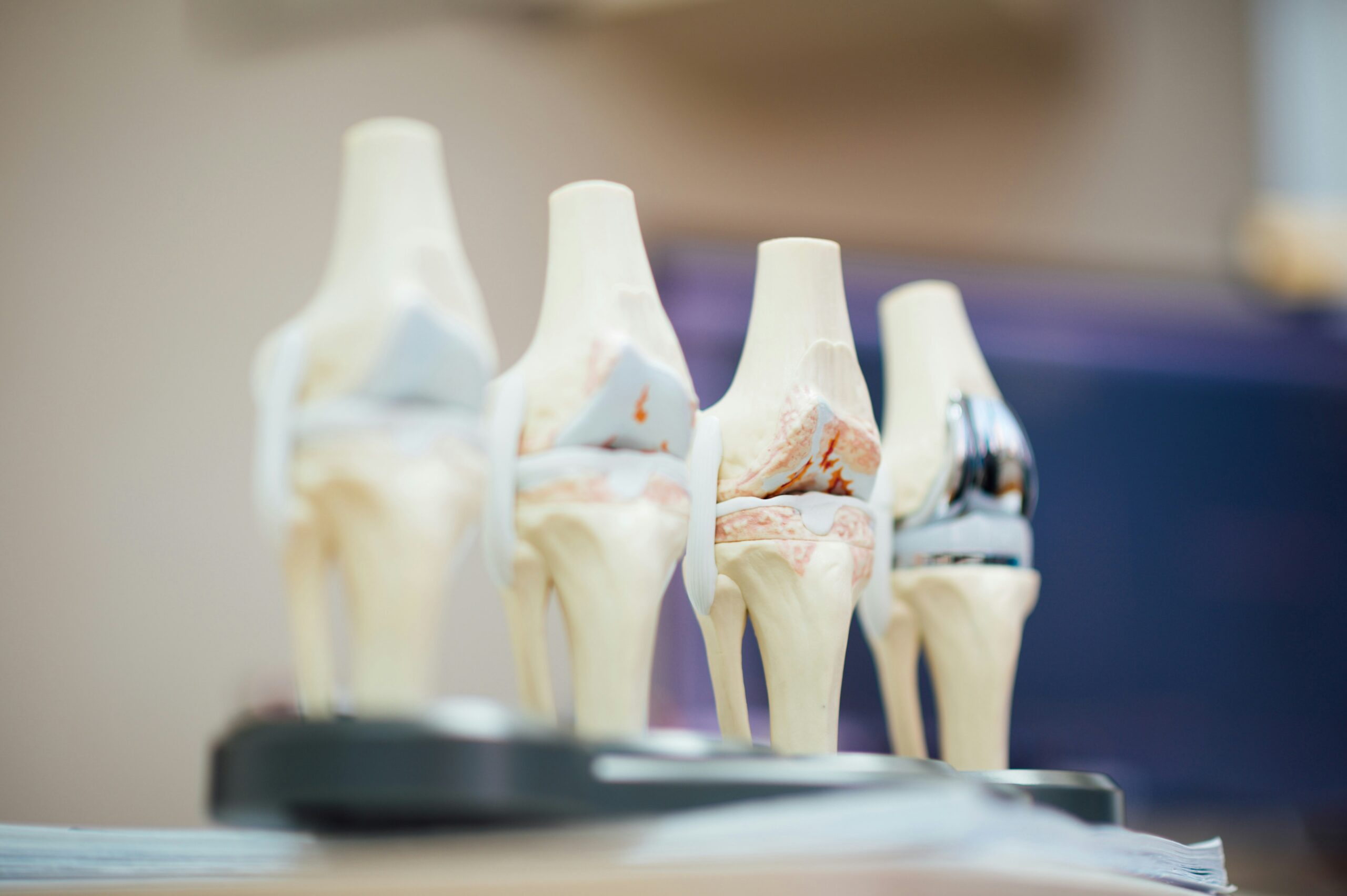
Patients often tell me that they would like to exercise but hesitate due to their knee or hip pain. They want to know what they should avoid, how to prevent and what is recommended to prevent or limit the progression of arthritis. Osteoarthritis (OA) is also known as degenerative arthritis. It is the most common form of arthritis in the knee. OA is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the joint which eventually wears down to the bony joint surface.
It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. It causes gradual onset of pain, swelling and stiffness in the involved joint, especially after increased activity. While diet and exercise help, some people are more likely to develop OA based on previous trauma or injury, labor intensive occupations and genetics. Either way, we all get OA to some degree but there are a few things you can do to limit wear and tear to your joints.
SOURCES: WebMD, University of Pennsylvania,
Visit your family doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
Next Week: Part II of II “Save Your Joints”
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

I wish I could tell you that after turning 50, there are health issues associated with age I plan to be mindful of and address proactively. Unfortunately, that ship has sailed for me well more than a decade ago. So, I share this medical information, not only as a health professional but also as an experienced senior.
Entering the fifth decade is not all dome and gloom. Often, this decade is associated with an established family, gratifying career, good health and acquired self-confidence…realizing that life does not have to be perfect to be wonderful!
However, research tells us that as the body ages, even small changes at the cellular level can be manifested into big changes and problems over time. Nine of ten older adults have some type of chronic disease and eight of ten have more than one. But the good news is that, with a modicum of effort, most of these illnesses can be controlled or prevented, including regular doctor visits, health screening and testing, and lifestyle changes.
While it is normal to experience some weight gain is expected with age. However, uncontrolled, the average person will gain 1-2 pounds per year, leading to 11 pounds per decade, according to the National Institutes of Health. Consequently, almost 45% of Americans between 40 to 60 are obese. Obesity is associated with at least 20 chronic illnesses such as high blood pressure, heart disease, diabetes, cancer, and arthritis.
SCREEN: Body Mass Index (BMI)
TREATMENT: Diet, Exercise, Lifestyle, Medications, Surgery
With age, the flexibility of blood vessels loses elasticity and, unchecked, two out of three adults over 60 have high blood pressure. While genetics is a factor, there are a few things that you can control such as diet (salt, calories), exercise, weight, stress, and smoking.
SCREEN: Blood Pressure Test, Lab Tests, Electrocardiogram (ECG/EKG)
TREATMENT: Diet, Exercise, Lifestyle, Medications
Plaque buildup in the arteries of the heart begins in childhood and advances rapidly with age. 6-7 percent of US adults between the ages of 40 and 60. 20% of men and almost 10% of women between the ages of 60 and 80 have heart disease.
SCREEN: Blood Pressure, Cholesterol testing, Blood Sugar Testing, Imaging (ECG/MRI)
TREATMENT: Diet, Exercise, Lifestyle, Medications, Surgery
10 % of Americans have diabetes and the percent only increases with age. Diabetes is associated with many serious chronic illnesses such as heart disease, blindness, kidney disease and others.
SCREEN: Blood Test for blood sugar levels such as A1C, fasting plasma glucose test and random plasma glucose test
TREATMENT: Diet, Exercise, Lifestyle, Medications
In many cases osteoarthritis (wear and tear of joints) is often associated with age. However, lifestyle, joint injuries, inactivity, obesity and diabetes play a significant role.
SCREEN: Physical Exam, Functional Scores, Xrays, MRI, CT, US
TREATMENT: Diet, Exercise, Physical Therapy, Lifestyle, Medications (NSAID’s, Steroids, Viscosupplementation), Bracing, Surgery
Loss of bone density and strength is associated with age and certain metabolic conditions such as early menopause, thyroid disease, prolonged use of blood thinners and steroids. However, a diet rich in vitamin D, regular weight bearing exercises such as walking, jogging, dancing etc can go a long way.
SCREEN: Fracture Risk Assessment Tool (FRAX), Dual-Energy X-Ray Absorptiometry (DEXA) TREATMENT: Diet, Exercise, Physical Therapy, Lifestyle, Medications (Oral and Injection)
Losing balance with age is a common problem due to changes in the vestibular system (balance system in the brain), loss of muscle strength and joint flexibility, and compromised vision and hearing. This can often lead to falls, head injuries and fractures.
SCREEN: Timed Up and Go (TUG) Test, Morse Fall Scale
TREATMENT: Physical Therapy – Falls Prevention Program/Balance Training , Diet, Exercise, Lifestyle, Environmental Modification, Vision/Hearing Testing
Almost 10% of adults between the ages of 55 and 65 have some form of vision and/or hearing loss. This can lead to many problems such as balance and falls as well as isolation and depression.
SCREEN: Regular Hearing Tests/Vision Testing
TREATMENT: Corrective Devices
Both men and women suffer from bladder problems with age... especially frequency and control. It can impact lifestyles in many ways. Often adults fail to hydrate properly, especially when traveling, to control urgency. This can lead to other health problems.
SCREEN: Urine Analysis, PSA, Imaging, CT Urogram, Urine Cystoscopy, Ultrasound,
TREATMENT: Diet, Exercise, Lifestyle, Avoid Caffeine and heavy lifting, Medications, Surgery
As the body ages, so too do the cells that make it up. Often these cells change into cancer different parts of the body. Skin, colon, breast, prostate, lung, throat, etc. Today, however, much progress has been made for early detection and treatment.
SCREEN: Physical Exam (Skin Exams), Lab Tests (blood work, PSA), Imaging (CT, Mammography, MRI), Genetic Testing, Pap Smears, HPV Tests, Colonoscopies/Stool Tests, Multi-Cancer Early Detection (MCED)
TREATMENT: Diet, Exercise, Physical Therapy, Lifestyle, Medications, Chemotherapy, Radiation, Immunotherapy and Targeted Therapy Surgery specific to the cancer type.
Age related mental health issues are vastly unreported and diagnosed. Medical problems can contribute to mental health such as high blood sugar levels and some infections. Overall, lifestyle, environmental factors and family structure and support are particularly important.
SCREEN: No Single Test – Combination of Tools including - Neurological and Cognitive Tests, Brain Scans (CT/MRI), Blood tests, Genetic Testing
TREATMENT: Diet, Exercise, Physical Therapy, Lifestyle, (avoid excessive toxins like alcohol and nicotine), Medications, Environmental Modifications.
SOURCES: WebMD, NIH, Mayo Clinic, Alzheimer’s Association, American Cancer Society, American Heart Association, American Diabetes Association

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Farmers and gardeners in NEPA always say that Memorial Day, the “kick off” day for planting without the fear of frost, however, this year we have had an unusually cold and wet spring… but it is not too late to start…not only for the beds but your body! While gardeners are anxious to work in their gardens and enjoy the fruits of their labor, a relaxing and enjoyable activity can turn dangerous quickly. Precautions are necessary as repetitive stress injuries such as shoulder and elbow tendonitis and carpal tunnel syndrome can stem from raking, weeding, digging and pruning. Additionally, simple scrapes, blisters, and bites can turn into serious problems if not treated appropriately. Since prevention is the best approach, the American Society of Hand Therapists (ASHT) promotes warm-up exercises and injury prevention tips to help all levels of gardeners avoid serious and long-term injuries while enjoying this popular outdoor activity.
ASHT recommends following these upper extremity warm-up exercises prior to gardening:
Note: These exercises should never be painful when completing them. You should only feel a gentle stretch. Hold 10 seconds and repeat 5 times. Should you experience pain, please consult a physician or hand therapist.
ASHT recommends the following guidelines to prevent injury and foster healthy gardening practices:
Professional Contributor: Nancy Naughton, OTD, CHT, is an occupational therapist and certified hand therapist practicing in NEPA.

Next Week: “Prevention of Gardening Injuries” Part II of II.
EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

At least once a week, a patient jokingly asks if they can get a “lube job” to loosen up their stiff knee joint. I respond by providing them with information about osteoarthritis and viscosupplementation, a conservative treatment administered by injection and approved by the FDA for the treatment of osteoarthritis of the knee.
Osteoarthritis (OA) is also known as degenerative arthritis. It is the most common form of arthritis in the knee. OA is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the knee joint which eventually wears down to the bony joint surface. It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. Symptoms include: pain, swelling, stiffness, weakness and loss of function.
Your family physician will examine your knee to determine if you have arthritis. In more advanced cases you may be referred to an orthopedic surgeon or rheumatologist for further examination and treatment. It will then be determined if you are a candidate for viscosupplementation. While this procedure is the most commonly used in the knee, it has also been used for osteoarthritis in the hip, shoulder and ankle.
Viscosupplementation is a procedure, usually performed by an orthopedic surgeon or rheumatologist, in which medication injected into the knee joint acts like a lubricant.
The medication is hyaluronic acid is a natural substance that normally lubricates the knee. This natural lubricant allows the knee to move smoothly and absorbs shock. People with osteoarthritis have less hyaluronic acid in their knee joints. Injections of hyaluronic acid substances into the joint have been found to decrease pain, improve range of motion and function in people with osteoarthritis of the knee.
When conservative measures, such as anti-inflammatory drugs, physical therapy, steroid injections fail to provide long lasting relief, viscosupplementation may be a viable option. Often, physical therapy and exercise are more effective following this injection to provide additional long-term benefit. Unfortunately, if conservative measures, including viscosupplementation fails, surgery, including a joint replacement may be the next alternative.
In 1997 the FDA approved viscosupplementation for osteoarthritis of the knee. Presently, there are several products on the market. One type is a natural product made from the comb of a rooster. However, if you are allergic to eggs or poultry products or feathers, you should not use the natural product. The other medication is best used for patients with allergies because it is manufactured as a synthetic product.
The long-term effects of viscosupplementation is much greater when other conservative measures are employed:
SOURCES: Genzyme Co, Sanofi-Synthelabo Inc, Seikagaku Co. and American Academy of Orthopaedic Surgeons
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
NEPA has experienced more than its share of bitter cold temperatures this winter. And, as much as I enjoy skiing, ice skating and snowshoeing, I have noticed a few achy joints when the mercury plummets! Osteoarthritis, the most common type of arthritis, is often considered to be a normal part of aging. Usually by the age of forty our joints, especially those which are weight bearing (lower spine, hips, knees, ankles, feet) begin to show signs of wear and tear. The cartilage begins to thin, the joint surfaces are not as smooth, and fluid which lubricates the joint becomes diluted, dehydrated and less protective.
Consequently, these aging joints become stiff, sore, weak, and sometimes swollen. Most people with osteoarthritis report additional pain and stiffness in the winter and early spring due to cold, damp weather and NEPA has plenty of it! The cold, for example, restricts the flow of blood to the joints, leading to more pain and stiffness. While moving to a warmer and less humid climate is one solution, it is not practical for most. But all is not lost because there are other alternatives to protect and keep your joints healthier this winter and early spring.
SOURCES: www.apta.org; www.webmd.com

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Patients often tell me that they would like to exercise but hesitate due to their knee or hip pain. They want to know what type of exercise is best for those suffering from osteoarthritis (OA). Osteoarthritis is also known as degenerative arthritis. It is the most common form of arthritis in the knee. It is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the joint which eventually wears down to the bony joint surface. It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. It causes gradual onset of pain, swelling and stiffness in the involved joint, especially after increased activity and weakness with loss of function due to disuse.
However, OA is not an excuse to avoid exercise but it is important to be smart about it. Regular exercise is essential to maintain a normal lifestyle for those with OA. However, if you do the wrong exercise, use poor technique, or are too aggressive, you could flare-up your joints and do more harm than good.
When performed correctly, exercise for those with OA has many benefits:
Pain Control
Exercise controls OA pain by releasing natural pain control chemicals in the body called endorphins. It also controls pain by assisting in weight loss and improving range of motion.
Weight Control
We all know how well exercise burns calories and that increased body weight creates increase stress on the joints.
Prevention of Joint Stiffness
Exercise will help maintain joint range of motion. A stiff joint is a painful joint.
Prevention of Muscle Weakness
Exercise will help maintain muscle strength. Weak muscles will allow or increase in joint wear and tear.
Maintain Lifestyle
If a joint is stiff and weak, then they become painful which negatively impacts your lifestyle. Exercise can prevent this problem.
Start Slowly
Wean into exercise because if you advance too quickly, you will flare up the joint and have increased pain. For example, walk for 5-10 minutes the first session. If you do not have pain, add 1-2 minutes each session.
Lose Weight
Every pound lost equates to less stress on your joints. For example, a loss of 5 pounds of body weight translates to 20-30 pounds of stress through the knee, according to David Borenstein, MD, President of the American College of Rheumatology. Also, body weight has a direct impact on daily activities. For example, walking upstairs creates stress through the knee equal to 4 times body weight and seven times body weight going downstairs. Therefore, less body weight equals less stress.
Low Impact Workouts
Low impact exercise creates less stress on the joints while strengthening leg muscles and those who those who maintain leg muscle strength have less stress on their joints. It is even important not to load your arms with heavy objects when walking or using stairs to limit joint stress.
Some examples of low-impact exercises are: walking, swimming, elliptical trainer, and biking. Strength training is also low-impact and should be performed with low weight and high repetitions. Water therapy is great for those with OA, especially in a heated pool. It is a great low-impact exercise with less gravity and stress on the joints. Walk, swim and do mild resistance exercises in the water. Use a snorkel and mask for swimming to limit excessive neck turning and back extension.
Walking is a great form of exercise; however, walking softly is important for those with OA. Wear good running shoes and orthotics if necessary. Discuss this with your physical therapist or podiatrist. When possible, use soft surfaces like cinder, mulch or rubber. Avoid grass and soft stand due to instability and torsion that may irritate your joints.
Warm-Up
Warming up your body is critical to prevent injury to the muscles and tendons. This can be done by marching in place or using aerobic equipment such as a bike for 5 to 10 minutes before exercise. Always perform the warm-up activity at ½ your normal pace.
Balance & Relaxation Techniques
Tai Chi and ballroom dancing are two good examples of activities which promote balance and relaxation. Studies showed that those with OA who participated in Tia Chi two times a week for eight weeks reported less pain, increased range of motion and improved daily activities and function. They also noted less low back pain and better sleeping.
Proper Clothing
Stay warm in winter and consider wearing compression shorts. Be cool in the summer months with DrytechR type material.
Pre/Post Exercise First Aid
If you are sore for longer than 12 to 24 hours after exercise, then you overdid it and must make adjustments next time. Otherwise, use hot packs, bath or shower before you exercise to loosen up and apply ice to your joints after exercise, especially if they are sore.
Post Exercise Stretch
Gentle, active range of motion stretches after exercise is important to maintain mobility. Do not bounce or cause pain. For example: Low Back – knees to chest; Arms – row –the – boat, arms behind head, arms behind back; Legs – wall lean calf stretch, bend and extend knees, open and close hips.
SOURCES: Rothman Institute, Philadelphia, PA and American Academy of Orthopaedic Surgeons; www.lifescript.com
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
There is still plenty of summer remaining and its not too late to think of your pleasure puddle in different light…a health spa! It may very well be the exercise of choice for many people. Many have discovered the benefits of moving their limbs in the warm water of a home pool following knee or shoulder surgery. Also, long distance runners who often look for cross training methods without joint compression and arthritis sufferers who are often limited in exercise choices by joint pain from compressive forces when bearing weight, can enjoy the buoyancy effects of water. These are good examples of the benefits or water exercise…aerobic and resistive exercise without joint compression.
Most doctors recommend some form of exercise with arthritis. Pain and fatigue are the most limiting factors for the person with arthritis. Pool exercise may be the answer. With proper technique, adequate rest periods, appropriate resistance and repetitions, water exercise can be very effective.
The following are some of the benefits of water exercise:
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
I have been advising my patients to exercise, keep active, and walk as long as they can in order to stay mobile and healthy. However, seniors often tell me activities that require prolonged walking is limited by ankle pain from arthritis. They often ask, “What is arthritis of the ankle?” How does it happen? What can I do about it?
Your family physician will examine your ankle to determine if you have arthritis. In more advanced cases you may be referred to a specialist such as a podiatrist, orthopaedic surgeon or rheumatologist for further examination and treatment. X-rays will show if the joint space between the bones in the ankle is getting narrow from wear and tear arthritis. If rheumatoid arthritis is suspected, blood tests and an MRI may be ordered. The diagnosis will determine if you problem if minor, moderate or severe.
In the early stages your treatment will be a conservative, nonsurgical approach, which may include; anti-inflammatory medication, orthopedic physical therapy, exercise, activity modifications, supplements, bracing, etc. You and your family physician, podiatrist, orthopedic surgeon or rheumatologist will decide which choices are best.
When conservative measures no longer succeed in controlling pain and deformity, improving strength and function then more aggressive treatment may be necessary.
SOURCES: Rothman Institute, Philadelphia, PA and American Academy of Orthopaedic Surgeons
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
Several years ago, while hiking to the bottom of the Grand Canyon with my family, my wife Esther developed “canyon knee,” also known as “hiker’s knee” or in medical terms, “patellar tendonitis.” Regardless of the term, the end result was that she had severe pain in the tendon below her knee cap and was unable to walk up the trail to get out of the canyon. In addition to ice, rest, bracing, and non-steroidal anti inflammatory medications, the National Park Ranger insisted that she use two trekking poles on her ascent to the rim.
Prior to that experience, I always thought that “walking, hiking sticks or trekking poles” were for show or those in need of a walking aide. Well, I could not have been more incorrect. Needless to say, Esther made it out of the canyon safely and, with the use of our life saving trekking poles; we have lived “happily ever after!” Now, 15 years later, I rarely walk more than 5 miles without my poles.
As a result of this experience, I have been recommending walking or trekking poles to my patients. These poles are an essential part of hiking or distance walking gear, for the novice and expert alike. Specifically, for those over 50 who have degenerative arthritis and pain in their lower back, hips, knees, ankles or feet, these simple devices have been shown to improve the efficiency of the exercise and lessen the impact on the spine and lower extremities. Additionally, using poles reduces the likelihood of ankle sprains and falls during walking. Trekking poles are also a safe option for those with compromised balance. If you want to walk distances for exercise and need a little stability but don’t want the stigma of a cane, trekking poles are for you.
Early explorers, Europeans and Native Americans have been using walking sticks for centuries. More recently, in the 1968 classic hiker’s bible, “The Complete Walker,” Colin Fletcher praised his “walking staff” for its multipurpose use: for balance and assistance with walking and climbing, protection from rattlesnakes, and for use as a fishing rod. Today, these sticks are now versatile poles made from light-weight materials.
Trekking poles are made of light-weight aluminum and vary in cost and quality. But, like most things, “you get what you pay for!” These hollow tubes can telescope to fit any person and collapse to pack in luggage for travel. Better poles offer multiple removable tips for various uses, conditions and terrains. For example, abasket to prevent sinking too deeply in snow, mud or sand; a blunt rubber tip for hard surfaces like asphalt or concrete, or the pointed metal tip to grip ice or hard dirt/gravel. Better quality poles offer an ergonomic hand grip and strap and a spring system to absorb shock through your hands, wrists and arms upon impact.
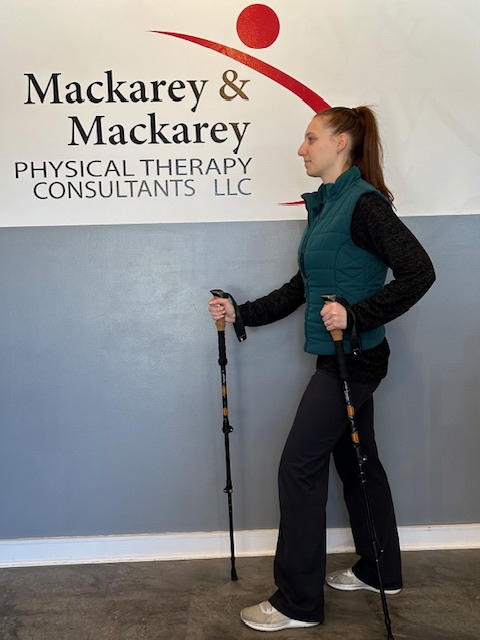
The poles should be properly adjusted to fit each individual. When your hand is griping the handle the elbow should be at a 90 degree angle. Proper use is simple; just walk with a normal gait pattern of opposite arm and leg swing. For example, left leg and right arm/pole swings forward to plant while the left arm/pole remain behind with the right leg .
This pattern is reciprocated with as normal gait advances (opposite arm and leg). I have been very pleased with my moderately priced poles (Cascade Mountain Tech from Dick’s Sporting Goods ($34.99 per pole). Prices range from $19.99 to 79.95 per pole. dickssportinggoods.com; montem.com; leki.com; rei.com. However, if you travel frequently to hike the State and National Parks, you may want to purchase more expensive poles that collapse and retighten more efficiently. (montem.com; leki.com;)
Montem Trekking Poles - with close-up of easy adjustable locking clasp.

There are numerous studies to support the use of trekking poles, especially research that supports their use for health and safety. One study compared hikers in 3 different conditions; no backpack, a pack with 15% body weight and a pack with 30% body weight. Biomechanical analysis was performed blindly on the three groups and a significant reduction in forces on lower extremity joints (hip, knee, and ankle) was noted for all three groups when using poles compared to those not using poles.
Another study confirmed that trekking poles reduced the incidence of ankle fractures through improved balance and stability. Additional studies support the theory that trekking poles reduce exercise induced muscle soreness from hiking or walking steep terrain and another study found that while less energy is expended in the lower body muscles using poles, increase energy is used in the upper body; therefore, the net caloric expenditure is equal as it is simply transferred from the legs to the arms.
In conclusion, it is important to remember that trekking poles for hiking or distance walking are much more than a style statement. They are proven to be an invaluable tool for health, safety and wellness by reducing lower extremity joint stress, improving stability and balance, and enhancing efficiency for muscle recovery.
Sources: Medicine and Science in Sports and Exercise. The Complete Walker, by Colin Fletcher
Model: Andrea Molitoris, PT, DPT at Mackarey Physical Therapy

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!