Ice baths have become a new trend or fad in health and fitness, especially among elite athletes and some celebrities. However, it is far from a new treatment modality. In fact, the Ancient Greeks employed cold-water immersion for fever, pain relief, relaxation and socialization. In addition, Hippocrates documented the use of cold for medicinal purposes for its analgesic benefits.
Ice baths, a type of cryotherapy, is also referred to as cold water immersion (CWI) or cold water therapy. This involves immersing your body in ice water for approximately 5-15 minutes from the neck down at 50-59 degrees. The ice baths are commonly used for pain, delayed-onset muscle soreness (DOMS), and inflammation and mood elevation.
In theory, the cold water lowers the temperature of your skin and body by vasoconstriction (narrow) of the blood vessels. When you get out of the cold, water the vasodilatation (widen) of the blood vessels. Immediately, this brings fresh oxygen and nutrient-rich blood back to the tissues to warm the body and in the process, reduce pain, inflammation and promote healing.
If you have the following health conditions, ice baths may not be the best therapeutic modality for you. Before you consider trying an ice bath, consult with your physician to avoid potentially serious problems:
While some studies have shown that subjects report less muscle soreness following CWI when compared to rest, most studies suggest that the reported effects are placebo. Also, reports of improved circulation, reduced inflammation and improved recovery or performance has not been scientifically validated. In view of this, it is recommended that those considering the use of CWI for pain and inflammation management, reduced muscle soreness, and mood elevation, should consult their physician to determine if the potential risks are worth the purported benefits.
SOURCES: nih; health.com; health.clevelandclinic.org; prevention.com

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
During a recent “lunch-and-learn” meeting at our office, several younger staff members were discussing the use of supplements to compliment their fitness routines. One such staff member, Lily Smith, a physical therapy student aid at our clinic from the University of Scranton, is also a serious weight training and fitness enthusiast and shared her experience with creatine supplements with the hope of educating others, especially those preparing to “get fit” in 2024!
A National Health Interview survey found the creatine use among adolescents and young adults to be 34%. It is also very popular in the military with 27% average usage. While athletes and exercise enthusiasts use protein shakes and creatine supplements with hopes to improve size, strength and performance, it appears that most users do not have a full understanding of the risks and benefits. In view of this, today address the use of creatine in strength training and make recommendations based on the literature.
As long as I can remember, young athletes would take or do anything that they believed would improve their speed, strength, agility and athletic edge in order to succeed in sports. Running with weights wrapped around the ankles, drinking raw eggs and whole milk, and consuming copious amounts of beef, pork, and chicken were not unusual. Today, it may not be much different. However, the products do not come from our kitchen cabinet and tremendous misinformation is associated with it. Creatine is one example that was purported to enhance performance as early as the 1970’s but only gained popularity in the 1990’s. 40% of all college athletes and 50% of professional athletes admit to using creatine at some point, despite a lack of scientific evidence to support its effectiveness or safety.
This supplement is a natural substance that turns into creatine phosphate in the body. Creatine phosphate helps produce adenosine triphosphate (ATP), which provides energy for muscles to contract. While the body produces some creatine, it can also be found in foods rich in protein such as meat and fish. Manufacturers claim that creatine use will improve strength, increase lean muscle mass and aide in the recovery from exercise induced fatigue.
While creatine is popular among young people due in part to its availability, very little research has been done in people under 18 years of age. Even in the few studies conducted on adults, the results regarding efficacy are mixed. Some studies show that creatine may improve strength performance due to the recovery cycle of ATP. In theory, the use of creatine is purported to allow one to recover more quickly from exercise. For example, shortly after lifting heavy weights to failure, a quick recovery might allow the weight lifter to lift an additional set of repetitions to increase the duration of intensive training. Therefore, based on this theory, one must work out to complete failure during training to benefit from creatine. However, it is important to remember, there is no evidence that this purported benefit is realized in performance improvement in weight training or endurance sports.
Furthermore, no studies support the notion that it improves performance in endurance sports. Also, research does show that not all users are affected by creatine the same way. Most users fail to find any benefit at all. More concerning to this author is the fact that there are no guidelines for safety or disclosure of side-effects from long term use. Make no mistake, based on the research and current wisdom, CREATINE IS AN UNPROVEN TREATMENT SUPPLEMENT!
If one decides that creatine is a product they would like to use, despite the lack of evidence for its effectiveness, there are recommendations that one should follow for proper use. But there is no consistently established dose. Some studies have found 25 grams daily for 14 days as a “kickstart” dose or “loading” phase followed by 4-5 grams (or 0.1 g/kg of bodyweight) daily for 18 months with few side effects such as: muscle cramps, dehydration, upset stomach, water retention/bloating with weight gain. It is important to remember when establishing a dosage that many weight training supplements already contain creatine and in high doses excess creatine is excreted by the kidneys. It is also recommended that creatine users “wean off” the product when they decide to discontinue use.
Remember, an average adult in the United States receives 1 to 2 grams of creatine each day from a normal, well-balanced diet. Creatine is naturally found in meat, poultry and fish and theoretically, one could increase their creatine intake through dietary changes. Some manufacturers recommend 10 to 30 grams per day with a maintenance dose of 2 to 5 grams per day for athletic performance. Creatine is available in many forms; tablets, capsules and powder. It should be kept in a cool, dry place out of direct sunlight.
Creatine use is not recommended if you are pregnant, breast feeding, have kidney disease or bipolar disorder. There are many reported side effects associated with creatine use such as; water retention, nausea, diarrhea, cramping, muscle pain and high blood pressure. It is recommended that users consume large quantities of water when taking creatine to prevent dehydration. It may be very dangerous to use creatine when dehydration or weight loss is associated with an activity such as wrestling or summer sessions during football.
Furthermore, some studies show that large amounts of carbohydrates may increase the effects of creatine and caffeine may decrease the effects. Users are warned that using creatine with stimulants such as caffeine and guarana (a Brazilian plant extract similar to caffeine found in energy drinks) can lead to serious cardiac problems. The effects of creatine supplements on the many organ systems of the body are unknown. High doses may cause kidney damage. Although no cases have been reported in the literature, it is not known how it may interact with other supplements, over-the-counter medications and prescription drugs.
In conclusion, despite the lack of scientific evidence that creatine is more effective than proper nutrition and effective weight training, it remains a popular, easily available supplement purported to improve strength, endurance and performance in athletes. While relatively safe if taken as directed, it is always wise to consult your physician, especially if you have a history or risk of kidney problems. And, by the way, Lily did not feel that creatine supplements made any significant difference, positively or negatively. She no longer uses it due to the expense, inconvenience and lack of scientific evidence to support its efficacy.
Sources: University of New England; Medicine & Science in Sports & Exercise; NIH and Lily Smith, PT student, University of Scranton, Student PT aide, Mackarey Physicla Therapy
.Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
January is the time of year that many people set goals and resolve to be their very best. Not surprisingly, weight loss and fitness are the most common resolutions. It is also a time when many residents of NEPA will plan vacations and travel to warmer climates. Well, it may be that you can do both… This year consider visiting a “Fitness Resort.” According to “FitStays,” fitness resorts are rapidly gaining popularity for people of all sizes and shapes. Last week in Part I of “Fitness Resorts” we discussed value of fitness resorts. This week we will present “a typical day, how long you should stay, expected costs, and some recommended resorts.
A fitness resort is a vacation destination where travelers go to exercise and lose weight. Sometimes called a “weight loss resort”, “fitness retreat”, “wellness resort”, “weight loss boot camp”, or “adult fat camp”, fitness resorts around the United States cater to people of all shapes and sizes.
Most fitness resorts consist of pre-determined, calorie-limited menus to help travelers in their weight loss journey. Some resorts promote menus of 1,000 to 1,500 calories-per-day, which is fewer than most people burn naturally via their resting metabolic rate (RMR).
In addition to net-negative calories through nutrition, fitness resorts and retreats typically have an extensive workout plan as part of their standard program. Many resorts and retreats offer daily hiking, in addition to strength classes, cardio, sports, and other physical activities.
The combination of healthy nutrition and active exercise means that most visitors can expect to lose weight at a fitness resort. Specific weight loss goals are determined by which fitness resort you pick, how long you stay, and how strenuously you want to stick to the program.
Fitness resorts (fitness retreats) are not your average “Reality TV Fat Camp.” In fact, your do not have to be excessively overweight to attend as people of all shapes and sizes benefit and enjoy the experience. Thousands of people chose to visit fitness resorts and fitness retreats every year because they are looking for a healthy alternative to a typical vacation. Instead, many want to “kick-start” a healthy lifestyle in a controlled environment. The basic concept of combining a limited-calorie diet with daily exercise, most people will have net-negative calories every day, lose weight, and gain strength and endurance at a fitness resort—provided they stick to the program.
Typically, fitness resorts offer one week programs but multiple weeks with a variety of options are available. However, for the best outcomes and carryover, experts recommend 2-3 weeks for your first visit to a fitness resort.
Fitness resorts, like everything else, vary in cost. According to FitStay, programs cost as little as $1,500 per week (all-inclusive), while some are more than $7,000 per week.
To choose the best fit for you, your budget, and goals, visit fitstay.com. Remember, most fitness resorts are all-inclusive, meaning that you won’t need to budget any extra for food. The program includes meals. Also, when choosing a fitness resort consider: location (where would you like to travel?); cost (how much can you afford to spend?); how long can you stay (one, two or three weeks?)
NOTE: One of these includes a fitness retreat in our very own Pocono Mountains!

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!
January is the time of year that many people set goals and resolve to be their very best. Not surprisingly, weight loss and fitness are the most common resolutions. It is also a time when many residents of NEPA will plan vacations and travel to warmer climates. Well, it may be that you can do both…this year consider visiting a “Fitness Resort!” According to “FitStays,” fitness resorts are rapidly gaining popularity for people of all sizes and shapes.
A fitness resort is a vacation destination where travelers go to exercise and lose weight. Sometimes called a “weight loss resort”, “fitness retreat”, “wellness resort”, “weight loss boot camp”, or “adult fat camp”, fitness resorts around the United States cater to people of all shapes and sizes.
Most fitness resorts consist of pre-determined, calorie-limited menus to help travelers in their weight loss journey. Some resorts promote menus of 1,000 to 1,500 calories-per-day, which is fewer than most people burn naturally via their resting metabolic rate (RMR).
In addition to net-negative calories through nutrition, fitness resorts and fitness retreats typically have an extensive workout plan as part of their standard program. Many resorts and retreats offer daily hiking, in addition to cardio and strength classes and assorted sports and other physical activities.
The combination of healthy nutrition and active exercise means that most visitors can expect to lose weight at a fitness resort. Specific weight loss goals will be determined by which fitness resort you pick, how long you stay, and how strenuously you want to stick to the program.
Fitness resorts (fitness retreats) are not your average “Reality TV Fat Camp.” In fact, you do not have to be excessively overweight to attend as people of all shapes and sizes benefit and enjoy the experience. Thousands of people chose to visit fitness resorts and fitness retreats every year because they are looking for a healthy alternative to a typical vacation. Instead, many want to “kick-start” a healthy lifestyle in a controlled environment.
Fitness resorts have been found to be effective for most attendees. The basic concept of combining a limited-calorie diet with daily exercise, most people will have net-negative calories every day, lose weight, and gain strength and endurance at a fitness resort—provided they stick to the program.
While some people report losing 1-3 pounds-per-week at a fitness resort, others experience much more success. Exactly how much you will lose will be dependent on a wide variety of factors, including the duration and intensity of your exercise and activities and the calories you consume. Inherently, men tend to lose weight more easily than women, and younger people typically have an easier time shedding pounds than older people.
Ideally, for long term success, a fitness resort program should be a part of a healthy lifestyle, rather than an absolute weight loss goal. Be aware that many “spas and wellness centers” entice people with lavish facilities in a beautiful environment but mostly offer passive modalities such as massage, meditation, acupuncture, manicures, pedicures and facials. While these modalities have value, if your goal is jump start on weight loss and physical fitness, a fitness resort may be a better option.
Most fitness resorts are not “diet retreats” or painful “boot camps.” With a little effort, you can easily find the right fit for you. You will not starve! While you need to limit caloric intake, you also need enough energy for the 3-6 hours of exercise and activities (swimming, biking, hiking, Zumba, Yoga) offered. There is no need to be intimidated as most attendees are like-minded people with the same goals and needs. A good resort will not only provide the right amount of calories and exercise for your goals but also educate you how to prepare meals and engage in proper exercise once you return home.
According to FitStays, most fitness resorts offer a set schedule and a camp-like experience for adults with three meals every day, usually prepared by expert nutrition staff and/or dietitians, designed around healthy foods. A typical morning begins with extended cardio exercises, such as a run, bike or hike. The afternoon may have more intense exercise classes such as strength training classes as well as more fun activities such as sports and games. Educational classes are offered throughout the day, so you can carryover the lessons from your fitness resort experience when you return home. Evenings are usually lighter to allow for leisure, rest, or spa services, which are also offered at many resorts.

NEXT WEEK: FITNESS RESORTS - PART II – A typical day at a fitness resort, recommended length stay, cost and top 20 recommended resorts.
EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, please check out our exercise forum!
Last week we discussed the healthiest New Year’s Resolutions, however, given the fact that 80% of those who made resolutions will have failed by January 19th, this week I will recommend the use of technology to improve the odds…there is an App for that!
While some apps can be a waste of time, when you find the right app for you most polls show that it can be extremely helpful. They can be used for learning, socializing, calculating, writing, graphing, news, weather, music, school, money AND HELPING YOU KEEP YOUR NEW YEAR’S RESOLUTIONS!
According to “Per Statista,” the most common resolutions are as follows: save money (59%), exercise more (50%), more time with family and friends (40%), lose weight (35%), spend less money (26%), less time on social media (19%), and less job stress.
Goodbudget, YNAB (You Need A Budget), PocketGuard, and Quapital are some of the better budget Apps. Some of these Apps are free, while others require a nominal fee. In addition to tracking spending and saving, most allow you to set you own parameters and goals. Some helpful features are: moving money from checking into savings every time you buy a coffee.
In addition to wrist trackers like Fitbit and Smart Watches, there are exercise equipment options with programs and tracking like Peleton, Norditrack and exercise mirrors like Tonal. However, there are also specific Apps that help you set goals and see your progress. Some of these include: Fitness22, FitNotes, MyFitbnessPal and Strong. Some of these allow you to input your exercises and create graphs showing progress in body weight, fat percentage and more. These Apps are especially useful for those who dislike going to the gym.
While distance-base technology such as Skype, WhatsApp, and Zoom worked well to keep connected during the pandemic and after, there are other Apps that offer more personal ways. Cozi is one of the best as it offers a simple organizer that displays the schedule of the entire family to assist you in planning a get together. Cozi is a great option as a simple organizer that offers a clear visual representation of the entire family’s schedule. It not only shows when people are free but also tracks the amount of time you spend (or don’t spend) with these special people.
There are so many weight loss apps available that it is easy to get confused or overwhelmed. Some of the most popular with the best reviews are: Noom, Reverse Health, Perfect Body, WeightWatchers and MyFitnessPal. MyFitnessPal has the added benefit of tracking exercise and activity with a calorie expenditure report. Simply set a goal, enter food intake and exercise/activity output and the app calculates the rest. A bar-code scanner makes it even easier!
Keeping a better eye on finances and expenses is a common resolution, especially as the holiday bills come in. Stax Bill, NetSuite, Paystand and Rocket Money are highly rated. These apps help you budget, save, provide an income analysis and credit scores, and disclose recurring fees.
Reducing stress is another common resolution and learning stress management techniques and incorporating them into our daily lives is vital. Some of the highly rated apps are: Personal Zen, Sanvello, The Mindfulness App, Headspace and Moodfit. These apps not only give you the tools for managing stress but also provide insights into your mood patterns and stressors. In addition to a “blue mood” you can also track gratitude and other feelings. Also, nutrition, sleep, and medications, which can affect your mood, can also be tracked. Once a pattern is established, tools can be applied to reduce and manage stress.
While at first glance it may seem odd that one might use an app to stop using another app but…don’t rule it out! OneSec is an app that creates a 10 second delay after you open an app to allow you time to pause and take a deep breath before you indulge. It will also tell you how many times you have opened the app in the last 24 hours…you might be shocked!
SOURCE: LIFEHACKER

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: mmptc@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice in Scranton and Clarks Summit and is an associate professor of clinical medicine at GCSOM. For all of Dr. Mackarey's articles, visit our exercise forum!
New Year’s Resolutions are very predictable. While most New Year Resolutions are health oriented, I purport that a healthy mind, body and spirit requires a healthy lifestyle. Interestingly, the ten most popular resolutions listed below, all have an impact on a healthy life.
SOURCE: A. Powell, About.com Guide

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at GCSOM. For all of Dr. Mackarey's articles, visit our exercise forum!
Happy Holidays! It is at this time of year that we celebrate life with great hope and faith. People of many faiths take time to reflect, respect, and resolve. Christians celebrate Christmas, the miraculous birth of Christ, the Son of God, and the Messiah. Jews celebrate Chanukah, the miraculous festival of lights, when one night’s oil provided enough light and safety for 8 nights. Both major faiths promote healthy lifestyles for the mind, body and spirit. These faiths are grounded in hope, faith, love and peace. It is no surprise that studies repeatedly demonstrate that faithful and spiritual people live longer and healthier lives! At this turbulent time in the world, it is important to note that people of all faiths benefited equally!
With this in mind, I purport, that to be truly healthy, one must have faith because complete health is multidimensional. Socrates preached this message to his students thousands of years before Christ. One must have a healthy mind, which requires intellectual stimulation with attainable goals related to education and intellect. One must have a healthy body by eating well, engaging in physical activity and have attainable goals related to his/her body. Likewise, one must have a healthy spirit with faith, hope, prayer and meditation, comrades and counsel, and set attainable spiritual goals.
How being religious or spiritual has been shown to benefit your mind, body and spirit.
High blood pressure (hypertension) can lead to heart disease and stroke, which are the leading causes of death in the United States, according to the Centers of Disease Control (CDC). It affects 1 in every 3 adults and only half of these people have their blood pressure under control. Well, religion and spiritually may help …
The health benefits of religion or spirituality are well documented. One study conducted at Duke University Medical Center on 4,000 subjects, older adults who described themselves as religiously active were 40% less likely to have high blood pressure when compared to those less active. Moreover, they were surprised to find that those who described themselves as spiritual rather than religious also were less likely to develop high blood pressure.
Research also indicates that religious people are more satisfied with their lives than those without faith. A sociology study determined that high satisfaction among church goers may be due to the strong social bonds that are developed within a religious congregation. Regular church attendees see the same people weekly and often more often, when participating in rewarding and gratifying church-related volunteer work.
In an impressive study published in the Journal of the American Medical Association, researchers interviewed 345 late-stage cancer patients to assess their spirituality as it related to their illness. 88% stated that they were religious as it related to their coping mechanisms. It was determined that those using religion for coping demonstrated a 7.4% rate of resuscitation as compared to 1.8% for those not using religion as a coping mechanism.
According to a Duke University study of 1,718 older adult participants, those described as “highly spiritual” were 50% less likely to have high levels of anti-inflammatory proteins that weaken the immune system and have been linked to some cancers, viral infections and autoimmune diseases. The outcome was similar for those who attend religious services at least once a week.
Those who attend religious services more than once per week are found to live and additional 7 years when compared to those who never attend services. Again, researchers feel that the social benefits of a belonging to a strong religious community may be a large part of the associated longevity. Additionally, the lifestyle of religious people is often healthier: members of these communities rarely engage in risky and unhealthy behaviors such as smoking, excessive drinking, indiscriminate, unprotected sex, etc.
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice in Scranton and Clarks Summit and is an associate professor of clinical medicine at GCSOM. For all of Dr. Mackarey's articles, visit our exercise forum!
Every December, as we finish the last of the leftover turkey, patients begin to talk about the holiday season and gift shopping. This conversation invariably leads to suggestions for gift ideas related to health, exercise and fitness. The suggestions below offer a wide variety of fitness related gifts, some expensive and frivolous and others reasonably priced and practical. I hope it makes your shopping a little easier.
Dry Tech is the best thing that has happened to exercise apparel since “jogging suit” was donned by all the “cool dudes” in the 70’s and 80’s . It is has great style and even better function. The specially made material is light weight and breathable and wicks moisture from the skin to the outer layers. Therefore, it will not get heavy with sweat which can weigh you down and cause friction with your skin which can lead to chaffing and blisters. The following exercise apparel is now available in Dry Tech:
NOTE: Shoes are a very important aspect to safe and comfortable exercise but are unique for running and other specific sports (tennis, basketball). Sneakers may be too difficult to buy for someone else. A gift certificate to an athletic shoe store (Scranton Running or Dick’s) may be a better choice.
For walking and hiking enthusiasts, trekking poles can be the perfect gift, especially for those over 50 and when on uneven terrain or inclement weather. The research is compelling…less stress on the lower back, hip, knee and ankle, as well as improved balance and safety. Leki, Black Diamond, and Trekology are good name brands while LL Bean and REI are reputable companies.
An exercise mat is helpful if you decide to exercise at home. Also, a required equipment for participating in yoga or Pilates classes is a mat.
These are essential for those interested in home exercise. For the average beginner, 3-5-8-10 pound (two of each) weights will be adequate. Dumbbells are good for shrugs, biceps, and triceps, bent over rows and lats, and lunges. Incremented and stackable dumbbells are also available by Bowflex SelecTech 552 (5-52 pounds for $299). and NordicTrack $189. Sandbags, which can be purchased as graduated weights from 1 to 5 pounds, are good for leg extensions, hamstring curls, hip hikes and hip abduction.
These cheap and versatile bands are also essential for a home program. The bands come in different colors to represent the amount of resistance with yellow being the easiest and black the most difficult. They are useful for upper and lower body. For specific band exercises visit a previous column in “Health & Exercise Forum” at The Times Tribune or www.mackareyphysicaltherapy.com
NOTE: Peloton, NordicTrack, SoulCycle are some of the companies that offer interactive exercise programs (usually through an internet subscription) for aerobic exercise using bikes, treadmills, ellipticals or rowing machines.
This can be an opportunity for someone to either get the proper advice from a professional to begin a fitness program or to revamp and tune up an old stale program. Word of mouth is a good way to find a reputable certified trainer.
Peloton – ($2,495 bike, $3,495 treadmill); Mirror Exercise – ($1,495); Tonal ($3,995.) FightCamp – ($1,219.); Forme Studio ($2,495.)
These devices use GPS technology to help the user track their activity to get more out of their exercise routines. They monitor activity, heart rate, distance, location, calories, and more. Some examples are:
Sometimes you need professional help to get started and stay focused. Just as with a personal trainer, a qualified and licensed nutritional counselor will assist you in establishing a safe and effective program to meet your nutritional and dietary goals. Again, ask around to see who has a good reputation or who may be a good fit for the recipient of your gift.
These gifts can be purchased at most local sporting goods stores or on-line.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopaedic and sports physical therapy. Dr. Mackarey is in private practice, located in Scranton and Clarks Summit, and is an associate professor of clinical medicine at GCSOM. For all of Dr. Mackarey's articles, check out our exercise forum!
Holiday shopping is stressful for your body, causing backache, as well as your wallet. Even the “online shopper” is at risk when you consider the hours sitting with poor posture on your electronic device. But I do believe that “in person” shopping is worse for backache… driving from store to store, getting in and out of the car while bundled in a sweater and winter coat can add stress to your spine. Often, the expert shopper carries package after package from the store to the car, repeatedly. Six, eight, or ten hours later, the shopper arrives home exhausted with the backache slowly increasing, only to realize that 15 or 20 packages must be carried from the car into the house. This dilemma is compounded by the fact that the rain turned to sleet, and the sleet to snow. You are slipping and sliding all the way from the car to the house while carrying multiple packages of various sizes and shapes, fighting through the already developing backache. The shopping bags get wet and tear, forcing you to tilt your body as you carry the packages. Of course, no one is home to help you unload the car and you make the trip several times alone. You get into the house exhausted and crash onto the couch because your backache is too much to do anymore at this point. You fall asleep slouched and slumped in an overstuffed pillow chair. Hours later you wake up with a stiff neck and lower back pain. You wonder what happened to your neck and back.
Plan Ahead: It is very stressful on your spirit, wallet and back to do all of your shopping in the three weeks available after Thanksgiving. Even though we dislike “rushing” past Thanksgiving to the next holiday, try to begin holiday shopping in before
Use the Internet: Supporting local businesses is important. However, Internet shopping can save you lots of wear and tear. Sometimes, you can even get a gift wrapped.
Gift Certificates: While gift certificates may be impersonal, they are easy, convenient and can also be purchased over the internet.
Perform Stretching Exercises: Stretch intermittently throughout the shopping day…try the three exercises below, gently, slowly, hold 3 seconds and relax, repeat 5 times.



Model: Paul Mackarey, PT, DPT, Clinic Director, Mackarey PT
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

As most sports enthusiasts know, Aaron Rodgers, former Green Bay Packer quarterback and recent New York Jets QB (for just over a minute and half) suffered a season ending injury when he tore his Achilles tendon in the first game of the 2023/24 NFL season. Since then, I have been answering many questions from patients and sports fans about the nature of the Achilles Tendon rupture injury, recovery, and how to prevent it.
As the days continue to get shorter and temperatures begin a slow steady decline, athletes and exercise enthusiasts will work harder to warm-up and exercise during the winter months. A little caution and preparation are in order to avoid muscle/tendon strain, or worse yet, muscle/tendon tears, especially Achilles Tendon rupture. The Achilles tendon is one of the more common tendons torn.
This is the second of two columns on Achilles tendon rupture. Last week, I discussed the definition, sign and symptoms of the problem. This week will present examination, treatment and outcomes.
A thorough history and physical exam is the first and best method to assess the extent of the injury and determine accurate diagnosis. While a complete tear is relatively easy to determine, a partial or incomplete tear is less clear. Ultrasound and MRI are valuable tests in these cases. X-rays are not usually used and will not show tendon damage.
Consultation with an orthopedic or podiatric surgeon will determine the best treatment option for you. When conservative measures fail and for tendons completely torn, surgical intervention is usually considered to be the best option with a lower incidence of re-rupture. Surgery involves reattaching the two torn ends. In some instances, a graft using another tendon is required. A cast or walking boot is used post-operatively for 6-8 weeks followed by physical therapy.
Most people return to close to normal activity with proper management. In the competitive athlete or very active individual, surgery offers the best outcome for those with significant or complete tears, to withstand the rigors of sports. Also, an aggressive rehabilitation program will expedite the process and improve the outcome. Walking with full weight on the leg after surgery usually begins at 6 -8 weeks and often requires a heel lift to protect the tendon. Advanced exercises often begin at 12 weeks and running and jumping 5-6 months. While a small bump remains on the tendon at the site of surgery, the tendon is well healed at 6 months and re-injury does not usually occur.
Prevention of muscle and tendon tears is critical for healthy longevity in sports and activities. In addition to the Achilles tendon, the tendons of the quadriceps (knee) and rotator cuff (shoulder) are also vulnerable. A comprehensive prevention program includes: gradual introduction to new activities, good overall conditioning, sport specific training, pre-stretch warm-up, stretch, strengthening, proper shoes, clothing, and equipment for the sport and conditions. Also, utilizing interval training, eccentric exercise (lowering body weight slowly against gravity – Photo 1) and proprioceptive and agility drills are essential (Photos 2 & 3).
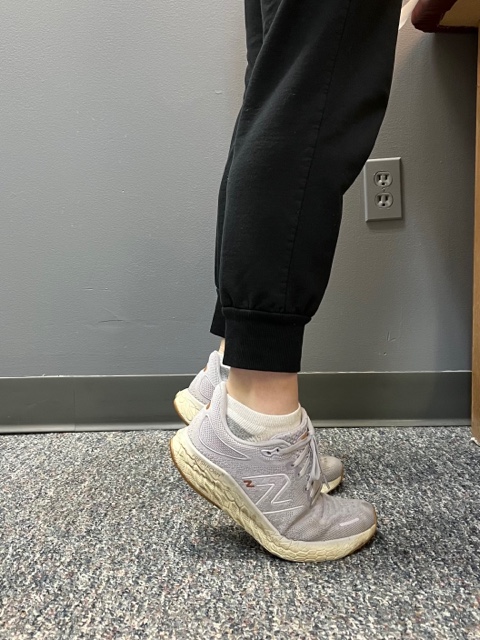

In PHOTO 1a & 1b: Eccentric Lowering and Lengthening: for the Achillies tendon during exercise. Beginning on the ball of both feet (1a), bend the strong knee to shift the weight onto the weak leg (1b). Slowly lowering the ankle/heel to the ground over 5-6 seconds. Repeat.
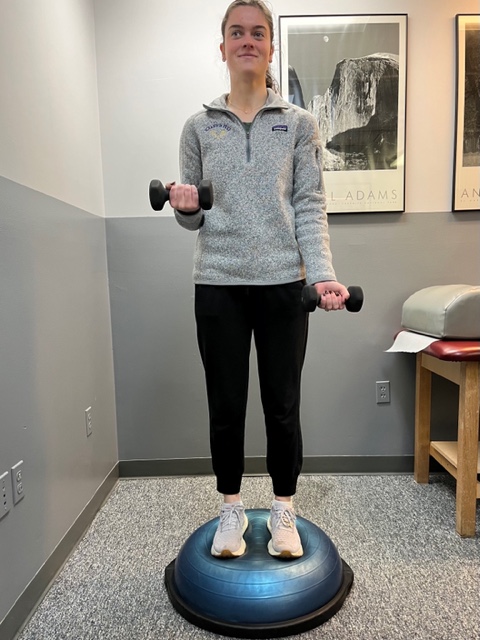
In PHOTO 2: Proprioceptive Training: for the Achillies tendon. Standing on a Bosu Ball while exercising the upper body (for example, biceps curls, shrugs, rows, lats) while maintaining balance on the ball.
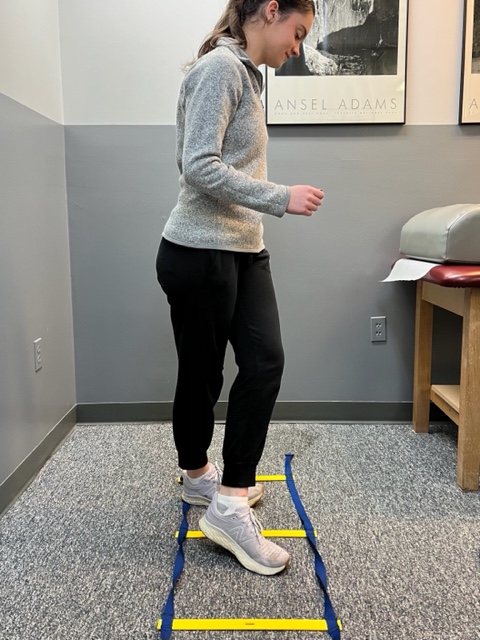
PHOTO 3: Agility Drills: for the Achilles tendon involves stepping through a “gait ladder” in various patterns and at various speeds.
MODEL: Kerry McGrath, student physical therapy aide at Mackarey Physical Therapy
Sources: MayoClinic.com;Christopher C Nannini, MD, Northwest Medical Center;Scott H Plantz, MD, Mount Sinai School of Medicine

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at GCSOM. For all of Dr. Mackarey's articles, visit our exercise forum!