Spring is in the air. The temps are rising and the days are longer, so get outside and walk! Walking can change the world…from Mahatma Gandhi and the Indian independence movement to Martin Luther King, Jr., and the civil rights movement, walking and protest have been interrelated. Moreover, walking has been associated with fostering good health and stimulating creativity.
Walking is about more than walking and always has been. Walking soothes. Walking inspires and sharpens the mind. WE CAN WALK!
It might be said that with the right mindset, every walk is a pilgrimage. Many breakthroughs has been stumbled upon while putting one foot in front of the other. We run from problems. We walk toward solutions. While working on A Christmas Carol, Charles Dickens would walk 15 or 20 miles through the back streets of London, turning over the plot in his mind as the city slept. Beethoven found inspiration while ambling in the verdant Wienerwald outside Vienna.
Recent studies suggest that walking stimulates our creative mind is at its most creative at three miles per hour, the speed of a moderately paced stroll. Stanford University researchers divided participants into two groups: walkers and sitters. They then administered a test designed to measure creativity. They found that creative thinking was “consistently and significantly” higher for the walkers than the sitters. It didn’t take a lot of walking to boost creativity, either—anywhere from 5 to 16 minutes.
Studies have also shown that people who walk regularly are healthier and live longer than those who don’t. Surprisingly, you don’t have to walk very fast or far to enjoy this benefit. One recent study, published in JAMA Internal Medicine, put the 10,000-step myth to rest. It is an arbitrary number. People—older adults in particular—accrue health benefits by taking only a few thousand steps each day, and at a leisurely pace.
In addition to stimulating creativity and reducing stress, walking has many benefits. “There’s no question that increasing exercise, even moderately, reduces the risks of many diseases, including coronary heart disease, breast and colon cancer, and Type 2 diabetes,” said Dr. Jennifer Joyce, MD, professor of family medicine at GCSOM. “Research has even shown that you could gain two hours of life for each hour that you exercise regularly.”
According to the American Heart Association, walking as little as 30 minutes a day can provide the following benefits:
Like everything, there is a right way of doing something, even walking. For efficiency and safety, walking with proper stride is important. A fitness stride requires good posture and purposeful movements. Ideally, here's how you'll look when you're walking:
Anything is better than nothing! However, for most healthy adults, the Department of Health and Human Services recommends at least 150 minutes of moderate aerobic activity or 75 minutes of vigorous aerobic activity, or an equivalent combination of moderate and vigorous aerobic activity. The guidelines suggest that you spread out this exercise during the course of a week. Also aim to do strength training exercises of all major muscle groups at least two times a week.
As a general goal, aim for at least 30 minutes of physical activity a day. If you can't set aside that much time, try several short sessions of activity throughout the day. Even small amounts of physical activity are helpful, and accumulated activity throughout the day adds up to provide health benefits.
Remember it's OK to start slowly — especially if you haven't been exercising regularly. You might start with five minutes a day in the first week and then increase your time by five minutes each week until you reach at least 30 minutes.
For even more health benefits, aim for at least 60 minutes of physical activity most days of the week.
Keeping a record of how many steps you take, the distance you walk and how long it takes can help you see where you started from and serve as a source of inspiration. Record these numbers in a walking journal or log them in a spreadsheet or a physical activity app. Another option is to use an electronic device such as a pedometer or fitness tracker to calculate steps and distance.
Sources: National Geographic; Mayo Clinic
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Every December, as we finish the last of the leftover turkey, patients begin to talk about the holiday season and gift shopping. This conversation invariably leads to suggestions for gift ideas related to health, exercise and fitness. The suggestions below offer a wide variety of fitness-related gifts, some expensive and frivolous and others reasonably priced and practical. I hope it makes your shopping a little easier.
These gifts can be purchased at most local sporting goods stores or on-line.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

More than 65 million people, almost 30% of the population in the United States, are actively involved in providing 20 or more hours of care for a chronically ill, disabled, or aged family member or friend each week. As our population continues to age, this number is expected to grow rapidly.
The role of a caregiver is multifaceted and often involves tasks and skills beyond the education or comfort level of most providers. Some examples include; managing money, paying bills, shopping, cleaning, maintaining and repairing a home, dispensing and injecting medications, cleaning wounds, changing dressings, catheter management, bed baths, assisting in position changes, transferring from the bed to the chair, ambulation, stair climbing, bathroom assistance for toileting and showering and many other responsibilities. Consequently, a caregiver is often at risk for mental, spiritual and physical fatigue or breakdown. It is no surprise that depression, illness and injury often plague a caregiver and eventually, the caregiver is in need of a caregiver. One of the most common injuries suffered by a caregiver is back pain.
Lower back pain (LBP) is one of the most common problems in our society. Over 90% of all Americans will suffer from it at least once in their lives. It is generally agreed that prevention is the best treatment for LBP.
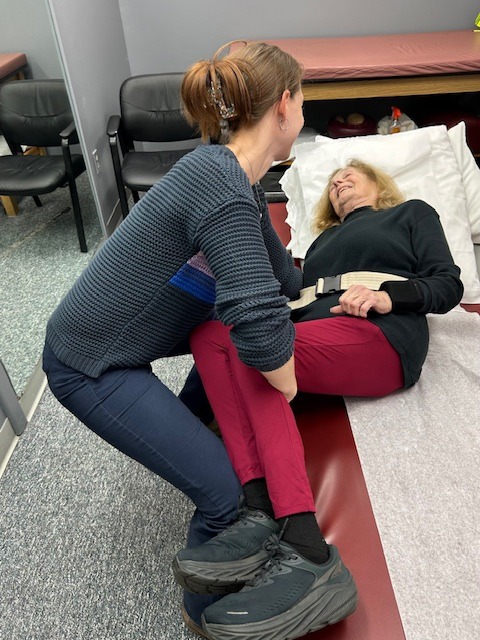
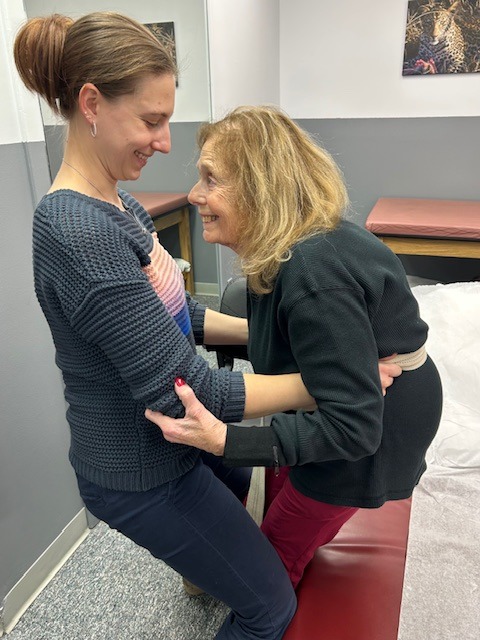
MODELS: Andrea Molitoris Kozlowski, PT, DPT, Associate Mackarey Physical Therapy, Doris Koloski, Scranton

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Here are 10 most common exercise myths!

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

While I fully expect to be at the “butt end” of many comments for this column, I feel compelled to address this topic at the request of several patients. It seems that many geriatric physical therapists commonly encounter patients that suffer from constipation which limits their participation in rehabilitation. Ironically, research demonstrates that exercise and activity actually help relieve constipation.
The National Digestive Diseases Information Clearinghouse (NDDIC) reports that 3.1 million people in the United States suffer from constipation. The NDDIC further reports that this problem leads to almost 400,000 hospitalizations, 1.4 million visits to emergency rooms, 1 million prescriptions and 121 deaths each year. Constipation is defined by the Ohio University College of Osteopathic Medicine as three or less bowel movements per week. It is also estimated that more than 27 percent of the elderly are affected.
Severe constipation can result in immediate medical attention in some cases due to intestinal obstruction. In addition to infrequent bowel movements, some symptoms include: feeling poorly, weight loss, loss of appetite, abdominal distention and/or pain, and vomiting.
Healthy people must continue to keep active. Get into good exercise habits at a young age and continue through life. Maintaining a consistent schedule of eating and exercise is also helpful. Some simple suggestions for beginning an exercise program for prevention of constipation in the healthy population are:
Depending on your general health and ambulatory status, these endurance exercises may be appropriate for you. Therefore, consider one or two of the following as a good starting point:
IN CONCLUSION: KEEP MOVING YOUR BODY AND YOU WILL KEEP MOVING YOUR BOWELS!
Visit your doctor regularly and listen to your body.
Keep moving, eat healthy foods, exercise regularly, and live long and well!

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

PIAA fall sport teams will begin their official practices a soon – including double sessions for high school football. While a warm August may be a wonderful time of year to swim and kayak, it may not offer the best temperature and humidity for athletes playing football, soccer and other sports. One common problem these athletes suffer from is severe muscle cramping. Every year multiple players limp off the practice field in pain and many concerned players, parents and grandparents repeatedly ask me about the problem. What exactly is a muscle cramp? Why does it happen? How can it be prevented?
A muscle cramp is defined as an involuntary contraction or spasm of a muscle that will not relax. The tight muscle spasm is painful and debilitating. It can involve all or part of the muscle and groups of muscles. The most common muscles affected by muscle cramps are gastrocnemius (back of lower leg/calf), hamstring (back of thigh), and quadriceps (front of thigh). Cramps can also occur in the abdomen, rib cage, feet, hands, and arms. They can last a few seconds or 15+ minutes. They can occur once or multiple times. It can cause very tight spasms or small little twitches.
Although the exact cause may be unknown at this time, there are several theories why muscle cramps occur. According to the American Academy of Orthopaedic Surgeons, when a muscle is flexible and conditioned, the muscle fibers are capable of changing length rapidly and repeatedly without stress on the tissue. Also, overall poor conditioning or overexertion of a specific muscle leads to poor oxygen/carbon dioxide exchange and build up of lactic acid and cause a muscle spasm. Also, this process can alter muscle spindle reflex activity and stimulate the spinal cord to send a message to the muscle to contract. If uncontrolled this leads to cramps and spasm.
Muscle cramps are more common in hot weather due to loss of body fluids, salts, minerals, potassium, magnesium and calcium. This leads to an electrolyte imbalance which can cause a muscle to spasm.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

After such a long, cold and wet spring, we are all grateful that the 4th of July holiday weekend is here! There is still plenty of time to be outdoors in NEPA and experience so many activities such as: biking, hiking, running, walking, swimming, boating, golfing, and playing tennis to name a few. It is a wonderful opportunity to discover your inner child, mix it up and try something new! Below are some new and exciting ways to stay active and have fun in the sun:
Spending time on any of the beautiful lakes in NEPA is time well spent. From an exercise standpoint, rowing, canoeing and kayaking offer a very special experience. Most kayaks are light weight, easy to use and maneuverable on a lake. Sitting low on the water offers a unique perspective as you feel yourself gliding across the lake. The Countryside Conservancy, in partnership with Lackawanna State Park, sponsors moonlight kayak events on the lake at the park. With a bright full moon, you can begin at 8 pm and return at 10 pm. Bring bug spray and headlights to enjoy the sunset and moon rise on the lake. You will feel like a kid breaking the rules of the park by being on the water after dark!
NOTE: Try kayaking in the daytime first and then advance to sunset trips before staying on the water for the moonlight. Rentals are available at the park.
Website: www.countrysideconservancy.org; www.dcnr.state.pa.us/stateparks.org
Stand up paddleboarding (SUP) is becoming a fast-growing sport among water enthusiasts. It is a fun way to exercise your core, improve balance, and tone your upper body. Stand Up Paddleboarding requires minimal equipment; a board that is essentially a long and wide surfboard and a long paddle to use while standing on the board. It can be done in the ocean surf, bay, lakes, or rivers; however, beginners would be wise to stay in calm water. Rentals are available at most beaches.
Check out the video for more information: REI paddleboard basics
What is it? Imagine a standup paddleboard with a handlebar and pedals like a exercise stepper machine. Instead of using a paddle, you step up and down on the pedals and fins under the board propel you through the water.
Check it out…Hobie Mirage Eclipse Stand Up Pedalboard; Dick’s Sporting Goods
Zumba is a very popular form of dance aerobics spiced up with Latin music. When adding water and sun to this already cool activity, you are assured to have fun while exercising. As with any aquatic exercise, the added resistance from the water gives arm rows and leg kicks more challenge. Female participants report an additional benefit; they are uninhibited to “shake that thing” to the music under the cover of the water. So, beat the heat, let loose and get some fun in the sun while you exercise.
NOTE: Consider trying regular Zumba first to get the hang of it. Amy Sekol is a local certified Zumba instructor and also offers Aqua Zumba. (amys.zumba.com)
Website: www.zumba.com
I love this idea…why didn’t I think of it first! In the gym I enjoy the elliptical machine because it simulates running without the impact on my joints but of course, I would rather be outdoors. Well, this is the answer to my prayers…an elliptical machine that is attached to a bike with handle bars and brakes included. I think it will probably be difficult on steep hills but it is something I MUST TRY!
Website: www.elliptigo.com; www.mywingflyer.com
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

As most sports enthusiasts know, in 2021 Tiger Woods ruptured his Achilles tendon while training at home and in 2023 Aaron Rodgers, a former Green Bay Packer quarterback, did the same in the first game of the 2023/24 NFL season with the New York Jets. As with many sports injuries, it is painful and devastating and best managed by PREVENTION!
Spring is here and as the days continue to get longer and temperatures begin a slow steady rise, athletes and weekend warriors are eager to get outdoors to play and exercise. However, be mindful of the weather (damp and rainy), temperature (cool mornings and evenings) and winter “dust” on your muscles and tendons. Many overjealous fitness enthusiasts will rush to pound the pavement and barely “fit in” a warm-up before participating. But, no matter how limited time is, skipping the warm-up is risky.
This time of year, one can expect to feel a little cold and stiff, especially if you are over 40, and therefore a little caution and preparation are in order to avoid muscle/tendon strain, or worse yet, muscle/tendon tears. The Achilles tendon is one of the more common tendons torn. Prevention of muscle tears, including the Achilles tendon includes; gradual introduction to new activities, good overall conditioning, sport specific training, pre-stretch warm-up, stretch, strengthening, proper shoes, clothing, and equipment for the sport and conditions.
A muscle contracts to move bones and joints in the body. The tendon is the fibrous tissue that attaches muscle to bone. Great force is transmitted across a tendon which, in the lower body, can be more than 5 times your body weight. Often, a tendon can become inflamed, irritated, strained or partially torn from improper mechanics or overuse. Although infrequent, occasionally tendons can also snap or rupture. A tendon is more vulnerable to a rupture for several reasons such as a history of repeated injections of steroids into a tendon and use of medications such as corticosteroids and some antibiotics. Certain diseases such as gout, arthritis, diabetes or hyperparathyroidism can contribute to tendon tears. Also, age, obesity and gender are significant risk factors as middle-aged, overweight males are more susceptible to tendon tears. Poor conditioning, improper warm-up and cold temperatures may also contribute to the problem.
Tendon rupture is very painful and debilitating and must not be left untreated. While conservative management is preferred, surgical management is usually required for complete tears. The purpose of this column is to present the signs, symptoms and management of Achilles tendon ruptures.
The Achilles tendon (also called the calcaneal tendon), is a large, strong cordlike band of fibrous tissue in the back of the ankle. The tendon (also called the heel cord) connects the powerful calf muscle to the heel bone (also called the calcaneus). When the calf muscle contracts, (as when you walk on the ball of your foot), the Achilles tendon is tightened, tension is created at the heel and the foot points down like pushing a gas pedal or walking on tip of your toes. This motion is essential for activities such as walking, running, and jumping. A partial tear of the tendon would make these activities weak and painful, while a full tear through the tendon would render these activities impossible.
With age, the Achilles tendon (and other tendons) gets weak, thin, and dehydrated, thus making it prone to inflammation, degeneration, partial tear or rupture. The middle-aged weekend warrior is at greatest risk. A full or complete tear (Achilles tendon rupture) usually occurs about 2 inches above the heel bone and is associated with a sudden burst of activity followed by a quick stop or a quick start or change in direction, as in tennis, racquet ball, and basketball.
In some instances, the tendon can be injured by a violent contraction of calf when you push off forcefully at the same time the knee is locked straight as in a sudden sprint. Other times, the tendon is injured when a sudden and unexpected force occurs as in a trip off a curb or sudden step into a hole or a quick attempt to break a fall.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
Next Week: Achilles tendon Part II of II
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

At least once a week, a patient jokingly asks if they can get a “lube job” to loosen up their stiff knee joint. I respond by providing them with information about osteoarthritis and viscosupplementation, a conservative treatment administered by injection and approved by the FDA for the treatment of osteoarthritis of the knee.
Osteoarthritis (OA) is also known as degenerative arthritis. It is the most common form of arthritis in the knee. OA is usually a gradual, slow and progressive process of “wear and tear” to the cartilage in the knee joint which eventually wears down to the bony joint surface. It is most often found in middle-aged and older people and in weight bearing joints such as the hip, knee and ankle. Symptoms include: pain, swelling, stiffness, weakness and loss of function.
Your family physician will examine your knee to determine if you have arthritis. In more advanced cases you may be referred to an orthopedic surgeon or rheumatologist for further examination and treatment. It will then be determined if you are a candidate for viscosupplementation. While this procedure is the most commonly used in the knee, it has also been used for osteoarthritis in the hip, shoulder and ankle.
Viscosupplementation is a procedure, usually performed by an orthopedic surgeon or rheumatologist, in which medication injected into the knee joint acts like a lubricant.
The medication is hyaluronic acid is a natural substance that normally lubricates the knee. This natural lubricant allows the knee to move smoothly and absorbs shock. People with osteoarthritis have less hyaluronic acid in their knee joints. Injections of hyaluronic acid substances into the joint have been found to decrease pain, improve range of motion and function in people with osteoarthritis of the knee.
When conservative measures, such as anti-inflammatory drugs, physical therapy, steroid injections fail to provide long lasting relief, viscosupplementation may be a viable option. Often, physical therapy and exercise are more effective following this injection to provide additional long-term benefit. Unfortunately, if conservative measures, including viscosupplementation fails, surgery, including a joint replacement may be the next alternative.
In 1997 the FDA approved viscosupplementation for osteoarthritis of the knee. Presently, there are several products on the market. One type is a natural product made from the comb of a rooster. However, if you are allergic to eggs or poultry products or feathers, you should not use the natural product. The other medication is best used for patients with allergies because it is manufactured as a synthetic product.
The long-term effects of viscosupplementation is much greater when other conservative measures are employed:
SOURCES: Genzyme Co, Sanofi-Synthelabo Inc, Seikagaku Co. and American Academy of Orthopaedic Surgeons
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
April is National Stress and Anxiety Awareness Month! According to the National Institutes of Health, an estimated 19.1% of U.S. adults 18 and older had an anxiety disorder in the past year. Anxiety disorders were higher for females (23.4%) than for males (14.3%). An estimated 31.1% of U.S. adults experience an anxiety disorder at some time in their lives.
There are a wide variety of anxiety disorders and will vary by the objects or situations that induce them. However, the features of excessive anxiety and related behavioral disturbances are similar. Anxiety disorders can interfere with daily activities such as job performance, schoolwork, and relationships. Symptoms include: distress, nausea, shortness of breath, bowel pattern changes, excessive perspiration, frequent laughing or crying, restlessness, and is often associated with depression. While there are many types and degrees of anxiety and there is no substitute for medical and psychological care, there are some simple and basic tools to help manage the problem…daily exercise is one easy, affordable and accessible suggestion for most. Multiple studies have discussed the incidence of unhealthy self management of anxiety, including the use of alcohol and recreational drugs.
Last week, I presented coping tips for the management of anxiety. In this column, I will discuss one of the most understated benefits of exercise – mental health! Specifically, aerobic exercise (exercise that increases your heart rate for 30 minutes or more) such as walking, biking, running, swimming, hiking, elliptical & stepper machines to name a few, is the secret to “runner’s high.” This exercise euphoria is not limited to runners alone, but all who engage in aerobic exercise are more likely to experience high energy, positive attitude and mental wellness.
Physical activity, specifically aerobic exercise, is a scientifically proven useful tool for preventing and easing anxiety and depression symptoms. Studies in the British Journal of Medicine and the Journal of Exercise and Sports Science found that anxiety and depression scores were significantly reduced in groups that engaged in aerobic running, jogging or walking programs, 30-45 minutes 3-5 days per week for 10-12 weeks, when compared to a control group and a psychotherapy counseling group.
According to research reported in sports medicine journals, exercise reduces anxiety and depression in two ways, psychologically (mentally) and physiological (physically).
SOURCES: University of Pittsburgh Medical Center (UPMC); National Institutes of Health (NIH); The American Journal of Sports Medicine
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
