“Everybody talks about the weather, but nobody does anything about it,” said Mark Twain. Just ask 93% of the arthritis sufferers who believe that the weather affects their pain level. History tells us that Benjamin Franklin, Leonardo da Vinci, and Christopher Columbus also felt this way about the weather.
Patients at our clinic have been particularly sensitive to joint pain on cold, damp days, especially during the past few weeks. In my clinical practice of orthopedic and sports physical therapy, an informal survey found that 95 out of 100 patients (95%) with arthritis reported increased pain with weather changes. While most people report that the coldness and dampness seem to irritate their joints, they also report more pain with weather changes in the summer. There is a reasonable explanation…
Joints in the body have a lining called synovium that secretes a lubricating fluid called synovial fluid. In joints with arthritis, there is an overproduction of synovial fluid. In theory, when the barometric pressure changes, so to will the pressure inside your joints, especially if it is already overfull with extra fluid from arthritis. This added pressure stimulates the nerve endings in the joint to produce inflammation and pain.
Despite this overwhelming response from patients, scientific studies vary in their support of this claim. According to the Mayo Clinic, in 1961, a famous arthritis doctor (rheumatologist), built a climate chamber and discovered that when high humidity was combined with low barometric pressure, patients reported increased joint pain and stiffness. A recent study found that changes in barometric pressure and cooler temperatures are associated with joint pain. However, other studies have found increased joint pain with high barometric pressure in both warm and cold weather while another study found pain with low pressure.
What does this mean? It means that patients with arthritis consistently report pain with weather changes, but science has not found an accurate method to consistently support these claims. Some of these inconsistencies may be attributed to the fact that there are differences in sensitivity among individuals. For example, some patients have symptoms before the weather changes, while others notice symptoms during or after the weather changes. Still yet, some report more pain in colder conditions while others notice more pain in warmer weather. It appears that changes in the weather, such as a high to a low or warm dry to cold damp and vice versa is the culprit when it comes to irritating arthritis in a joint.
If I have arthritis, should you move to Arizona? Yes and no! Yes, the warm and dry climate of Arizona will probably make you feel better overall. However, it will not cure the degenerative changes in your joints, and you may still have pain when CHANGES in the weather occur. This is proven to be true by the fact that there are many very busy rheumatologists in Arizona!
In conclusion, it is safe to say that there is some evidence to support the claim that most patients with arthritis have increased symptoms of joint pain and stiffness with CHANGES in the weather:
Therefore, each patient must be individually evaluated by their physician to determine the extent of their arthritis and its relationship to the changes in the weather. While the cause of their increased symptoms with changes in the weather may not be completely understood, each patient must determine the adjustments in their lifestyle and/or medications according to the particular weather patterns that affect their problem most.
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Patients often tell me that they would like to exercise but hesitate due to their knee or hip pain. They want to know what they should avoid, how to prevent and what is recommended to prevent or limit the progression of arthritis. Osteoarthritis (OA) is also known as degenerative arthritis. It is the most common form of arthritis in the knee. OA is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the joint which eventually wears down to the bony joint surface.
It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. It causes gradual onset of pain, swelling and stiffness in the joint involved, especially after increased activity. While diet and exercise help, some people are more likely to develop OA based on previous trauma or injury, labor intensive occupations and genetics. Either way, we all get OA to some degree but there are a few things you can do to limit wear and tear to your joints.
However, OA is not an excuse to avoid exercise, but it is important to be smart about it. Regular exercise is essential to maintain a normal lifestyle for those with OA. However, if you make poor lifestyle choices, do the wrong exercise, use poor technique, or are too aggressive, you could flare-up your joints and do more harm than good.
SOURCES: WebMD, University of Pennsylvania
Visit your family doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
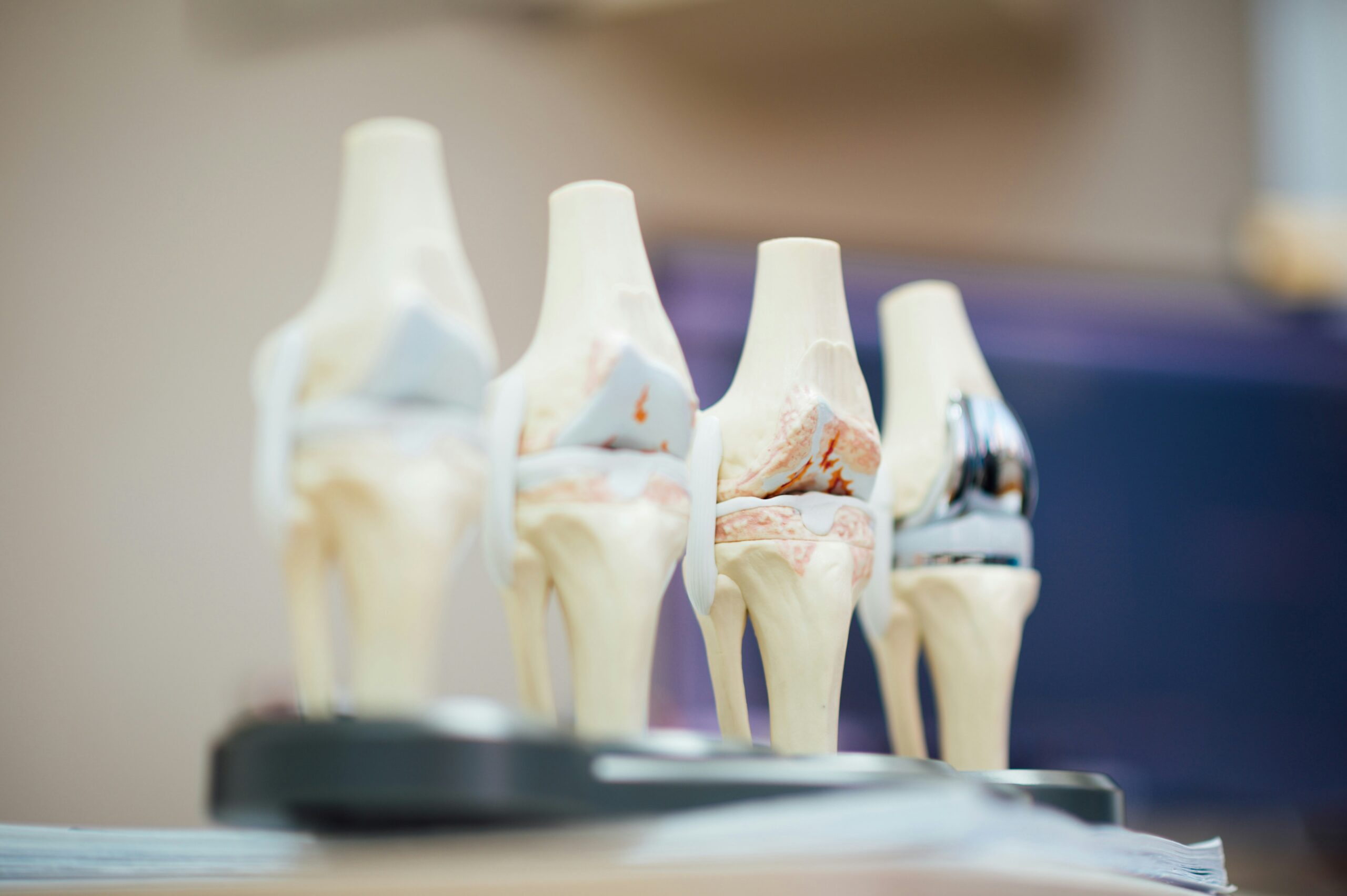
Patients often tell me that they would like to exercise but hesitate due to their knee or hip pain. They want to know what they should avoid, how to prevent and what is recommended to prevent or limit the progression of arthritis. Osteoarthritis (OA) is also known as degenerative arthritis. It is the most common form of arthritis in the knee. OA is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the joint which eventually wears down to the bony joint surface.
It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. It causes gradual onset of pain, swelling and stiffness in the involved joint, especially after increased activity. While diet and exercise help, some people are more likely to develop OA based on previous trauma or injury, labor intensive occupations and genetics. Either way, we all get OA to some degree but there are a few things you can do to limit wear and tear to your joints.
SOURCES: WebMD, University of Pennsylvania,
Visit your family doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
Next Week: Part II of II “Save Your Joints”
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Happy Holidays Seniors! My gift to readers this holiday season is to offer some health tips for seniors. However, before I get accused of being a “Scrooge” about enjoying the food and drink associated with the season, please know that I was raised in an Italian kitchen. As such, it is fair to say that I have and will eat my fair share of the Italian Christmas Eve food celebration consisting of, but not limited to: Chianti wine, seafood antipasti, calamari, baccala, smelts, pasta with anchovies, seafood ravioli, cannoli, Italian cheesecake and Baci Perugina Dark Chocolate Hazelnut candy, cappuccino, espresso, sambuca and limoncello.
Overindulgence during the holidays causes many, including seniors, to make New Year's resolutions related to diet and exercise. But, this year, I propose that you incorporate healthy habits during the holiday season, and you may find that your resolutions are not as hard to keep. According to American Association of Retired Persons (AARP), seniors are considered those 50 years old and older. I will never forget how humbled I felt when I received my application to join AARP a few years ago. With this in mind, this year I offer healthy holiday tips for seniors, who are especially vulnerable to unhealthy holiday habits.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Happy Holidays! Despite political divisions and war in the Middle East and Ukraine, it is at this time of year that we celebrate life with great hope and faith. People of many faiths take time to reflect, respect, and resolve. Christians celebrate Christmas, the miraculous birth of Christ, the Son of God, and the Messiah. Jews celebrate Chanukah, the miraculous festival of lights, when one night’s oil provided enough light and safety for 8 nights. Both major faiths promote healthy lifestyles for the mind, body and spirit. These faiths are grounded in hope, faith, love and peace. It is no surprise that studies repeatedly demonstrate that faithful and spiritual people live longer and healthier lives! At this turbulent time in the world, it is important to note that people of all faiths benefited equally!
I purport that to be truly healthy; one must have faith because complete health is multidimensional. Socrates preached this message to his students thousands of years before Christ. One must have a healthy mind, which requires intellectual stimulation with attainable goals related to education and intellect. One must have a healthy body by eating well, engaging in physical activity and having attainable goals related to his/her body. Likewise, one must have a healthy spirit with faith, hope, prayer and meditation, comrades and counsel, and set attainable spiritual goals.
Being religious or spiritual has been shown to benefit your mind, body and spirit…

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

November is National Alzheimer’s Disease Awareness Month. It is appropriate that it is also National Family Caregivers Month, since many people afflicted with Alzheimer’s are physically well and often rely on caregivers. It would be very unusual to find a person whose life has not been affected by someone with Alzheimer’s disease (AD). AD is a form of dementia. It is sometimes referred to as Senile dementia/Alzheimer’s type (SDAT). Currently, more than 4 million people in the USA have AD. Approximately 10% of all people over 70 have significant memory deficits. The number doubles each decade after 70. The risk increases with age and family history for the disease.
AD is a progressive degenerative disease of the brain that affects memory and thought process. Memory impairment is the hallmark of this disease. Also, those suffering from AD present changes with the following: language, decision-making, judgment, attention, and other personality or aspects of mental function. AD progresses differently in each case.
Two types of AD have been identified, early onset and late onset. In early onset, symptoms appear before the age of 60 and progress very rapidly. It accounts for 5-10% of all cases. Autosomal dominant inherited mutations have been found in early onset AD.
The cause of AD is not completely understood; however, most experts agree that both genetic and environmental factors are involved. It is important to rule out other medical causes before a final diagnosis of AD can be made. Only a post-mortem microscopic examination of brain tissue can confirm the diagnosis. Structural and chemical parts of the brain disconnect as the brain tissue shows twisted fragments of protein that clogs up the nerve. Clusters of dead and dying nerve cells block the transmission of information and communication from one nerve cell to the next. AD causes a disconnection of areas of the brain that normally work together.
The Greater Boston Physicians for Social Responsibility and the Science and Environmental Health Network offer the following guidelines to reduce the Risk of Developing AD:
Source: The HealthCentralNetwork, Inc

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

While I fully expect to be at the “butt end” of many comments for this column, I feel compelled to address this topic at the request of several patients. It seems that many geriatric physical therapists commonly encounter patients that suffer from constipation which limits their participation in rehabilitation. Ironically, research demonstrates that exercise and activity actually help relieve constipation.
The National Digestive Diseases Information Clearinghouse (NDDIC) reports that 3.1 million people in the United States suffer from constipation. The NDDIC further reports that this problem leads to almost 400,000 hospitalizations, 1.4 million visits to emergency rooms, 1 million prescriptions and 121 deaths each year. Constipation is defined by the Ohio University College of Osteopathic Medicine as three or less bowel movements per week. It is also estimated that more than 27 percent of the elderly are affected.
Severe constipation can result in immediate medical attention in some cases due to intestinal obstruction. In addition to infrequent bowel movements, some symptoms include: feeling poorly, weight loss, loss of appetite, abdominal distention and/or pain, and vomiting.
Healthy people must continue to keep active. Get into good exercise habits at a young age and continue through life. Maintaining a consistent schedule of eating and exercise is also helpful. Some simple suggestions for beginning an exercise program for prevention of constipation in the healthy population are:
Depending on your general health and ambulatory status, these endurance exercises may be appropriate for you. Therefore, consider one or two of the following as a good starting point:
IN CONCLUSION: KEEP MOVING YOUR BODY AND YOU WILL KEEP MOVING YOUR BOWELS!
Visit your doctor regularly and listen to your body.
Keep moving, eat healthy foods, exercise regularly, and live long and well!

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

According to the United States Environmental Protection Agency, NEPA and all of Pennsylvania is experiencing a change in climate as indicated by a half a degree (F) in temperature, more frequent and heavy rainstorms and the tidal portion of the Delaware River is rising one inch every eight years. Last summer was one of our hottest on record and this summer has produced several heat waves with more expected. For those without air conditioning or access to a lake or pool, it will also be remembered as record setting warm temperatures. A local reader who cares for her elderly mother wrote to express her concern about dehydration in the elderly. Age, diet, illness and medications are some of the many reasons why elders suffer from dehydration not only in the summer heat, but year-round.
Next to oxygen, water is the nutrient most needed for life. A person can live without food for a month, but most can survive only three to four days without water. Even though proper hydration is essential for health, water gets overlooked as one of the six basic nutrients. Dehydration occurs when the amount of water taken into the body is less than the amount that is being lost. Dehydration can happen very rapidly (i.e. in less than eight hours); the consequences can be life threatening and the symptoms can be alarmingly swift.
In the body, water is needed to regulate body temperature, carry nutrients, remove toxins and waste materials, and provide the medium in which all cellular chemical reactions take place. Fluid balance is vital for body functions. A significant decrease in the total amount of body fluids leads to dehydration. Fluids can be lost through the urine, skin, or lungs. Along with fluids, essential electrolytes, such as sodium and potassium, are also perilously depleted in a dehydrated individual.
Dehydration is the most common fluid and electrolyte disorder of frail elders, both in long term care facilities and in the community! Elders aged 85 to 99 years are six times more likely to be hospitalized for dehydration than those aged 65 to 69 years. More than 18% of those hospitalized for dehydration will die within 30 days, and associated mortality increases with age. Men appear to dehydrate more often than women and dehydration is often masked by other conditions.
Elderly individuals are at heightened risk for dehydration for several reasons. Compared to younger individuals, their regulatory system (i.e. kidneys and hormones) does not work as well and their bodies have lower water contents. Older adults often have a depressed thirst drive due to a decrease in a particular hormone. They do not feel thirsty when they are dehydrated. This is especially true in hot, humid weather, when they have a fever, are taking medications, or have vomiting or diarrhea. They have decreased taste, smell, and appetite which contribute to the muted perception of thirst. Because of dementia, depression, visual deficits, or motor impairments, elderly people may have difficulty getting fluids for themselves. Many elderly individuals limit their fluid intake in the belief that they will prevent incontinence and decrease the number of trips to the bathroom. The medications that they are taking (e.g. diuretics, laxatives, hypnotics) contribute to dehydration.
Elders may suffer headaches, fainting, disorientation, nausea, seizure, a stroke, or a heart attack as a result of dehydration. The minimum daily requirement to avoid dehydration is between 1,500 (6.34 cups) and 2,000 ml of fluid intake per day. Six to eight good-sized glasses of water a day should provide this amount. Better hydration improves well-being and medications work more effectively when an individual is properly hydrated.
Those who care for the elderly whether at home or in a health care facility need to be alert to the following symptoms:
By the way, plain old tap water is a good way to replenish fluid loss. Keep in mind that some energy drinks not only have excess and unneeded calories but also contain sugar that slows down the rate at which water can be absorbed from the stomach. Consuming alcoholic and caffeinated beverages actually have an opposite, diuretic effect!

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Despite recent challenges for air travel due to increased volume, severe weather and a nationwide shortage of air traffic controllers, Americans report high levels of enthusiasm for air travel this summer, including travel abroad.
Confession; I recently was on a long trip that required sitting on an airplane for more than six hours…and I wore compression stockings … guess I’m getting older (and wiser)!
Have you noticed that being in a car or on an airplane for more than three hours leads to neck and back pain? Soreness, stiffness and swelling in your legs? With a little planning, preventing or limiting these problems on long trips is possible. Also, as people age and/or develop other health problems, they are more vulnerable to developing a more serious problem associated with long trips; deep vein thrombosis (DVT) or blood clots. But problems with long-distance travel can be avoided. The following tips, based on research and personal experience, can prevent neck, back and leg pain and stiffness and DVT.
A DVT is a blood clot that forms in a deep vein. The deep veins pass through the muscles and cannot be seen like the veins just under your skin. While it may occur in your arms, it is much more common in the legs, especially the calf muscle when traveling. When a blood clot forms in a leg vein it usually sticks to the vein wall. Often, pain and swelling lead you to the doctor and treatment is rendered before serious complications develop. However, there are two possible complications. One, a pulmonary embolus, occurs when a part of the clot logged in your deep vein of the calf breaks off and gets lodged in the lung. This is a very serious problem that can be fatal. Two, post-thrombotic syndrome, occurs when you have pain and swelling in your calf after a DVT.
The following risk factors for DVT significantly increase the potential for problems when traveling on long trips by air, more than 5 hours. Trains, cars and buses also create a risk, but air travel creates a greater risk for the following reasons: reduced cabin pressure, reduced cabin oxygen levels, dehydration and alcoholic drinks, which may increase dehydration and immobility.
Airplane seats are “C” shaped and force you to round your neck and back forwards. These exercises are designed to stretch and extend your back in the opposite direction. Please perform slowly, hold for 3-5 seconds and repeat 10 times each hour.
Sitting:
When sitting in an airplane seat, take the neck pillow in the overhead compartment and place it in the small of your lower back. While sitting or standing up, perform postural exercises every 30-45 minutes.
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

I wish I could tell you that after turning 50, there are health issues associated with age I plan to be mindful of and address proactively. Unfortunately, that ship has sailed for me well more than a decade ago. So, I share this medical information, not only as a health professional but also as an experienced senior.
Entering the fifth decade is not all dome and gloom. Often, this decade is associated with an established family, gratifying career, good health and acquired self-confidence…realizing that life does not have to be perfect to be wonderful!
However, research tells us that as the body ages, even small changes at the cellular level can be manifested into big changes and problems over time. Nine of ten older adults have some type of chronic disease and eight of ten have more than one. But the good news is that, with a modicum of effort, most of these illnesses can be controlled or prevented, including regular doctor visits, health screening and testing, and lifestyle changes.
While it is normal to experience some weight gain is expected with age. However, uncontrolled, the average person will gain 1-2 pounds per year, leading to 11 pounds per decade, according to the National Institutes of Health. Consequently, almost 45% of Americans between 40 to 60 are obese. Obesity is associated with at least 20 chronic illnesses such as high blood pressure, heart disease, diabetes, cancer, and arthritis.
SCREEN: Body Mass Index (BMI)
TREATMENT: Diet, Exercise, Lifestyle, Medications, Surgery
With age, the flexibility of blood vessels loses elasticity and, unchecked, two out of three adults over 60 have high blood pressure. While genetics is a factor, there are a few things that you can control such as diet (salt, calories), exercise, weight, stress, and smoking.
SCREEN: Blood Pressure Test, Lab Tests, Electrocardiogram (ECG/EKG)
TREATMENT: Diet, Exercise, Lifestyle, Medications
Plaque buildup in the arteries of the heart begins in childhood and advances rapidly with age. 6-7 percent of US adults between the ages of 40 and 60. 20% of men and almost 10% of women between the ages of 60 and 80 have heart disease.
SCREEN: Blood Pressure, Cholesterol testing, Blood Sugar Testing, Imaging (ECG/MRI)
TREATMENT: Diet, Exercise, Lifestyle, Medications, Surgery
10 % of Americans have diabetes and the percent only increases with age. Diabetes is associated with many serious chronic illnesses such as heart disease, blindness, kidney disease and others.
SCREEN: Blood Test for blood sugar levels such as A1C, fasting plasma glucose test and random plasma glucose test
TREATMENT: Diet, Exercise, Lifestyle, Medications
In many cases osteoarthritis (wear and tear of joints) is often associated with age. However, lifestyle, joint injuries, inactivity, obesity and diabetes play a significant role.
SCREEN: Physical Exam, Functional Scores, Xrays, MRI, CT, US
TREATMENT: Diet, Exercise, Physical Therapy, Lifestyle, Medications (NSAID’s, Steroids, Viscosupplementation), Bracing, Surgery
Loss of bone density and strength is associated with age and certain metabolic conditions such as early menopause, thyroid disease, prolonged use of blood thinners and steroids. However, a diet rich in vitamin D, regular weight bearing exercises such as walking, jogging, dancing etc can go a long way.
SCREEN: Fracture Risk Assessment Tool (FRAX), Dual-Energy X-Ray Absorptiometry (DEXA) TREATMENT: Diet, Exercise, Physical Therapy, Lifestyle, Medications (Oral and Injection)
Losing balance with age is a common problem due to changes in the vestibular system (balance system in the brain), loss of muscle strength and joint flexibility, and compromised vision and hearing. This can often lead to falls, head injuries and fractures.
SCREEN: Timed Up and Go (TUG) Test, Morse Fall Scale
TREATMENT: Physical Therapy – Falls Prevention Program/Balance Training , Diet, Exercise, Lifestyle, Environmental Modification, Vision/Hearing Testing
Almost 10% of adults between the ages of 55 and 65 have some form of vision and/or hearing loss. This can lead to many problems such as balance and falls as well as isolation and depression.
SCREEN: Regular Hearing Tests/Vision Testing
TREATMENT: Corrective Devices
Both men and women suffer from bladder problems with age... especially frequency and control. It can impact lifestyles in many ways. Often adults fail to hydrate properly, especially when traveling, to control urgency. This can lead to other health problems.
SCREEN: Urine Analysis, PSA, Imaging, CT Urogram, Urine Cystoscopy, Ultrasound,
TREATMENT: Diet, Exercise, Lifestyle, Avoid Caffeine and heavy lifting, Medications, Surgery
As the body ages, so too do the cells that make it up. Often these cells change into cancer different parts of the body. Skin, colon, breast, prostate, lung, throat, etc. Today, however, much progress has been made for early detection and treatment.
SCREEN: Physical Exam (Skin Exams), Lab Tests (blood work, PSA), Imaging (CT, Mammography, MRI), Genetic Testing, Pap Smears, HPV Tests, Colonoscopies/Stool Tests, Multi-Cancer Early Detection (MCED)
TREATMENT: Diet, Exercise, Physical Therapy, Lifestyle, Medications, Chemotherapy, Radiation, Immunotherapy and Targeted Therapy Surgery specific to the cancer type.
Age related mental health issues are vastly unreported and diagnosed. Medical problems can contribute to mental health such as high blood sugar levels and some infections. Overall, lifestyle, environmental factors and family structure and support are particularly important.
SCREEN: No Single Test – Combination of Tools including - Neurological and Cognitive Tests, Brain Scans (CT/MRI), Blood tests, Genetic Testing
TREATMENT: Diet, Exercise, Physical Therapy, Lifestyle, (avoid excessive toxins like alcohol and nicotine), Medications, Environmental Modifications.
SOURCES: WebMD, NIH, Mayo Clinic, Alzheimer’s Association, American Cancer Society, American Heart Association, American Diabetes Association

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
