May is National Bike Month! It is time to dust it off your bike and enjoy the many beautiful and well-maintained trails that are available at the Countryside Conservancy at Lackawanna State Park, Lackawanna Heritage Valley Authority and other locations in the Greater Scranton Area. For those who don’t have a bike, it might be a good time to get one!
There are many obvious reasons to bike…cardiovascular fitness, burn calories, improve leg strength and others. But the real question is, “what are the advantages of biking over other forms of exercise?” Glad you asked…
Prevention is the best management of musculoskeletal problems associated with biking. First, many of the problems associated with biking such as knee pain, buttock soreness, and tendonitis can be prevented through proper fitting. Furthermore, it is important that your equipment be in good working order, such as tires, chain, brakes and pedals. Next, be sure to maintain a reasonable fitness level in order to bike safely. If you are a beginner, start slowly. Warm up and slowly bike for 10 to 15 minutes and build up over time.
Practice the coordination of stopping, starting, shifting and braking. Work on good strength and flexibility of the hamstrings, quadriceps, calves and gluteal muscles. All of these muscles are necessary to generate pedal force. Balance is also important to safety and can be practiced on and off the bike. Be aware that adaptive equipment can modify your bike for added comfort and safety such as soft handlebar tape, seat post and front fork shock absorbers, padded biking shorts, c-out and gel pad saddle seats, and wider tires.
Be careful not to progress too quickly because inactivity to over activity in a short period of time can create problems. Overuse injuries such as tendonitis can be avoided by cross training. Bike every other day and walk, run or swim on off days. Make sure to take time off to recover after a long ride. Use ice and massage to sore muscles and joints after riding.
Remember, cycling should be fun! Pain from improperly fitted and poorly maintained equipment is preventable. Excessive workouts and training rides should be kept to a minimum and consider cross-training in between.
EQUIPMENT: Helmets are a must! Also, keep your bike in good condition. Road bikes should have mirrors and reflectors. Use hand signals and obey traffic rules. Dress for weather and visibility. Have first-aid and tire patch kit, tire pump and tools. Seat comfort can be improved with gel cushion or split seat.
BE ALERT: for traffic, parked cars, pedestrians’ loose gravel and cracks in the road.
SOURCES: American Physical Therapy Association
Visit your doctor regularly and listen to your body.
Keep moving, eat healthy foods, and exercise regularly

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

“The woods are lovely, dark, and deep,
But I have promises to keep,
And miles to go before I sleep,
And miles to go before I sleep.” Robert Frost
On March 30, 2026, NEPA lost one of its most dedicated conservationists, Dorrance Reynolds Belin…our version of John Muir, Theodore Roosevelt, and Rachel Carson. While Dorrance served on numerous boards, in my view, he will be most fondly remembered for his environmental stewardship as founder of the Eastern Pennsylvania Chapter of the Nature Conservancy and Countryside Conservancy. I am not sure if Dorrance ever had the pleasure of meeting Robert Frost, Pulitzer Prize winning American Poet, but it is not hard to imagine that he had Dorrance in mind when writing the above poem. Thank you Dorrance, and those who worked with you, for the vision and foresight to preserve these special places for our children, grandchildren and great grandchildren to enjoy!
According to their mission statement, The Countryside Conservancy manages 1,190 acres of lands and waters to protect their conservations value. Most of these acres are open to the public for visitation and many have trails. Collectively, the conservancy contributes to 10 miles of singletrack hiking and biking trials to the 30-mile Lackawanna State Park/Countryside Conservancy Trail System …for more information visit: countrysideconservancy.org.
Please get outdoors and enjoy the trails…walking, running, biking, snowshoeing, cross-country skiing or horse back riding. But if you want to try something new this spring that will allow you to exercise on more interesting and less stressful surfaces in the beautiful woods of Northeast Pennsylvania…try trail running!
Trail running forces one to run 25% slower due to the uneven terrain (rocks, tree roots, stumps), incorporate “light running” techniques by running with short strides on the balls of my feet. You will feel much more refreshed by avoiding the direct sunlight under the cover of the trees. Furthermore, you can enjoy the up-close view of nature as I ran by cool streams and wet mossy rocks, beautiful flowers, rhododendron, and mountain laurel. Observe deer, chipmunks and birds. In my quest to avoid the hot sun, I discovered the beautiful underworld of “trail running” - it is beautiful, peaceful, natural and unique. It is fun to get in touch with your inner child as you run in the woods and get muddy. Trail running makes running fun…and it’s good for your joints!
The trail running community purports that trail running is popular because it satisfies a primal need for man to move through nature, derived from hunter/gatherer days. Others who promote trail running feel the popularity is due to the many advantages it offers. One, trail running prevents impact injuries due to soft surfaces. Two, the training style of running with shorter strides on the ball of the foot, lessens impact. Three, this type of running will develop stronger ankles and trunk core muscles while improving balance, coordination and proprioception from running on uneven surfaces. Lastly, the ability to release copious amounts of endorphins while breathing fresh air instead of roadside fumes is invaluable.
Find a Trail – Start by asking around. Hikers, mountain bikers, and horseback riders are a good start. The American Trail Running Association has a website with a free directory of trails in the United States. PA State Parks such as Lackawanna State Park in Dalton, offer many options www.visitPAparks.com, countrysideconservancy.org. or download the app AllTrails. Learn the difference between “nontechnical trails” which are wider with a paved, dirt or gravel base and much easier than “technical trails” which are narrow, rocky, hilly and challenging.
Sources: American Trail Running Association, Trailspace.com, countrysideconservancy.org.
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Spring has sprung in NEPA and summer is just around the corner... great news for outdoor enthusiasts! It is also good news for those who need walk for health reasons. However, for many who have not maintained an active lifestyle or have health issues, it is challenging to know where to begin. Moreover, beginning without a good plan can lead to injury and leave you discouraged. For example, those overweight and de-conditioned should not start a walking program too aggressively. Walking at a fast pace and long distance without gradually weaning into it will most likely lead to problems.
There is probably nothing more natural to human beings than walking. Ever since Australopithecus, an early hominin (human ancestor) who evolved in Southern and Eastern Africa between 4 and 2 million years ago, that our ancestors took their first steps as committed bipeds. With free hands, humans advanced in hunting, gathering, making tools etc. while modern man uses walking as, not only a form of locomotion, but also as a form of exercise and fitness. It is natural, easy and free...no equipment or fitness club membership required!
“There’s no question that increasing exercise, even moderately, reduces the risks of many diseases, including coronary heart disease, breast and colon cancer, and Type 2 diabetes,” said Dr. Jennifer Joyce, MD, professor of family medicine at GCSOM. “Research has even shown that you could gain two hours of life for each hour that you exercise regularly.” A recent study demonstrated that a 15 minute walk after a meal is very effective in reducing blood sugar levels.
According to the American Heart Association, walking as little as 30 minutes a day can provide the following benefits:
Anything is better than nothing! However, for most healthy adults, the Department of Health and Human Services recommends at least 150 minutes of moderate aerobic activity or 75 minutes of vigorous aerobic activity, or an equivalent combination of moderate and vigorous aerobic activity. The guidelines suggest that you spread out this exercise during the course of a week. Also aim to do strength training exercises of all major muscle groups at least two times a week.
As a general goal, aim for at least 30 minutes of physical activity a day. If you can't set aside that much time, try several short sessions of activity throughout the day (3 ten or 2 fifteen minute sessions). Even small amounts of physical activity are helpful, and accumulated activity throughout the day adds up to provide health benefit.
Remember it's OK to start slowly — especially if you haven't been exercising regularly. You might start with five minutes a day the first week, and then increase your time by five minutes each week until you reach at least 30 minutes.
For even more health benefits, aim for at least 60 minutes of physical activity most days of the week. Once you are ready for a challenge, add hills, increase speed and distance.
Keeping a record of how many steps you take, the distance you walk and how long it takes can help you see where you started from and serve as a source of inspiration. Record these numbers in a walking journal or log them in a spreadsheet or a physical activity app. Another option is to use an electronic device such as a smart watch, pedometer or fitness tracker to calculate steps and distance.
Make walking part of your daily routine. Pick a time that works best for you. Some prefer early morning, others lunchtime or after work. Enter it in your smart phone with a reminder and get to it!
Studies show that compliance with an exercise program is significantly improved when an exercise buddy is part of the equation. It is hard to let someone down or break plans when you commit to someone. Keep in mind that your exercise buddy can also include your dog!
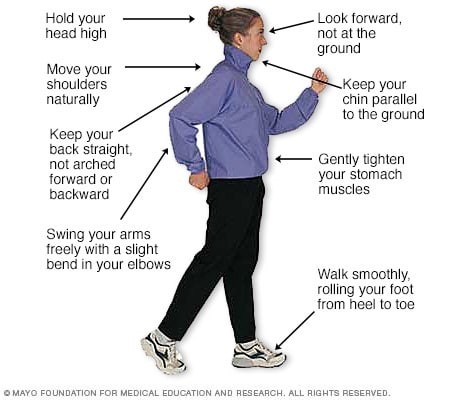
Like everything, there is a right way of doing something, even walking. For efficiency and safety, walking with proper stride is important. A fitness stride requires good posture and purposeful movements. Ideally, here's how you'll look when you're walking:
Sources : Sapiens.org; WebMD; Mayo Clinic
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Have you ever noticed high level athletes warming up before a game or competition walking or running backwards? You may also see fitness enthusiasts in gyms emulating these athletes to improve their fitness or performance. I found the concept of backward walking (also called retro walking) interesting and decided to research the topic for more information and validation. Walking backward does have many therapeutic benefits, however, before you attempt this activity on a treadmill or elliptical, please consult your physician and physical therapist and have a spotter nearby.
At a recent meeting of The American College of Sports Medicine, several studies were presented on the topic of backward waking. Most of the research was conducted while moving backward on a treadmill and an elliptical machine. When comparing two groups recovering from knee injuries, the backward motion group showed significant improvement in strength in the quadriceps (front thigh) and hamstring (back thigh) muscles when compared to the traditional forward walking group. Furthermore, the muscles of the front (tibialis anterior) and back (gastro/achilles) of the shin/ankle also demonstrated an increase in strength and endurance with backward walking. One explanation is that forward motion is routine in daily living that it has become very efficient and does not tax or stress the muscles the body. While this efficiency prevents fatigue in daily activities, it may not stress the muscles enough to gain strength as quickly as an unfamiliar exercise.
Due in great part to the increased strain of performing unfamiliar exercise, backward walking on a treadmill or backward pedaling on an elliptical, offered a greater cardiovascular benefit and caloric expenditure than forward motion at all levels. Specifically, walking backward on a treadmill at 2.5 mph at grades of 5% - 10% has been found to significantly increase cardiovascular endurance than walking forward under the same conditions. This knowledge is useful for healthy individuals in need of greater cardio exercise. However, it may also serve as a precaution for those with cardio problems and should consult their physician prior to engaging in this activity.
A recent study in the International Journal of Obesity, found that those who performed new activities or increased the intensity of an activity, even if for a short duration (interval training) expended more energy and burned more calories than those who worked out at the same pace consistently for a longer duration. Moreover, when engaging in a new activity such as backward walking, even more calories were burned. This phenomenon may be due to the fact that routine activities such as forward walking are performed more efficiently and easily.
We challenge our body when we inefficiently perform a new motor skill such as backward walking and burn more calories. In other words, if you want to burn more calories without exercising for longer periods of time, then try a new activity and engage in higher intensity, intermittently, for part of the time. For example, walk backward on the treadmill for 30 minutes at 2.5 mph, but do so at a 5 – 10% incline for 1-2 minutes every 5 minutes.
Some studies show that using other muscle groups by performing different exercises not only prevents boredom but also protects your muscles and tendons from overuse and joints from wear and tear. Specifically, the knee joint and the patella joint (the joint where the knee cap glides on the knee), benefit from backward walking due to less stress and compression forces on the joint. The thigh and ankle/foot muscles benefit from using a different form of contraction while lengthening the muscle. Some authors propose that this may also prevent strains and pulls and may be valuable to strengthen those with a history of shin splints and flat feet (pronation).
Mixing up your program prevents boredom. As a rule, those willing to change their exercise routine are more compliant and continue to exercise longer than those stuck in the same routine. A new challenge to improve distance, speed, and resistance while exercising in a different direction will be refreshing to your program.
Prevention of falls by improvement in balance and coordination has received a great deal of attention in the past few years. This is not only valuable to the athlete but may be even more important to those over 50. With age, balance centers are slow to react to changes in inclination, elevation, rotation and lateral movements. This slow reaction time leads to falls that may cause fractures, head injuries and more. Working on this problem by challenging the vestibular and balance centers before it is seriously compromised is important and backward walking is one way for this to be effectively accomplished.


Treadmill Backward Walking MODEL: Lexi DiGregorio, PTA
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Spring sports and outdoor activities are here…tennis, pickleball, baseball, soccer, running, walking, hiking, golfing, etc. One of the most common injuries associated with physical activity, especially after a sedentary winter or change in temperature is a “pulled hamstring.” This painful injury is not only for the weekend warrior. Well-trained, healthy and fit professional athletes often have their season interrupted for weeks and months due to a hamstring injury. What is the hamstring? How is it injured? What is the best treatment?
A hamstring strain is a tear of the muscle fibers of the muscle group in the back of the thigh called the hamstring. The hamstring muscle is a group of three muscles that run from the back of the hip (lower pelvis), crossing the back of the knee and attaches to the knee bone (tibia). The hamstring muscles work to extend the hip and bend the knee during running and walking activities. They are very active when an athlete changes direction, especially forwards and backwards or decelerating. This injury, like others muscle strains, varies in intensity.
Severe hamstring strain occurs when many muscle fibers are torn. The athlete may experience a sudden onset of severe pain in the back of the thigh and occasionally report a popping sensation. Pain, swelling and black and blue skin from tissue damage and bleeding is often reported. Also, pain is reproduced when attempting to bend the knee. In very severe cases, the boney attachment can be pulled so strongly that a small fracture can occur. Healing time can be as short as a few days or as long as weeks or even months.
Your family physician will examine the back of your leg to determine if you have hamstring strain. Sometimes, pain in the buttocks and back of the leg can be referred from your lower back if the sciatic nerve is inflamed. In more advanced cases, you may be referred to an orthopedic surgeon for further examination and treatment. An X-ray, MRI or bone scan will show the extent of the tear and if the bone is involved. The diagnosis will determine if your problem is minor, moderate or severe.
There are many conservative options. Your family physician or orthopedic surgeon will help you decide which choices are best.
Recent studies have determined that a training program specifically designed to prevent hamstring injuries is effective, especially for the competitive athlete. This program includes:
SOURCES: Journal of Physical Medicine & Rehabilitation and American Academy of Orthopaedic Surgeons
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

A health column about sugar for Easter??? Well, maybe this information will be more appropriate next week! For those trying to lose weight or “get in shape” for the “bathing suit season,” a better understanding of the role sugar plays in your diet and overall health may be valuable. You have probably noticed a lot of attention being paid to sugar lately. Many television stars and other celebrities have shared their experiences using a “sugar cleanse” when they need to lose a few pounds and get healthier.
I have had several patients and friends tell me the same thing. For 4-6 weeks these people decide to avoid all refined sugars with the goal of losing weight and improving their health and wellness. Well, what is all the fuss about? Terms like simple sugars and simple carbs, which are purported to be bad, and complex carbs, suggested to be good, are being used ad nauseam. While medical research does not support the value of a short term “sugar cleanse,” it may have value for another reason. For example, it would be very beneficial if one engages in a “sugar cleanse” for the purpose of changing their palate with the hope of developing long term healthy eating habits, especially for those with diabetes…to be implemented AFTER the Easter candy has been consumed!
So, with this in mind, I decided to find the answers to some simple questions about the fuss over sugar. What is a simple sugar? What is a complex sugar? Which sugars are good for you?
Sugars, along with starches and fibers, are one of three types of carbohydrates (also referred to as a carb). A carb is “simple” or “complex,” based on its chemical composition and how it is processed in the body. It gets a little complicated because some foods have both simple and complex carbs. Typically, simple carbs are chemically more “simple” and basic, and therefore they are broken down more easily and serve as a quick source of energy. Some of these carbs are naturally simple (like fruit and milk) while others are processed or refined sugars such as those used in candy, soda and baked goods.
To determine if a food product has good or bad simple sugar, you must also know how much fiber, vitamins and minerals are in the food. A food with a higher sugar content combined with a low fiber, vitamin or mineral content will be worse than a food with the same sugar content but high fiber and vitamins or minerals. For example: a candy bar, which is high in sugar without fiber or vitamins or minerals, is not as healthy as a fresh orange, which contains fiber, vitamins and minerals along with its simple sugar (fructose).
Complex carbs have a more complicated chemical makeup and take more time for the body to break down for use as energy. Therefore, these are considered “good” carbs because they provide a more even distribution of energy for the body to use during activity. They cause a more consistent and gradual release of sugar into the blood stream (as opposed to peaks and valleys caused by simple carbs) and provide energy to function throughout the day. Additionally, “good” carbs have the added benefit of providing vitamins, fiber, and minerals that are missing from simple carbs.
Remember that carbohydrates fuel the body and are an important source of energy, especially for active and athletic people. However, carefully selecting the type of carb you eat is critical to peak function and performance.
Simple carbs taste great (according to our modern brain raised on simple sugars) and are easy to break down into a quick source of energy. However, the sensation of hunger is quick to return because the sugar is released and used up in the body quickly, giving the sensation of needing more.
Simple carbs are often “refined” and therefore stripped of their fiber, vitamins and minerals, which is why they are often referred to as “empty” calories.
Simple carbs lead to rapid spikes in blood sugar and insulin levels after meals. When these levels are not controlled over time, it can lead to obesity, which is ultimately related to adult-onset diabetes and high blood pressure.
Sources: www.everydayhealth.com; www.yourdictionary.com; Mayo Clinic
Visit your doctor regularly and listen to your body

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Spring is in the air. The temps are rising and the days are longer, so get outside and walk! Walking can change the world…from Mahatma Gandhi and the Indian independence movement to Martin Luther King, Jr., and the civil rights movement, walking and protest have been interrelated. Moreover, walking has been associated with fostering good health and stimulating creativity.
Walking is about more than walking and always has been. Walking soothes. Walking inspires and sharpens the mind. WE CAN WALK!
It might be said that with the right mindset, every walk is a pilgrimage. Many breakthroughs has been stumbled upon while putting one foot in front of the other. We run from problems. We walk toward solutions. While working on A Christmas Carol, Charles Dickens would walk 15 or 20 miles through the back streets of London, turning over the plot in his mind as the city slept. Beethoven found inspiration while ambling in the verdant Wienerwald outside Vienna.
Recent studies suggest that walking stimulates our creative mind is at its most creative at three miles per hour, the speed of a moderately paced stroll. Stanford University researchers divided participants into two groups: walkers and sitters. They then administered a test designed to measure creativity. They found that creative thinking was “consistently and significantly” higher for the walkers than the sitters. It didn’t take a lot of walking to boost creativity, either—anywhere from 5 to 16 minutes.
Studies have also shown that people who walk regularly are healthier and live longer than those who don’t. Surprisingly, you don’t have to walk very fast or far to enjoy this benefit. One recent study, published in JAMA Internal Medicine, put the 10,000-step myth to rest. It is an arbitrary number. People—older adults in particular—accrue health benefits by taking only a few thousand steps each day, and at a leisurely pace.
In addition to stimulating creativity and reducing stress, walking has many benefits. “There’s no question that increasing exercise, even moderately, reduces the risks of many diseases, including coronary heart disease, breast and colon cancer, and Type 2 diabetes,” said Dr. Jennifer Joyce, MD, professor of family medicine at GCSOM. “Research has even shown that you could gain two hours of life for each hour that you exercise regularly.”
According to the American Heart Association, walking as little as 30 minutes a day can provide the following benefits:
Like everything, there is a right way of doing something, even walking. For efficiency and safety, walking with proper stride is important. A fitness stride requires good posture and purposeful movements. Ideally, here's how you'll look when you're walking:
Anything is better than nothing! However, for most healthy adults, the Department of Health and Human Services recommends at least 150 minutes of moderate aerobic activity or 75 minutes of vigorous aerobic activity, or an equivalent combination of moderate and vigorous aerobic activity. The guidelines suggest that you spread out this exercise during the course of a week. Also aim to do strength training exercises of all major muscle groups at least two times a week.
As a general goal, aim for at least 30 minutes of physical activity a day. If you can't set aside that much time, try several short sessions of activity throughout the day. Even small amounts of physical activity are helpful, and accumulated activity throughout the day adds up to provide health benefits.
Remember it's OK to start slowly — especially if you haven't been exercising regularly. You might start with five minutes a day in the first week and then increase your time by five minutes each week until you reach at least 30 minutes.
For even more health benefits, aim for at least 60 minutes of physical activity most days of the week.
Keeping a record of how many steps you take, the distance you walk and how long it takes can help you see where you started from and serve as a source of inspiration. Record these numbers in a walking journal or log them in a spreadsheet or a physical activity app. Another option is to use an electronic device such as a pedometer or fitness tracker to calculate steps and distance.
Sources: National Geographic; Mayo Clinic
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

Germaphobes, cleaning zealots, neat freaks, and those with diagnosed or undiagnosed obsessive-compulsive disorder (OCD), this column is for you! If you would rather clean your bathroom floor than go for a walk on a beautiful sunny day, please read on. If you use a toothbrush on tile grout on a regular basis and take pride in the sparkle of your toilet bowl than beware… studies show that performing these tasks with too much vigor and passion might lead to back, neck, and shoulder and wrist pain.
For some, and you know who you are, (I am related to a few) spring cleaning can be a particularly exciting sporting event. It is almost an exorcism to rid a home of all its evil spirits, smudges, dust, dirt, germs, and odors. Every April curtains come off the windows to be washed and carpets rolled up, removed and cleaned. The surfaces under the curtains and carpets are sterilized with cleaning detergents, disinfectants and chemicals that would make sterile techniques in most hospital operating rooms seem inadequate. And that doesn’t include the heavy work: moving furniture, bedding, including mattresses and box springs.
As a physical therapist and survivor of childhood exposure to copious amounts of cleaning chemicals, I have come to learn that there are healthy and safe options for spring cleaning your home. Of course, the most obvious solution is to hire professional help if you can afford it. The other practical solutions are below:
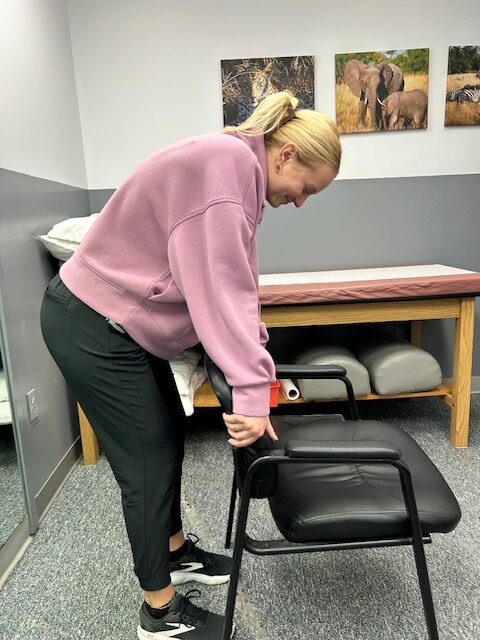 Incorrect
Incorrect 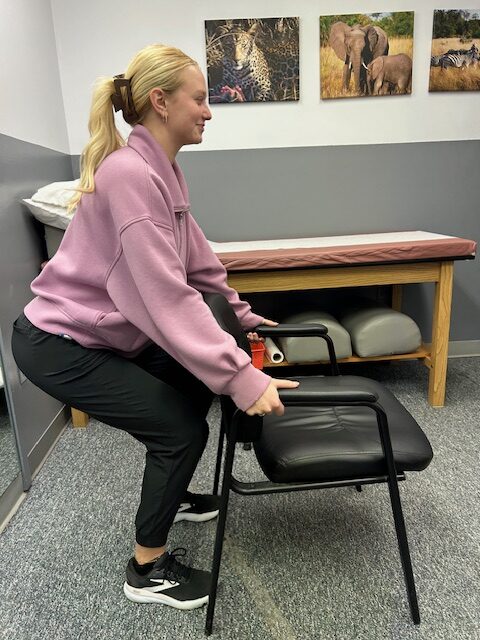 Correct
Correct Incorrect
Incorrect  Correct
Correct
Model: Hannah Keane, Physical Therapy Aide, Mackarey PT
Sources: National Center for Injury Prevention and Control at the CDC, www.medicinenet.comwww.household-management-101

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!

“Everybody talks about the weather, but nobody does anything about it,” said Mark Twain. Just ask 93% of the arthritis sufferers who believe that the weather affects their pain level. History tells us that Benjamin Franklin, Leonardo da Vinci, and Christopher Columbus also felt this way about the weather.
Patients at our clinic have been particularly sensitive to joint pain on cold, damp days, especially during the past few weeks. In my clinical practice of orthopedic and sports physical therapy, an informal survey found that 95 out of 100 patients (95%) with arthritis reported increased pain with weather changes. While most people report that the coldness and dampness seem to irritate their joints, they also report more pain with weather changes in the summer. There is a reasonable explanation…
Joints in the body have a lining called synovium that secretes a lubricating fluid called synovial fluid. In joints with arthritis, there is an overproduction of synovial fluid. In theory, when the barometric pressure changes, so to will the pressure inside your joints, especially if it is already overfull with extra fluid from arthritis. This added pressure stimulates the nerve endings in the joint to produce inflammation and pain.
Despite this overwhelming response from patients, scientific studies vary in their support of this claim. According to the Mayo Clinic, in 1961, a famous arthritis doctor (rheumatologist), built a climate chamber and discovered that when high humidity was combined with low barometric pressure, patients reported increased joint pain and stiffness. A recent study found that changes in barometric pressure and cooler temperatures are associated with joint pain. However, other studies have found increased joint pain with high barometric pressure in both warm and cold weather while another study found pain with low pressure.
What does this mean? It means that patients with arthritis consistently report pain with weather changes, but science has not found an accurate method to consistently support these claims. Some of these inconsistencies may be attributed to the fact that there are differences in sensitivity among individuals. For example, some patients have symptoms before the weather changes, while others notice symptoms during or after the weather changes. Still yet, some report more pain in colder conditions while others notice more pain in warmer weather. It appears that changes in the weather, such as a high to a low or warm dry to cold damp and vice versa is the culprit when it comes to irritating arthritis in a joint.
If I have arthritis, should you move to Arizona? Yes and no! Yes, the warm and dry climate of Arizona will probably make you feel better overall. However, it will not cure the degenerative changes in your joints, and you may still have pain when CHANGES in the weather occur. This is proven to be true by the fact that there are many very busy rheumatologists in Arizona!
In conclusion, it is safe to say that there is some evidence to support the claim that most patients with arthritis have increased symptoms of joint pain and stiffness with CHANGES in the weather:
Therefore, each patient must be individually evaluated by their physician to determine the extent of their arthritis and its relationship to the changes in the weather. While the cause of their increased symptoms with changes in the weather may not be completely understood, each patient must determine the adjustments in their lifestyle and/or medications according to the particular weather patterns that affect their problem most.
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!


Guest Author: Gretchen Welby, PharmD, MHA
Gretchen graduated from Philadelphia College of Pharmacy and Science, The University of Scranton, and received a Doctor of Pharmacy degree from Temple University.
Gretchen has been teaching for over 25 years at Rutgers University, Keystone College, Lackawanna College, The University of Scranton, and Marywood University. She has earned certifications in Pilates, yoga, barre and teaches all three locally. She has a Wellness and Lifestyle coaching certification from Harvard University.
Gretchen resides in Scranton with her husband, Timothy Welby, MD, and has three daughters – Casey, Kate, and Caroline.
I have invited Gretchen Welby, PharmD, MHA to present the current wisdom on the very controversial topic of vaccination/immunization to raise awareness and dispel any myths and misunderstandings.
Scientific progress has rarely advanced by popular vote, and vaccination is no exception. While public sentiment deserves respect and thoughtful engagement, the evidence guiding immunization policy is built on decades of rigorous research, transparent testing and continuous review. These research processes are designed precisely to rise above fear, trend, politics or misinformation. Choosing to prioritize scientific findings over shifting opinion is not an act of dismissal, but of responsibility…it is a commitment to decisions that protect both individual lives and the collective good, even when those decisions challenge what feels comfortable or widely believed.
2024 marked the 50th anniversary of the World Health Organization’s Expanded Programme on Immunization (EPI). An initiative to make life-saving vaccines available to all worldwide. A modeling study done to mark the 50 years of EPI estimated that vaccination averted 154 million deaths, including 146 million deaths among children. Several additional studies on vaccine effectiveness show that vaccines improve infant safety, contribute to a healthy society, and even reduce cancer risk. Vaccines work for an individual and society. The data show that many vaccines can reduce mortality by 99% or more. Unfortunately, global immunization has been a victim of its own success because people have forgotten how deadly and dangerous the diseases vaccines protect against can be.
Vaccine effectiveness is overshadowed today by misinformation about vaccine safety, changing vaccine administration timelines, and mixed public health messaging. What are the outcomes of the recent relaxed vaccine message? The number of measles cases has jumped. Fifty-nine cases were reported in 2023. In 2025, 2242 cases were reported. For additional perspective, an article published in the 2007 edition of JAMA listed the number of deaths pre-vaccine release and the number of deaths post-vaccine release. The findings are remarkable.
The recent Centers for Disease Control and Prevention (CDC) change to the childhood vaccine schedule reduces routine protection against 13 childhood diseases to 7, with shared decision-making now required for the remaining 6. Diphtheria, tetanus, acellular pertussis (DTaP; Tdap), Haemophilus influenzae type b (Hib), Pneumococcal (PCV), Inactivated poliovirus (IPV), Measles, mumps, rubella (MMR), Varicella (VAR), and Human papillomavirus (HPV – changing from 2 doses to 1 dose) are now part of the routine vaccine schedule.
Rotavirus, COVID-19, Influenza, Hepatitis A, Hepatitis B, Meningococcal ACWY, and Meningococcal B are now grouped in a shared-decision-making model. Traditionally, when changes are made to the vaccine schedule, they are made with much deliberation, study, and expert input from multiple agencies and governing bodies. However, this recent change, however, did not follow the normal study path. This is concerning because changes are proposed without proper study of the immediate and long-term consequences.
Vaccines have been shown to be safe, with most patients experiencing very minor side effects. Normal reactions from vaccinations include low-grade fever for 24-48 hours. A low-grade fever and minor muscle aches signal the body's immune response. Tenderness and redness at the injection site are other normal reactions from immunization and should last from 24-48 hours. There is no proof that thimerosal (a preservative historically used in vaccines) causes adverse reactions. Additionally, thimerosal has been removed from most vaccine preparations used today. Vaccines do not overwhelm a child’s immune system. Children are exposed to hundreds of antigens daily. A WHOLE pediatric vaccination schedule exposes them to around 50 antigens. There is NO evidence to support altering or delaying the American Academy of Pediatrics vaccination schedule. This does NOT increase safety; it DECREASES protection at a time when infants and children are most vulnerable.
How can consumers of healthcare information, in particular, vaccine information, find reliable, trustworthy, educated guidance? Since the June 2025 changes in CDC personnel have resulted in less qualified members of the Advisory Committee on Immunization Practices (ACIP), it is generally best to rely on non-governmental sources such as the American Academy of Pediatrics, American College of Gynecologists, the Infectious Disease Society of America, and the Vaccine Integrity Project for vaccine advice. Additionally, discuss vaccine efficacy and safety with your doctor.
For More Information:
Vaccination greatly reduces disease, disability, death and inequity worldwide - PMC
The New Federal Vaccine Schedule for Children: What Changed and What Are the Implications? | KFF
JAMA 2007; 298:2155-2162
Visit your doctor regularly and listen to your body.

EVERY MONDAY – Read Dr. Paul J. Mackarey “Health & Exercise Forum!” via Blog
EVERY SUNDAY in "The Sunday Times" - Read Dr. Paul J. Mackarey “Health & Exercise Forum!” in hard copy
This article is not intended as a substitute for medical treatment. If you have questions related to your medical condition, please contact your family physician. For further inquires related to this topic email: drpmackarey@msn.com
Paul J. Mackarey PT, DHSc, OCS is a Doctor in Health Sciences specializing in orthopedic and sports physical therapy in Scranton and Clarks Summit. Dr. Mackarey is in private practice and is an associate professor of clinical medicine at Geisinger Commonwealth School of Medicine. For all of Dr. Mackarey's articles, visit our exercise forum!